A Hidden Rhythm
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The only clinical information available for this tracing is that the ECG was obtained from an older woman. Without any other background, where should we go from here?
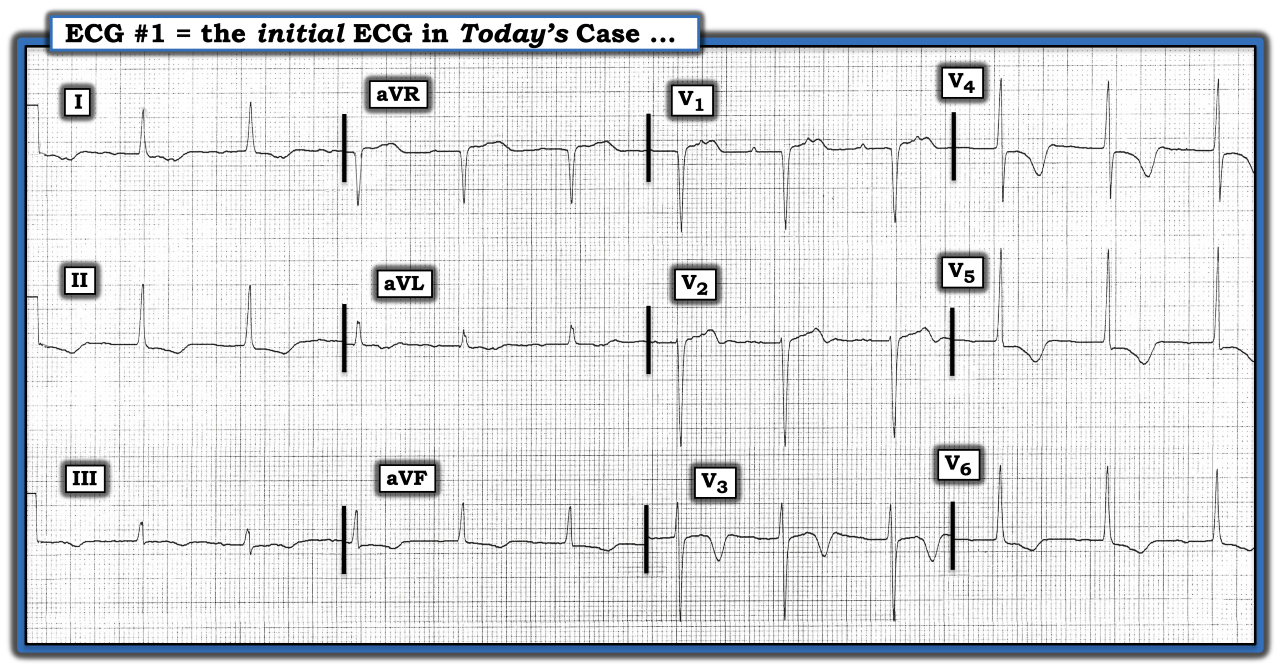
Interpretation: One of the most common oversights observed over the years is the failure to begin interpretation by always looking for atrial activity in lead II. If the rhythm is sinus, then an upright P wave with constant PR interval should be seen in standard lead II. Although we lack a long lead rhythm strip in this tracing, it should be apparent no P waves are present in lead II.
• After lead II, the next possible location for P waves is lead V1, since the chest electrode for this lead lies above the atria. The interesting finding here is P waves are visible in lead V1. They are not really apparent anywhere else on this ECG. Five P waves appear in lead V1, with a constant P-P interval. This suggests there is an underlying regular atrial rhythm at a rate of ~135 beats to 140 beats per minute.
• Although we would want to confirm the rhythm by reviewing a long lead V1 rhythm strip, it appears the PR interval before the second and third QRS complexes in lead V1 is constant. This strongly suggests the rhythm in this tracing is atrial tachycardia with 2:1 AV conduction. Otherwise, this ECG is remarkable for satisfying voltage criteria for left ventricular hypertrophy and for ST-T wave depression in multiple leads, with surprisingly deep T wave inversion in the midchest leads.
Impression: We do not know any clinical history about this patient but there are some abnormalities, including atrial tachycardia with 2:1 AV block and left ventricular hypertrophy. Also, there are ST-T wave abnormalities consistent with left ventricular “strain” and/or ischemia that may be acute (and which could be the result of a recent cardiac event). Full evaluation of this patient is essential.
For more information about and further discussion of this case, please click here.
The only clinical information available for this tracing is that the ECG was obtained from an older woman. Without any other background, where should we go from here?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
