Ultrasonographic Occiput Position in Early Labor in the Prediction of Cesarean Section
Ultrasonographic Occiput Position in Early Labor in the Prediction of Cesarean Section
Abstract & Commentary
Synopsis: The occiput posterior relationship with Cesarean section is worth exploring.
Source: Akmal S, et al. BJOG. 2004;111:532-536.
An enlightening article recently appeared in the British Journal of Obstetrics and Gynaecology by Akmal and colleagues. They performed sonograms in 601 women in active labor to assess the position of the fetal head as it entered the maternal pelvis. Using the simple end point of Cesarean section, they then folded in a variety of other variables, such as maternal age, parity, maternal height, ethnicity, fetal gender, gestational age, and whether labor was spontaneous or induced.
Eighty-seven patients had Cesarean sections (14%) in the study. A major difference in Cesarean section rates (CSR) was noted between those with occiput posterior positions in early labor (19%) and those with other cephalic positions (11%). The variables most associated with Cesarean section are outlined in the Table below, lifted directly from the paper.
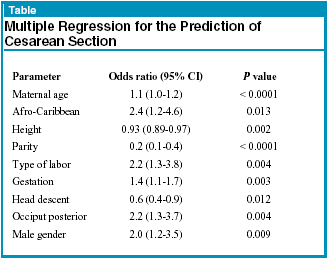
Most of the indicators are not surprising, but some are, such as fetal sex. Akmal and colleagues then developed a scoring system based on the above variables and came up with a probability score for an individual entering labor. Interestingly, 337 patients (63%) had low scores (below a preset threshold), and their positive predictive value for Cesarean section was 4%. However, the remaining 224 (37%) who had scores above this threshold had CSR’s between 32% for the lower score and 56% for the highest.
Comment by John C. Hobbins, MD
At first, I thought there was nothing new in this study, and the idea of rating a patient’s chances of a successful vaginal delivery (ahead of time) is not new and, in fact, has been very recently revisited.1 However, the addition of assessment of head position through ultrasound is a new wrinkle and, using the variables published in this article, the CSR in those with low scores (making up the majority of patients) was only 4%.
Akmal et al explain the increased odds ratios for the variables in various ways and cite literature to support their reasons. For example, short mothers and those of Afro-Caribbean ancestry tend to have smaller or non-gynecoid pelves. Older women have uteri that need more oxytocic help and their providers tend to have a lower bail out threshold for them. Multiparas require less uterine effort to accomplish early cervical dilation, and induced labors have always had a higher CSR, probably because the uterus is not ready for labor, coupled with the reasons for the induction in the first place.
The factor that is not as easy to explain is the 2-fold higher CSR for male fetuses. Akmal et al reference a study showing that male fetuses have a lowered ability to release catecholamines in response to fetal hypoxia/acidosis, and therefore, are more susceptible to fetal distress.2 This one I have trouble swallowing, especially since there is no evidence in the paper for a higher CSR for fetal compromise in male fetuses.
The occiput posterior relationship with Cesarean section is worth exploring. There is evidence that persistent occiput posteriors result more frequently from the relationship between the occiput and the pelvic inlet, rather than from an inherent inability to rotate during passage through the midpelvis. That would mean that the die is cast early, rather than late.
Now—what do we do with this information in clinical practice? First, those with low probabilities for Cesareans should be given every chance for a vaginal delivery short of fetal compromise. Also, those with a high probability for Cesarean section should have an opportunity to have a vaginal delivery, but if they fall off the labor curve at any time along the way, it might be judicious to avoid postponing the inevitable.
Akmal et al made a pitch for a Dublin-like approach of active management of labor in those patients with a high probability for Cesarean, and cite a recent randomized clinical trial (RCT) showing a benefit from this approach. However, although it may make sense to make a short but aggressive try at vaginal delivery, some RCTs have not validated the active management of labor approach, and the study cited did not address specifically patients with high probabilities for Cesarean sections.3-6
Last, using ultrasound to assess the position of the fetal occiput in early labor should yield important adjunctive information in later decision making.
References
1. Wilkes PT, et al. Obstet Gynecol. 2003;102:1352-1357.
2. Souka AP, et al. J Maternal Fetal Neonatal Med. 2003; 13:59-63.
3. Main DM, et al. Am J Obstet Gynecol. 2000;182: 1312-1320.
4. Rossavik IK. Am J Obstet Gynecol. 1980;136:579-583.
5. Lieberman E, et al. Am J Obstet Gynecol. 1997;176: 667-671.
6. Pattinson RC, et al. Br J Obstet Gynaecol. 2003;110: 457-461.
John C. Hobbins, MD, Professor and Chief of Obstetrics, University of Colorado Health Sciences Center, Denver, is Associate Editor for OB/GYN Clinical Alert.
An enlightening article recently appeared in the British Journal of Obstetrics and Gynaecology by Akmal and colleagues. They performed sonograms in 601 women in active labor to assess the position of the fetal head as it entered the maternal pelvis. Using the simple end point of Cesarean section, they then folded in a variety of other variables, such as maternal age, parity, maternal height, ethnicity, fetal gender, gestational age, and whether labor was spontaneous or induced.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
