The Joint Commission and the FDA take steps to curb adverse events related to the use and misuse of opioid drugs
The Joint Commission and the FDA take steps to curb adverse events related to the use and misuse of opioid drugs
Emergency departments face unique challenges in treating patients who present with pain
Noting that opioid analgesics are among the drugs most often associated with adverse drug events, the Joint Commission has issued a Sentinel Alert, urging hospitals to step up their efforts to prevent complications and deaths from use of these powerful drugs. At the same time, the Food and Drug Administration (FDA) has launched an opioid safety plan that requires the manufacturers of extended-release and long-acting opioids to fund continuing education programs for physicians and others who prescribe these drugs. The training sessions, which are scheduled to begin in March of 2013, will be voluntary, but the FDA estimates that within three years of implementing the education program, at least 60% of the 32,000 health professionals who prescribe the drugs will have received the opioid training.
These moves come amid growing alarm that patients are being harmed because of dosing errors, improper monitoring, and dangerous drug interactions associated with opioids such as morphine, oxycodone, and methadone. The Joint Commission reports that of the opioid-related adverse events reported by hospitals to the accrediting agency between 2004 and 2011, 47% involved wrong-dose medication errors, 29% pertained to improper patient monitoring, and 11% were attributed to factors such as excessive dosing, interactions with other drugs, and adverse reactions. Also, according to the FDA, close to 16,000 Americans died from overdoses involving opioids in 2009, and in 2011, nearly 23 million prescriptions for extended-release and long-acting opioids were dispensed in the United States.
The Joint Commission stresses that while some patients require opioids to manage their pain, use of these drugs can slow breathing to dangerous levels and can cause other problems as well such as dizziness, nausea, and falls. Further, while the Sentinel Alert focuses primarily on opioid use among hospitalized patients, the agency observes that EDs have unique challenges with regard to opioid use that also should be addressed.
ED visits involving misuse, abuse of drugs are way up
Indeed, the latest report from the Drug Abuse Warning Network (DAWN), issued in July 2012, notes that ED visits involving the misuse or abuse of pharmaceuticals increased by a whopping 115% between 2004 and 2010, and ED visits involving adverse reactions to pharmaceuticals taken as prescribed increased by 86% between 2005 and 2010. (See Figure 1.) While only a portion of these adverse reactions are related to opioids, many experts agree that opioids are of particular concern.
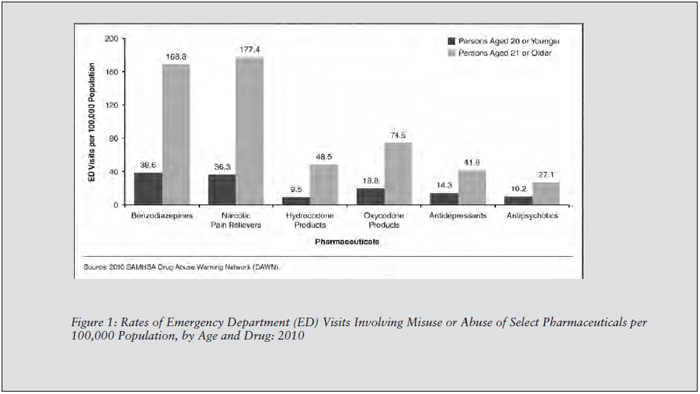
The American College of Emergency Physicians (ACEP) released a clinical policy paper on opioid prescribing in the ED earlier this year, and some individual states are taking on the issue as well. For example, in Washington state, an ED opioid abuse work group recently unveiled guidelines on opioid prescribing that have been disseminated to every ED in the state, explains Stephen Marshall, MD, medical director of the ED at Overlake Hospital Medical Center in Bellevue, WA, and president of the Washington chapter of ACEP. (See Source for links to ACEP paper and W-ACEP guidelines, below.)
The guidelines were prompted by data showing that there is a high number of accidental deaths related to prescription medications in the state, observes Marshall, but he emphasizes that the problem is not an easy one to solve. "This is a bit of a dilemma for emergency physicians. A significant portion of our practice is to try to relieve pain and to do so in a timely and humane way, and yet, we understand with more and more education that in patients who do receive narcotic medications or opioids, that we may be creating a secondary problem while we are trying to relieve their initial problems," says Marshall.
The guidelines don't prevent physicians from treating their patients in the way they think is best, but rather set up a support structure that helps them to have conversations with their patients about appropriate care, explains Marshall. (See also "To improve opioid prescribing practices, enlist the support of state-level agencies," below.)
Time to institute photo IDs?
