Acute Shoulder Injuries in the Emergency Department
July 1, 2023
Reprints
AUTHORS
Kermit D. Huebner, MD, MPH, Assistant Professor, Emergency Medicine, Wright State University, Dayton, OH
Nick Gualtieri, DO, Resident, Wright State University, Dayton, OH
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Attending Emergency Physician, Trinity, Samaritan Hospital, Troy, NY
EXECUTIVE SUMMARY
- All elements of the shoulder joint complex are required for a stable and complete range of motion without joint subluxation.
- Provocative testing is useful for diagnosing rotator cuff, labral, and acromioclavicular injuries.
- Glenohumeral dislocations can be diagnosed with radiographs or point-of-care ultrasound.
- Assess distal nerve and vascular function before and after reduction of a glenohumeral dislocation.
- Sternoclavicular dislocations are associated with significant additional injuries.
- The majority of proximal humerus fractures are treated conservatively.
- Point-of-care ultrasound can identify rotator cuff tears and glenohumeral dislocation.
Epidemiology
Shoulder injuries have a significant impact on the quality of life. A recent systematic review of global shoulder pain found the annual incident rate varied from 7.7 to 62 per 1,000 person-years and lagged only behind the low back and the knee as a location for musculoskeletal pain.1
Persistent pain occurs in up to 50% of shoulder injuries.2 Loss of strength and range of motion have profound implications on recreational activities, occupational opportunities, and the ability to care for oneself, given that approximately 130 degrees of shoulder flexion and abduction are necessary to perform activities of daily living.3
Shoulder Anatomy, Function, and Evaluation
The shoulder girdle is designed to provide a wide range of motion and stability of the upper extremity through osseous and soft tissue structures. The osseous structures include the proximal humerus, the scapula (including the glenoid, coracoid process, and acromion), and the distal clavicle. The glenoid labrum and capsule, the rotator cuff, and the biceps tendon comprise the glenohumeral joint. Other supporting structures include the deltoid muscle, acromioclavicular (AC) joint, sternoclavicular (SC) joint, and scapulothoracic and subscapular bursae. The scapula is the foundation of the shoulder joint, providing articulation with the axial skeleton and the insertion of musculature, and includes the glenoid fossa for articulation with the humeral head. The rotator cuff and the deltoid muscle act synergistically to enable shoulder abduction and flexion through a wide range of motion.4
The shoulder’s main function is hand alignment along different anatomic planes while linking the axial and appendicular skeleton. The glenohumeral ligaments, synovial fluid, and glenoid labrum are static stabilizers, while muscular structures and the rotator cuff serve as dynamic stabilizers compressing the humeral head toward the glenoid.5 Compressive forces against the glenoid are required in the mid-range of shoulder motion because of the laxity of the capsuloligamentous structures.
Although the glenoid is shallow, the glenoid labrum increases depth by 50%.6 The unconstrained geometry of the glenohumeral joint is stabilized by the rotator cuff, with contributions from the deltoid, latissimus dorsi, teres major, biceps, and triceps throughout a full range of motion. The humeral head is centered anteroposteriorly by the antagonistic forces of the subscapularis and infraspinatus/teres minor muscles, while the supraspinatus counteracts the deltoid muscles’ cranial force.7 All elements of the shoulder joint are required for a balanced, stable, and complete range of motion without joint subluxation.
Evaluation of shoulder injuries requires a detailed history and directed physical examination. The clinician should obtain a history related to injury or overuse syndromes. The physical examination should include inspection, palpation, range of motion, strength, and neurovascular integrity.8 Inspection focuses on obvious deformities, muscle atrophy, prior incisions, scars, swelling, ecchymosis, and erythema visualized from the front, side, and back. Palpation is focused on the point of maximal pain described by the patient.
Range of motion testing consists of forward elevation, abduction, external rotation, and internal rotation. Normal range of shoulder motion consists of 180 degrees forward elevation, 90 degrees abduction with the scapula stabilized by the examiner’s hand, 80 degrees of external rotation at the side, and internal rotation to the fourth to eighth vertebral body.9
Sensation testing should include all dermatomes along the C4-T1 distribution and vascular testing should include the brachial, radial, and ulnar pulses.
