ECG Review: Adenosine for a Wide Tachycardia?
ECG Review: Adenosine for a Wide Tachycardia?
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
This article originally appeared in the June 15, 2012, issue of Internal Medicine Alert. It was edited by Stephen Brunton, MD, and peer reviewed by Gerald Roberts, MD. Dr. Brunton is Adjunct Clinical Professor, University of North Carolina, Chapel Hill, and Dr. Roberts is Assistant Clinical Professor of Medicine, Albert Einstein College of Medicine, New York, NY. Dr. Brunton serves on the advisory board for Lilly, Boehringer Ingelheim, Novo Nordisk, Sunovion, and Teva; he serves on the speakers bureau of Boehringer Ingelheim, Lilly, Kowa, Novo Nordisk, and Teva. Dr. Roberts reports no financial relationship to this field of study.
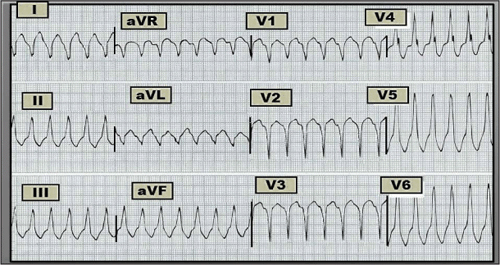
Figure — 12-lead ECG obtained from a 30-year-old man with palpitations.
Scenario: The 12-lead ECG shown above was obtained from a previously healthy 30-year-old man who presented to the emergency department with new-onset palpitations. No prior ECG was available for comparison. The patient was alert and hemodynamically stable at the time this tracing was recorded. What is the rhythm? Is this rhythm likely to respond to adenosine?
Interpretation: The rhythm is rapid and regular at a rate of ~180/minute. The QRS complex is obviously wide. No P waves are seen. Thus, the rhythm is a regular wide-complex tachycardia (WCT) without clear sign of atrial activity. Ventricular tachycardia (VT) must be assumed until proven otherwise!
Clinical management of sustained VT depends on the clinical setting in which it occurs. If no pulse is present, the rhythm is treated the same as for ventricular fibrillation — with immediate unsynchronized countershock. If a pulse is present but the patient is unstable (i.e., hypotensive, short of breath, having chest pain), then immediate synchronized cardioversion is in order. On the other hand, if the patient is hemodynamically stable and tolerating the rhythm (as in this case), there is at least a moment of time to contemplate management. A trial of antiarrhythmic therapy (with amiodarone, procainamide, or other antiarrhythmic agent) is in order — keeping in mind that the patient should be cardioverted if decompensation occurs at any time during the process.
Much has been written about the role of adenosine in the management of a stable patient with either VT or a regular WCT of uncertain etiology. If (as may occur on occasion) the WCT is supraventricular with preexisting bundle branch block or aberrant conduction, adenosine may convert the rhythm. Because of the ultra-short half-life of this drug (less than 10 seconds!), any adverse effects that may result from adenosine are usually short-lived. The important clinical point to appreciate is that a small but significant percentage of VT rhythms are adenosine-responsive! The reason for this is uncertain, but thought to relate to adenosine receptor inhibition of adenylate cyclase, as well as modulation in autonomic tone. The most common adenosine-responsive form of VT originates from the right ventricular outflow track (RVOT). Clinically, this most often occurs in otherwise healthy young adults without structural heart disease. Episodes of VT are often related to catecholamine release, and therefore commonly occur with exercise or stress. The ECG picture of RVOT VT is distinctive: The QRS is wide with a left bundle branch block pattern in the precordial leads and a superior axis in the limb leads (as in the Figure). Other forms of adenosine-responsive VT may not be distinguishable from non-responsive forms. The patient with RVOT VT should be referred for electrophysiologic study following conversion of the acute rhythm disturbance. By way of perspective, it is important to emphasize that most VT will not be adenosine-responsive. Nevertheless, it is well to be aware that some VT will respond to this drug, which provides an additional rationale for considering a trial of adenosine when confronted with a stable patient who presents in either VT or a WCT of uncertain etiology.
Scenario: The 12-lead ECG shown above was obtained from a previously healthy 30-year-old man who presented to the emergency department with new-onset palpitations. No prior ECG was available for comparison. The patient was alert and hemodynamically stable at the time this tracing was recorded. What is the rhythm? Is this rhythm likely to respond to adenosine?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
