Antiretroviral Prophylaxis After Nonoccupational Exposure to HIV
Antiretroviral Prophylaxis After Nonoccupational Exposure to HIV
Abstract and Commentary
Synopsis: Postexposure prophylaxis (PEP) with effective antirtrovirals should be instituted within 72 hours substantial nonoccupational exposure to HIV.
Source: CDC Antiretroviral postexposure prophylaxis after sexual, injection drug use, or other nonoccupational exposure to HIV in the United States. MMWR 2005; 54(RR02):1-20. Available at www.cdc.gov/mmwr/preview/mmwrhtml/rr5402a1.htm
The CDC published its first recommendations for management of exposure to HIV in the occupational setting in 1990, at a time when the only available antiretroviral was zidvudine.1 They first addressed the issue of non-occupational exposure in print in 1998, at which time they, however, concluded that the available evidence for or against post-exposure prophylaxis (PEP) in this setting was inadequate to allow them to make a recommendation applicable to the United States.2 Since then, a great deal of information has become available.
Data from animal and human studies provide clear evidence that the initiation of antiretroviral therapy within 48 to 72 hours after nonoccupational exposure to HIV is likely to reduce the risk of transmission. This document considers a nonoccupational exposure to be "any direct mucosal, percutaneous, or intravenous contact with potentially infectious body fluids that occurs outside perinatal or occupational situations (eg, health-care, sanitation, public safety, or laboratory employment). Potentially infectious body fluids are blood, semen, vaginal secretions, rectal secretions, breast milk, or other body fluid that is contaminated with visible blood."
They recommend prompt institution of PEP within 72 hours after such exposures when the source is known to be HIV infected and the exposure is substantial (see Figure 3). The estimated risks of various exposures are listed in Table 1, below.
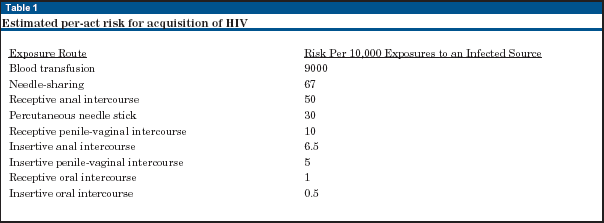
In cases in which the HIV status of the source is unknown, PEP is not recommended, but clinicians and patients are encouraged "to weigh the risks and benefits on a case-by-case basis." In addition, in instances in which patients seek care more than 72 hours after substantial exposure, clinicians might consider prescribing PEP "if, in their judgment, the diminished potential benefit of PEP outweighs the potential risk for adverse events from antiretroviral medications." In any case, individuals seeking evaluation should be provided counseling in risk-reduction and any other intervention services that are indicated in order to reduce the likelihood of future exposures.
The CDC recommends, as preferred PEP regimens, one of the following:
- Efavirenz plus either lamivudine or emtricitabine plus either zidovudine or tenofovir.
- Lopinavir/ritonavir (Kaletra®) plus either lamivudine or emtricitabine plus zidovudine. PEP should be administered for 28 days.
The potential teratogenicity of efavirenz precludes its use in pregnancy and in women of childbearing age at risk of pregnancy. When efavirenz is prescribed to women of childbearing potential, they should be instructed about the need to avoid pregnancy.
In practice, decisions concerning the level of risk are often quite difficult. A good practice in such circumstances, it seems to me, is to initiate PEP and then reevaluate. PEP can always be discontinued if a conclusion is reached that the risk of exposure was negligible.
References
1. CDC. Public Health Service statement on management of occupational exposure to human immunodeficiency virus, including considerations regarding zidovudine postexposure use. MMWR. 1990; 39(RR01):1-14.
2. CDC Management of Possible Sexual, Injecting Drug-Use, or Other Nonoccupational Exposure to HIV, Including Considerations Related to Antiretroviral Therapy: Public Health Service Statement. MMWR. 1998;47:No. RR-17).
The CDC published its first recommendations for management of exposure to HIV in the occupational setting in 1990, at a time when the only available antiretroviral was zidvudine. They first addressed the issue of non-occupational exposure in print in 1998, at which time they, however, concluded that the available evidence for or against post-exposure prophylaxis (PEP) in this setting was inadequate to allow them to make a recommendation applicable to the United States.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