Provocative testing may detect impingement, rotator cuff pathology, labral injuries such as superior labral anterior to posterior (SLAP) tears, AC joint pathology, and joint instability.
The Neer and Hawkins-Kennedy tests are used to identify shoulder impingement of the rotator cuff or bursa against the coracoacromial arch. The Neer test is positive when pain is elicited as the greater tuberosity impinges against the acromion during forced arm elevation while stabilizing the scapula. The Hawkins-Kennedy test is positive when pain is produced by flexing the shoulder to 90 degrees, flexing the elbow to 90 degrees, and forcibly internally rotating the shoulder to drive the greater tuberosity under the coracoacromial ligament. Both tests have sensitivity and specificity for subacromial impingement of about 70% to 80% and 60%, respectively.10
Rotator cuff testing isolates the subscapularis, supraspinatus, infraspinatus, and teres minor muscles. (See Table 1.) Labral injury testing includes the crank test, which is positive when clicking or pain is present in the shoulder with passive rotation and axial rotation of the arm while held in abduction. The O’Brien’s active compression test is positive for SLAP lesions when deep pain is elicited in the shoulder while the forearm is pronated but not when supinated. Superficial pain over the AC joint with O’Brien’s active compression testing portends an AC injury. Cross-body adduction also may elicit AC joint pain.
Table 1. Provocative Shoulder Examination Techniques |
||||
Pathology |
Test |
Performance Steps |
Positive Finding |
Sensitivity/Specificity |
Rotator cuff: subscapularis |
Internal lag sign |
Flex the patient’s elbow to 90° while holding the shoulder at 20° elevation and 20° extension while standing from behind. Internally rotate the shoulder to near maximum and ask the patient to maintain the position while supporting the elbow. |
A lag in internal rotation as the wrist is released |
100%/84% |
Lift off test |
Bring the hand around the back to the lumbar region with the palm facing outward and assess the patient’s ability to lift the hand away from the back with internal rotation. |
Inability to lift the hand away from the back |
80%/100% |
|
Belly press |
The patient presses the abdomen with the palm of the hand while maintaining shoulder internal rotation. |
The elbow does remain in the front of the body |
40%/90% |
|
Bear hug |
Place the patient’s palm on the opposite deltoid and ask them to resist the examiner pulling it anteriorly. |
Greater than 20% weakness compared to the other side |
60%/92% |
|
Rotator cuff: supraspinatus |
Jobe’s test |
Abduct the arm to 90° and angle forward by 30° and internally rotate with the thumb pointing to the floor. |
Pain and arm drop with the examiner pressing down while the patient attempts to maintain position |
88%/62% |
Drop sign |
Passively elevate the arm to 90° in the scapular plane while supporting the elbow, release the elbow support and have the patient slowly lower the arm back to neutral. |
Weakness or pain causes the arm to drop to the side |
73%/77% |
|
Rotator cuff: infraspinatus |
External rotation lag sign |
Passively flex the elbow to 90° and rotate the shoulder to maximal external rotation while holding the wrist and have the patient maintain that position. |
Arm drift into internal rotation |
56%/98% |
Rotator cuff: teres minor |
Hornblower’s sign |
Abduct the arm to 90° and externally rotate, then have the patient maintain position. |
Arm falls into internal rotation |
17%/96% |
Labral injuries and SLAP lesions |
Active compression test (O’Brien’s test) |
The patient forward flexes the arm to 90° while keeping the elbow extended. Adduct the arm 10° to 15° across the body and pronate the forearm with the thumb pointing down. The examiner then applies a downward force on the wrist in pronation and supination |
Positive for SLAP tear if deep pain in the glenohumeral joint with the forearm pronated but not when supinated |
67%/37% |
Crank test |
Hold the patient’s arm abducted and apply passive rotation and axial rotation. |
Clicking or pain in the glenohumeral joint |
46%/72% |
|
AC joint |
Cross-body adduction |
The patient elevates the arm to 90° and actively adducts the arm across the body. |
Pain in the AC joint |
77%/79% |
O’Brien’s test (active compression test) |
The patient forward flexes the arm to 90° with the elbow fully extended and the arm is then adducted 10° to 15° across the body with the forearm pronated. |
The patient resists when the examiner applies a downward force |
14%/92% |
|
SLAP: superior labral anterior posterior; AC: acromioclavicular |
||||
Specific Injuries
Shoulder injuries may involve soft tissues such as musculature, ligaments, and the labrum; dislocation of joint articulations; and fractures of osseous structures discreetly or in combination.
