ECG Review: A CVA to be Anticoagulated?
By Ken Grauer, MD, Professor and Associate Director, Family Practice Residency Program, Department of Community Health and Family Medicine, College of Medicine, University of Florida, Gainesville. Dr. Grauer is on the Editorial Board of Emergency Medicine Alert.
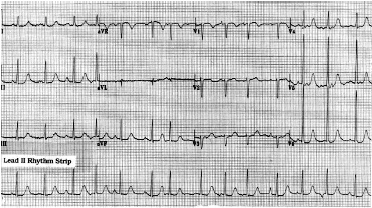
Figure: 12-lead ECG and rhythm strip obtained from an elderly woman with an acute stroke. Should the patient be anticoagulated?
Clinical Scenario: The electrocardiogram (ECG) and rhythm strip in the Figure were obtained from an elderly woman admitted for an acute stroke. Her neurologic deficit was not progressing, and she was clinically stable at the time of admission to the hospital. There was no history of smoking. The computer interpreted her rhythm as atrial fibrillation. Do you agree? Should the patient be anticoagulated?
Interpretation: In the absence of contraindications, the finding of atrial fibrillation is an indication for acute anticoagulation when a patient presents with an acute cerebrovascular accident (CVA) (e.g., non-hemorrhagic transient ischemic attack or stroke). However, the rhythm strip in the Figure does not represent atrial fibrillation; atrial activity is clearly present throughout the rhythm strip. P-wave morphology varies, virtually from beat to beat. A spectrum of disorders exists among the irregular supraventricular entities known as sinus rhythm or sinus arrhythmia with premature atrial contractions (PACs), wandering atrial pacemaker, and multifocal atrial tachycardia (MAT).
The key to distinguishing among these three entities lies with determining if there is an underlying sinus mechanism to the rhythm. This is defined by the presence of an upright P-wave shape with consistent morphology and a constant PR interval preceding many (if not most) of the QRS complexes on the tracing. Although in its extreme form, a marked sinus arrhythmia with frequent PACs may be difficult to recognize, one usually can identify the presence of an underlying sinus mechanism by recognizing at least a few consecutively occurring upright P waves with consistent P-wave morphology in at least selected portions of a sufficiently long lead II rhythm strip. This is very different than the phenomenon of a wandering atrial pacemaker, in which several beats occur with one P-wave shape, followed by a gradual shift for the ensuing consecutively conducted beats to a second or third P-wave shape—ultimately returning to the original P-wave morphology. This is consistent with the physiologic concept of a gradual shift in pacemaker site from different places in the atria.
In contrast to sinus mechanism rhythms and wandering pacemakers, P-wave morphology in the Figure is completely different from beat to beat, most consistent with the entity known as MAT. Admittedly the overall heart rate is not as rapid as the name of this entity implies. Although most often seen in long-term smokers with chronic pulmonary disease, MAT also may occur occasionally in non-smokers.
The clinically important point in this case is that despite constant alternation of atrial impulse sites, atrial contraction is maintained, such that anticoagulation of this rhythm is not essential as it would be if an elderly patient with acute non-hemorrhagic stroke presented with atrial fibrillation.
The electrocardiogram and rhythm strip in the figure were obtained from an elderly woman admitted for an acute stroke. Her neurologic deficit was not progressing, and she was clinically stable at the time of admission to the hospital. There was no history of smoking. The computer interpreted her rhythm as atrial fibrillation. Do you agree? Should the patient be anticoagulated?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