Among the recommendations spelled out in the document, the guidelines discourage the administration of intravenous and intramuscular opioids in the ED for the relief of chronic pain, and they stress that long-acting or controlled-release opioids should not be prescribed at all in the ED setting.
Further, the guidelines suggest that EDs should photograph patients who present with complaints of pain without a government-issued ID. "Everybody has anecdotal stories of people taking someone's insurance card and showing up and pretending to be that person, and getting prescriptions or getting health care in a fraudulent way," says Marshall. "This helps to avoid that."
This practice should also help to prevent people from going to multiple EDs to access prescriptions for narcotics that they can then re-sell or divert, adds Marshall. "These people are not necessarily the users of the drugs, so we would like to eliminate this practice completely because it is a danger to society," he says. "Probably half of the prescription narcotic deaths that are reported involve people taking drugs that were not actually prescribed to them. The drugs were either diverted or taken out of a parent's or friend's medicine cabinet, so we are trying our best to reduce this."
Having a photo ID program in the ED is one way to address this problem, but it is only a first step, says Marshall. The next step is having pharmacists require a photo ID when patients pick up their prescriptions, he says.
Other recommendations in the guidelines are designed to address patients who present to the ED to receive narcotics for relief of chronic pain. "There is significant evidence that narcotics or opioids aren't very good at treating chronic pain, even though we have many people going down that pathway," says Marshall. "We want to give them hope and help them switch to medications that are safer and more likely to work better for them."
Marshall adds that posters summarizing the pain medication prescribing policies advocated in the guidelines have been posted in every ED in the state so that patients will understand what they can expect if they present to an ED for pain, and why the policies are in place.
Physicians adjust prescribing practices
For the past 15 months, hospitals in Washington have been under intense legislative pressure to reduce non-emergent ED visits, so practices that reduce drug-seeking behavior should assist in this effort, although development of the opioid guidelines began long before the legislature began cracking down on ED visits, explains Marshall. "The timing was fortuitous in helping us to show that we could offer an alternative solution to the legislature's rather draconian, non-clinical intervention of trying to limit visits," he says. "We were able to show them that we had been working on this for two years with other state agencies and that we already had a plan in place."
The opioid guidelines have only been in place for about a year at this point, so it is difficult to gauge what impact they will have, but Marshall indicates that preliminary data show that the number of prescription opioid-related accidental overdoses seems to be decreasing. "The bad news is that the number of heroin-related accidental deaths seems to be increasing, so part of this process may be pushing addicted people who don't want help to other sources for their narcotics, but it is too soon to make that judgment," says Marshall.
However, there is also evidence that ED physicians are adjusting their prescribing practices. "What I can tell you from my practice and my partner's practice is that we are writing fewer prescriptions and we are talking to patients about the risk of addiction when we are giving narcotics for acute pain relief," says Marshall. "If a patient comes in with a broken ankle, there is some evidence that opioid narcotics do well in combination with Tylenol or ibuprofen, so we are going to prescribe them for that, but we are also going to try to prescribe less than we might have, we are going to try to make sure the patient gets careful follow-up, and we will warn people about the risks of narcotics or opioid prescriptions left in their medicine cabinets and not taken."
Be careful with drug-drug interactions, methadone
Lynn Webster, MD, FACPM, FASAM, president-elect of the American Academy of Pain Medicine, and Medical Director, Lifetree Clinical Research and Pain Clinic, Salt Lake City, Utah, welcomes the FDA's initiative aimed at providing physicians with more education about how to prescribe extended-release and long-acting opioids because he believes many physicians lack understanding of how to identify patients who are most likely to be vulnerable from the use of these drugs. In addition, Webster notes that some physicians don't know how to properly initiate some of these medicines, or how to rotate from one type of opioid to another safely. "Sometimes physicians are unaware of drug-drug interactions, and some will use medicines that are inappropriate for the emergency setting," adds Webster.
Another problem that Webster sees in ED settings is that in the case of acute trauma-related pain, physicians often prescribe more medicine than is necessary. For example, a patient who presents to the ED with a legitimate pain complaint may receive a prescription for a week or two of pain medication when he only needs the medicine for one or two days, explains Webster. "The unused medicine then becomes available for diversion," he says.
Webster contends that physicians in the ED should not even be prescribing long-acting or extended-release opioids because the ED is an acute setting. "If an extended-release opioid is needed, then it should be prescribed by someone who is going to follow the individual for a long time," he says. "It is just not appropriate to use extended-release or long-acting opioids for acute pain, particularly in patients who may be opioid naïve."