Rotator Cuff Tendinopathy
Rotator cuff tendinopathy is a multifactorial disorder. Age greater than 50 years, diabetes, cardiovascular disease, and osteoarthritis are associated with rotator cuff tendinopathy.11 Mechanical injury from repetitive movements associated with working with the shoulder above 90 degrees; extreme arm elevation; repetitive, high-frequency, high-force exposure; and vibration increase the risk for rotator cuff tendinopathy. Cell-mediated transformation of tenocytes into chondrocytes may lead to calcific deposits in the rotator cuff or the subacromial-subdeltoid bursa leading to rotator cuff calcific tendinitis.12 (See Figure 1.)
Figure 1. Calcific Tendinitis |
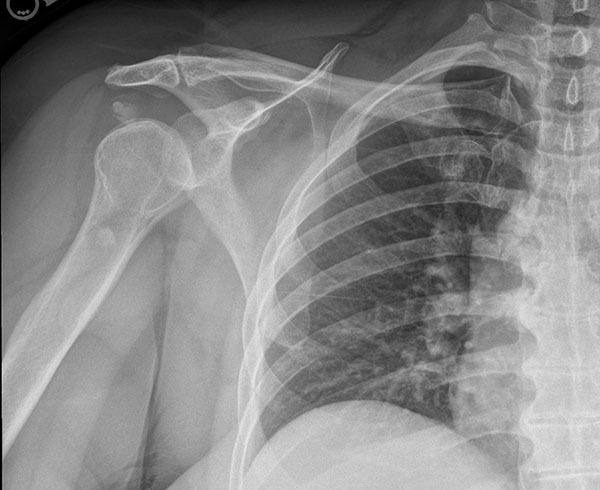 |
Courtesy of J. Stephan Stapczynski, MD. |
Symptoms may range from pain radiating from the anterior shoulder laterally to the arm, sudden pain with lifting and reaching, and pain with throwing an object, to loss of strength and motion. The hallmark of rotator cuff tendinopathy is pain and weakness experienced most during shoulder elevation and external rotation.13 A common feature of rotator cuff tendinopathy is the narrowing of the subacromial space, which may be evaluated by measuring the acromiohumeral distance by ultrasound, computed tomography (CT), or magnetic resonance imaging (MRI).14 Treatment includes relative rest, modification of activities, and physical therapy.
Rotator Cuff Tears
Rotator cuff tears result from injury and/or degeneration and are most common in the dominant arm.15 Most rotator cuff repairs occur in working-age patients, although the prevalence of tears increases with age. MRI studies of asymptomatic patients older than 60 years of age reveal up to 54% have partial or complete rotator cuff tears.16 Risk factors include repetitive lifting, overhead activities, and microtrauma associated with overuse syndromes in sporting and occupational activities.
Rotator cuff tears from acute injury typically are painful and may be associated with a snapping sensation with arm weakness. Acute, traumatic rotator cuff tears are present most commonly in younger patients with a fall on an outstretched hand, attempts to grab onto an object while falling, or associated with a shoulder dislocation. Plain film imaging should be obtained to exclude fractures or dislocation. Partial-thickness tears often are treated nonoperatively with a combination of nonsteroidal anti-inflammatories, physical therapy, and steroid injection, while full-thickness tears should be managed with surgical intervention.17
Nontraumatic tears from overuse may present with crepitus with certain shoulder movements, pain or weakness with specific movements, or pain at rest and at night. Plain film imaging may reveal a bone spur or degenerative changes but usually is normal.15 Conservative therapy includes analgesia, anti-inflammatory medications, physical therapy, and subacromial anesthetic injections with or without steroids. Nonoperative, conservative management should be continued for at least six weeks to three months with consideration for repeat imaging with ultrasound or MRI if there is no improvement. Surgery may be considered for full-thickness tears greater than 1 cm2, symptoms persisting more than one year, and functional impairment.18
The American Academy of Orthopaedic Surgeons’ clinical practice guidelines for the management of rotator cuff injuries include strong recommendations for using a combination of clinical examination testing to diagnose or stratify patients with rotator cuff tears, use of MRI and ultrasound as adjuncts to clinical examination, and consideration of both physical therapy and surgical management in symptomatic small to medium full-thickness rotator cuff tears.19
Labrum Injuries
The glenoid labrum is a vascularized fibrocartilaginous structure that contains sensory fibers to aid in proprioception.20 It acts as a bumper while deepening the concavity of the glenoid and serves as the attachment for glenohumeral ligaments creating a suction cup effect to maintain stability.21 Tears in the labrum result in shoulder pain and instability and may include a SLAP lesion (superior labrum from anterior to posterior), Bankart lesion (capsulolabral avulsion) anterior and inferiorly, and a posterior labral tear (reverse Bankart lesion).22
Symptoms range from vague deep shoulder pain, mechanical popping and clicking with range of motion, and weakness. Physical examination may reveal crepitance with range of motion and positive provocative testing dependent on the specific lesion.
Most patients will have anterior instability with increased susceptibility to dislocation, while those with posterior instability are prone to recurrent subluxations.23 The diagnosis of labial injuries can be confirmed with MRI, although the reported sensitivity is only about 50% but with a 90% specificity. First-line treatment for labrum injuries includes rest from sports, nonsteroidal anti-inflammatories, and physical therapy. SLAP lesions may require arthroscopic debridement with or without labrum repair and biceps tenotomy/tenodesis.24 Posterior labrum tears may require posterior labral repair with capsulorrhaphy.25
Adhesive Capsulitis
Adhesive capsulitis results from fibrosis and contracture of the joint capsule producing a painful shoulder with gradual loss of active and passive motion.26 This disorder may develop after repetitive microtrauma, and there is an increased incidence in patients with diabetes mellitus and hypothyroidism.27
Examination reveals a decreased range of motion, particularly with external rotation and abduction. Imaging is not required for the diagnosis; however, MRI may reveal thickening of the coracohumeral ligament, axillary pouch, and rotator interval joint capsule. MR arthrography (MRA) may reveal post-contrast enhancement of the joint capsule.28
Treatment includes nonsteroidal anti-inflammatories combined with physical therapy. Intraarticular corticosteroid injections may be effective in the short and mid-term. Patients with reduced post-injection external rotation in abduction and high pre- and post-injection pain scores are more likely to progress to surgical management.29 Combining hydrodilation by injecting fluid into the capsule under imaging and corticosteroid injections can expedite recovery, especially in the first three months of treatment.30
Arthroscopic capsular release (limited to the anterior capsule or circumferential) is effective in more than 80% of cases and allows for diagnostic arthroscopy to rule out additional pathology.31
Acromioclavicular Joint Injury and Dislocation
The AC joint provides articulation between the distal clavicle, the acromion process, and the coracoid process of the scapula, forming a gliding joint. The coracoclavicular ligaments (including the trapezoid and conoid) and AC ligaments enhance stability in the vertical and horizontal planes, respectively. The normal coracoclavicular distance from the superior coracoid to the inferior clavicle is 11 mm to 13 mm.
AC joint injuries typically occur from direct impact or a fall with the arm adducted. These injuries are common in athletic populations and account for up to 50% of shoulder injuries in contact sports.32 AC joint injuries may range from ligamentous sprains, partial and complete tears, to joint separation and dislocation.
AC joint injuries are described using the Rockwood classification based upon radiographic findings focused on the clavicle’s position in relation to the acromion.33 Type I injury consists of sprained AC ligaments resulting from a downward force on the acromion with normal radiographs. There is tenderness over the AC without AC instability. Type II injury includes rupture of the AC ligaments and sprained coracoclavicular ligaments with radiographic findings of AC joint widening with an elevation of the clavicle 25% to 50% above the acromion. Examination of the AC joint reveals tenderness and horizontal instability.