One drug-drug combination that ED physicians should be careful to avoid is the use of opioids and benzodiazepines. "There is significantly more toxicity to both drugs — the benzodiazepine and the opioid — when they are prescribed in combination," explains Webster.
Physicians in the ED should also be careful about how they use methadone, a drug that is increasingly being used as a narcotic pain reliever because many payers are declining to cover branded drugs, observes Webster, but he emphasizes that it is a risky choice.
"One-third of the opioid deaths in this country are due to methadone, and many of those are due to an inappropriate starting dose," he says. "My guideline is never to start anyone on more than 15 milligrams of methadone, even though the package insert states that you can start someone on up to 30 milligrams. Sometimes 30 milligrams is lethal."
With the increasing use of methadone as a pain reliever, there has been a huge increase in ED visits related to the non-medical use of the drug, according to a DAWN report covering the years 2004 to 2009. (See Figure 2, below.) These would pertain to patients who took more of the drug than prescribed, patients who took methadone prescribed to someone else, deliberate poisoning, or documented misuse or abuse of the drug.
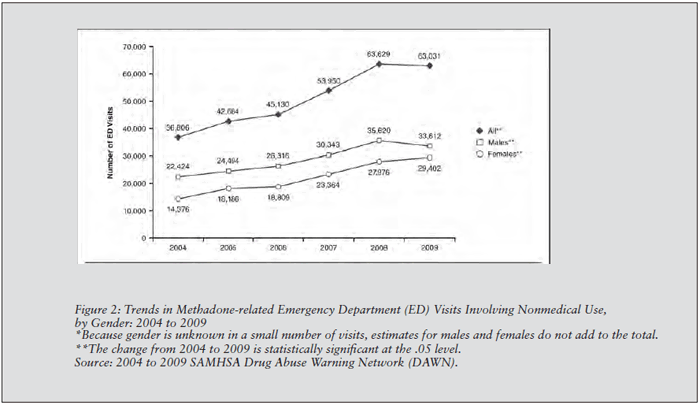
Joint Commission: Take these steps
The Joint Commission is urging hospitals to implement practices designed to ensure that patients receiving opioids are regularly monitored and that pain management experts are consulted to review pain management plans. The agency also encourages the use of technology to enhance safety in opioid prescribing, and it recommends additional training and education on the safe use of opioids for both clinicians and patients. Other steps that hospitals should consider include using standardized tools to screen patients for any risk factors that could heighten the possibility of adverse events from opioid use, and the tracking of any opioid-related incidents.
Sources
- The American College of Emergency Physicians (ACEP) issued a clinical policy paper on opioid prescribing in the ED in June 2012. To review the paper, "Critical Issues in the Prescribing of Opioids for Adult Patients in the Emergency Department," visit the ACEP website at: http://www.acep.org/clinicalpolicies.
- The Washington State Chapter of the American College of Emergency Physicians collaborated with other state agencies to develop Washington Emergency Department Opioid Prescribing Guidelines. They can be accessed at http://washingtonacep.org/Postings/edopioidabuseguidelinesfinal.pdf.
- Stephen Marshall, MD, Medical Director, Emergency Department, Overlake Hospital Medical Center, Bellevue, WA, and President, Washington Chapter, American College of Emergency Physicians. E-mail: [email protected].
- Lynn Webster, MD, FACPM, FASAM, President-Elect, American Academy of Pain Medicine, and Medical Director, Lifetree Clinical Research and Pain Clinic, Salt Lake City, Utah. E-mail: [email protected].
Improve ED opioid prescribing practices by enlisting support of state-level agencies To effectively tackle the issue of opioid prescribing practices in the ED, you will need the support of physician and nurse champions in high places, but you should also try to enlist the participation of state-level agencies such as the health department, the hospital association, and medical association, advises Steven Marshall, MD, medical director of the ED at Overlake Hospital Medical Center in Bellevue, WA, and president of the Washington chapter of the American College of Emergency Physicians (W-ACEP). These groups can not only help you win buy-in for the effort, they may also provide some financial support. In Washington, for example, state agencies picked up the tab for printing posters so that every ED in the state could prominently display how patients presenting to the ED with pain will be treated, and why these policies were implemented. "The state was going to take [W-ACEP] money for that, and then they just decided to step up and do it," says Marshall. "It was a big deal having the state be on board with the effort." |
Noting that opioid analgesics are among the drugs most often associated with adverse drug events, the Joint Commission has issued a Sentinel Alert, urging hospitals to step up their efforts to prevent complications and deaths from use of these powerful drugs.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.