Type III injury results from disruption of the AC and coracoclavicular ligaments with the detachment of the deltoid and trapezius muscles. Vertical or horizontal instability will be present. Type III injuries will have 100% elevation of the clavicle above the acromion and a widened coracoclavicular interspace. (See Figure 2.) Type IV injury is the rupture of all supporting structures with posterior displacement of the clavicle in or through the trapezius. Radiographs in type IV injury may appear similar to a type II or III and often require axillary radiographs to visualize the posterior dislocation of the clavicle. Examination findings include posterior fullness and may include skin tenting.
Figure 2. Left AC Separation |
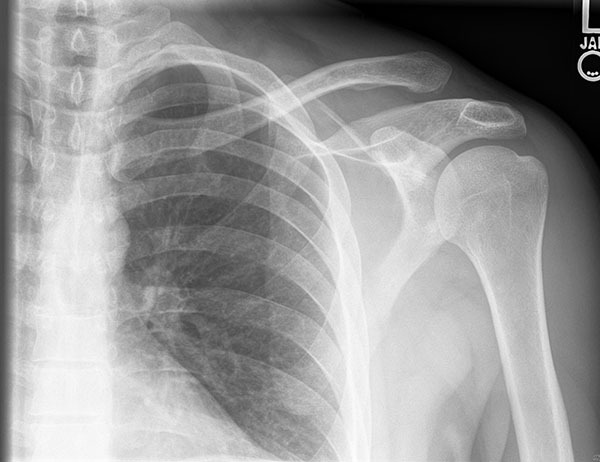 |
Courtesy of J. Stephan Stapczynski, MD. |
Type V injury is a rupture of all supporting structures similar to type III but with a 200% to 300% disparity of the coracoclavicular interspace. Clinically there is a severe shoulder droop that does not improve with attempts at shoulder shrug. Type VI injury includes an inferiorly displaced clavicle with disruption of the AC ligament, deltoid, and trapezius muscles. This rare injury often is associated with other injuries and may involve paresthesias from nerve injury.34
MRI allows assessment of the AC and coracoclavicular ligaments and interpretation may be enhanced when performed in the coronal oblique plane parallel to the distal clavicle.35 Further, radiographic and MRI classifications may be discordant in up to 50% of cases, with MRI findings more aligned with functional assessments using the AC joint instability score.36
Treatment of AC joint injuries typically is nonsurgical for type I and II injuries and surgical for type IV and VI, with debate on the indications for surgical management for type III and V injuries.37 Surgical management of AC joint injuries may range from soft tissue repair, tansarticular AC joint fixation, coracoclavicular screw fixation, nonanatomic reconstruction of the coracoclavicular ligaments, anatomic reconstruction of the coracoclavicular ligaments, distal clavicle resection, and dynamic muscle transfer.
Conservative treatment includes a sling and nonsteroidal anti-inflammatories. Both nonoperative and operative management of type III and V injuries provides good restoration of function and patient satisfaction at 24 months.38
Glenohumeral Shoulder Dislocations
The glenohumeral articulation is the most commonly dislocated joint in the body.39 Glenohumeral joint dislocations (shoulder dislocation) occur in a bimodal mechanism of injury pattern, with younger populations most often engaged in sporting activities and falls most common in patients older than 60 years of age. Dislocation results when a force applied to the shoulder disrupts the labrum, joint capsule, supporting ligaments, and muscles required for joint stability, given the substantial range of motion provided by the shallow glenoid.
Patients typically present with pain, deformity, and inability to perform a full range of motion at the shoulder. Physical examination should include a thorough assessment of the joint and the neurovascular integrity of the arm. Analgesia should be administered with consideration for nonsteroidal anti-inflammatories, opiates, or intraarticular injection of 10 mL to 20 mL of 1% lidocaine. Muscle relaxation for reduction may consist of benzodiazepines or procedural sedation, although many reduction techniques may be performed slowly without medication.
Shoulder dislocations are defined by the position of the humerus relative to the glenoid, with anterior, posterior, or inferior with anterior dislocations comprising more than 95%. A shoulder X-ray series including a trans-scapular Y view is sufficient for diagnosis in most cases.40 Imaging should be obtained before and after reduction to evaluate for fractures that may complicate the reduction and necessitate orthopedic consultation. Reduction of a humeral head dislocation associated with an isolated greater tuberosity fracture is associated with a low rate of displacement; however, emergency department reduction with surgical neck fractures resulted in a high rate of displacement.41
Anterior shoulder dislocations may be classified as subcoracoid, subglenoid, and subclavicular. The majority of anterior dislocations are subcoracoid, with subclavicular dislocations being rare. Patients present with a squared-off shoulder appearance with decreased ability to touch the opposite shoulder.
Reduction techniques are categorized as traction-countertraction, leverage, or scapular manipulation, with procedural steps noted in Table 2. A systematic review and meta-analysis of closed reduction techniques for closed shoulder reductions revealed decreased pain with scapular manipulation, followed by traction-countertraction techniques and then leverage techniques, with no difference in success rates between the groups.42 Incarceration of the long head of the biceps tendon and interposition of a rotator cuff tendon may create a mechanical block to closed reduction requiring surgical management.43
Table 2. Anterior Shoulder Reduction Techniques |
||
Category |
Technique |
Performance Steps |
Traction-Countertraction |
Hippocratic |
Place your heel in the patient’s axilla and apply traction by pulling on the forearm. |
“Traction-countertraction” |
Hold the patient’s elbow in 90° flexion and the shoulder in 90° abduction and apply traction to the shoulder by leaning back while the assistant provides counter traction. Sheets may be wrapped around the patient to assist with traction-countertraction. |
|
Stimson |
Place the patient prone with weights hanging from the wrists to gradually relieve muscle spasms, allowing the humeral head to reduce. May add downward manual traction or gentle external rotation as needed. |
|
FARES (Fast, Reliable, and Safe) |
Grasp the wrist of the affected arm and provide gentle axial traction. In a smooth and cyclical manner (about two cycles per second), move the arm up and down, about 5 cm above and below the horizontal plane. Continue arm oscillations while gradually abducting the arm. If not reduced at 90° of abduction, add gentle external rotation and continue abducting up to 120°. |
|
Boss-Halzack-Matter (DAVOS) |
Have the patient sit with hip and knee maximally flexed on the affected side. Tightly wrap the patient’s wrists together anterior to the tibial tuberosity using a bandage. Ask the patient to relax, gradually lean backward with the spine straight, extend the head, shrug the shoulders, and straighten the relaxed arms. |
|
Leverage |
“External rotation” (Hennepin) |
Gently hold the patient’s wrist and keep the elbow flexed 90° with the forearm neutral and the thumb pointed up. Slowly rotate externally by applying force to the volar surface of the wrist until the forearm is near 90° external rotation. |
Milch |
Place the patient in a supine position. Hold the patient’s arm at the wrist and abduct it to an overhead position and externally rotate it to 90°. |
|
Kocher |
Place the patient in a supine position with the arm adducted and the elbow flexed at 90°. Externally rotate the shoulder until resistance is felt. The shoulder then is adducted and flexed in external rotation. |
|
Cunningham |
The patient sits upright in a chair with the arm adducted next to the body and the elbow flexed to 90°. Kneel on the side of the affected arm facing the patient, then slide your hand between the patient’s forearm and body, with the hand of the patient resting on your upper arm. Apply gentle traction downward and massage the trapezius, deltoid, and biceps muscles in sequence to initiate reduction. |
|
Scapular Manipulation |
Scapular manipulation |
Place the patient in a prone position with the affected arm hanging over the bed and apply downward traction manually or by attaching weights. Manipulate the scapula stabilizing the superior aspect of the scapula. Use both of your thumbs to apply a medial and dorsal force to the inferior tip of the scapula to slightly displace it dorsally while pushing it toward the spine. |
Modified scapular manipulation |
Raise the head of the bed 90° and have the patient sit sideways, with the unaffected side leaning against the head of the bed. Apply downward traction and gently rotate the arm internally or externally as needed. Have an assistant manipulate the scapula as described earlier. |
|
Source: Streitz MJ. Overview of shoulder dislocation reduction techniques. MSD Manual. Professional Version. Reviewed/revised September 2022. https://www.msdmanuals.com/professional/injuries-poisoning/how-to-reduce-dislocations-and-subluxations/overview-of-shoulder-dislocation-reduction-techniques |
||
Posterior shoulder dislocations most often occur with movement of the humeral head posterior to the glenoid and inferior to the acromion. Posterior dislocations result from either an indirect force that leads to internal rotation and adduction of the shoulder, a direct blow anteriorly, or intense muscular contraction from seizures and electric shock.
Physical examination in poster dislocations typically shows anterior shoulder flattening with a posterior prominence and an inability to rotate or abduct externally. The arm may be locked in an internally rotated position. Plain film imaging may appear normal or reveal a “lightbulb” appearance of the humeral head; however, the trans-scapular Y view should demonstrate a humeral head posterior to the glenoid fossa. (See Figures 3 and 4.) A Velpeau view may be obtained if the patient cannot comply with a trans-scapular Y.44
Figure 3. Posterior Dislocation Anteroposterior View |
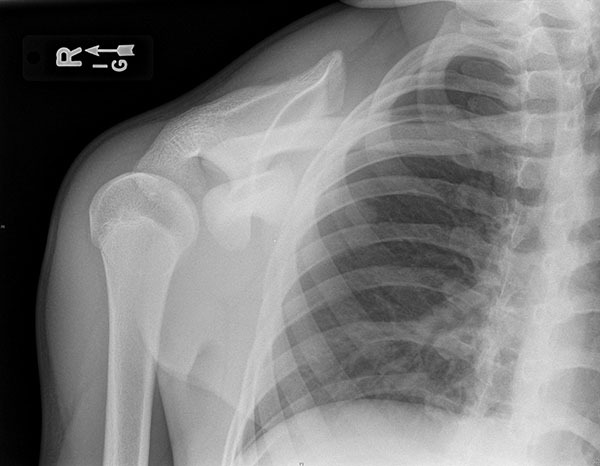 |
Courtesy of J. Stephan Stapczynski, MD. |
Figure 4. Posterior Dislocation Axillary View |
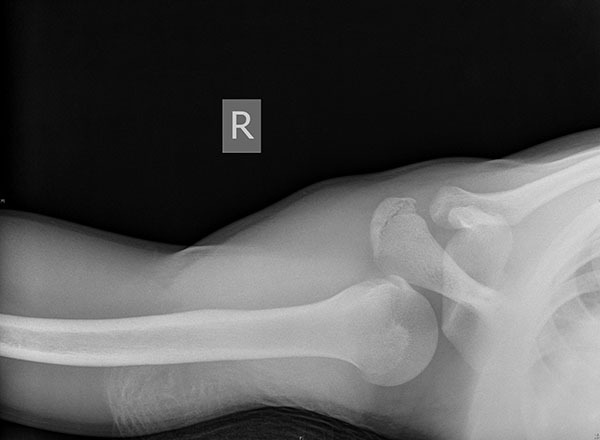 |
Courtesy of J. Stephan Stapczynski, MD. |
Closed reduction should be attempted by inline traction and manipulation of the humeral head followed by immobilization with up to 20 degrees of external rotation.45 The FARES (fast, reliable, safe) technique for anterior shoulder dislocations has been reported successful in a posterior dislocation case report.46 Surgical intervention with posterior labral repair may be required if non-reducible to closed reduction or if there is persistent posterior shoulder instability. Recurrent dislocation may occur in up to 9% of posterior shoulder dislocations associated with bony or soft tissue abnormalities.47
Inferior shoulder dislocations (luxation erecta) account for roughly 0.5% of all shoulder dislocations. A typical mechanism is a fall with extreme hyperabduction creating a tear in the inferior joint capsule allowing the humeral head to displace inferiorly. Patients are unable to adduct the arm, which is held in abduction with the elbow flexed toward the head. Physical examination should assess neurovascular compromise in addition to evaluation of the joint. Plain film imaging should reveal the humeral head inferior to the glenoid fossa.
Closed reduction techniques include traction-countertraction and may involve manual manipulation of the humeral head superiorly. Alternatively, the humerus may be pushed laterally while pulling superiorly on the medial condyle to move the humeral head into an anterior dislocation position, followed by any of the previously mentioned anterior reduction techniques.
Complications of shoulder dislocations include shoulder instability, fractures, and neurovascular injuries. Anterior dislocations may be complicated by a Hill-Sachs lesion, which is an osseous defect on the humeral head. (See Figure 5.) The incidence reaches 100% with recurrent anterior shoulder dislocations and may be associated with glenoid bone loss. Treatment includes nonsurgical management focused on physical therapy and rehabilitation.48
Figure 5. Hill Sachs Deformity |
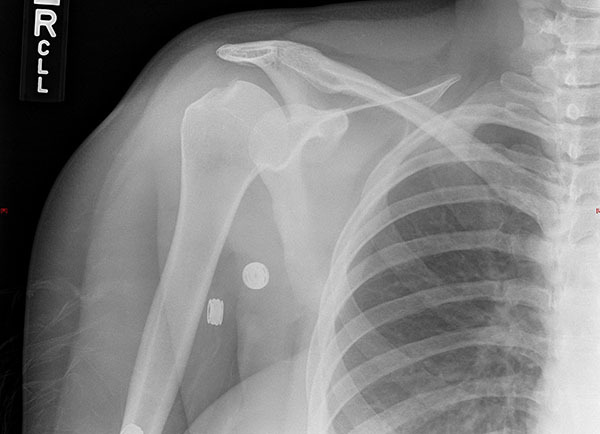 |
Courtesy of J. Stephan Stapczynski, MD. |
A Bankart lesion with or without bony involvement of the anteroinferior glenoid may be present and may result in instability. Posterior dislocations may result in labral or bony lesions posteriorly in a similar fashion.49
Brachial plexus injuries are a complication of shoulder dislocation, with increased incidence in elderly women with simple falls and young men with high-energy and multi-trauma injuries. Most brachial plexus injuries affect multiple nerves, with the axillary nerve being the most common. Symptoms mostly consist of neuropraxia, with complete nerve disruption occurring in less than 3%. The majority of symptoms resolve spontaneously. Operative treatment is required in up to 18%.50 Persistent motor weakness is associated with the duration of shoulder dislocation; therefore, prompt reduction should be expedited.51
Vascular injuries are rare, with axillary artery compression, lacerations, and pseudoaneurysms reported with anterior and inferior dislocations.52
Sternoclavicular Dislocation
SC joint injuries account for less than 3% of shoulder injuries but may prove difficult to diagnose and are associated with significant additional injuries.53 The SC joint comprises a fibrocartilaginous disc that articulates the proximal clavicle and the sternum. SC joint stability results from the costoclavicular, interclavicular, and capsular ligaments, with only roughly 50% of the medial clavicular surface articulating directly with the sternum. Disruption of the SC joint may result in anterior (more commonly) or posterior dislocation (less commonly) of the clavicle in relation to the sternum.54
SC disruption may occur after an indirect force with lateral compression, especially in the setting of multisystem trauma. SC dislocation often is missed in the multiple trauma patient; therefore, particular attention to the SC joint is important in the secondary and tertiary examination of patients with shoulder or clavicle pain.55
Anterior SC dislocation results from compressive forces to the thorax, including medially directed impact on the lateral shoulder.56 Patients present with pain and swelling adjacent to the sternum, with a limited range of motion of the ipsilateral shoulder. Anterior SC dislocations may be difficult to visualize on standard anterior-posterior radiographs; however, serendipity views with a 40% cephalic tilt may be helpful.
Orthopedic consultation may attempt reduction with procedural sedation or in the operating room under general anesthesia. Reduction is performed by abducting and extending the arm while applying axial traction and direct posterior pressure over the medial clavicle. Reduction is followed by application of a Velpeau bandage, plaster jacket, or figure-of-eight brace for six weeks.57
Posterior SC dislocation is rare, occurring in 3% to 5% of SC dislocations, and results from the application of force directly over the anteromedial aspect of the clavicle or indirect force to the posterolateral aspect of the shoulder.58 Posterior SC dislocation is much more dangerous because of the associated risk of pneumothorax, vascular injury to the subclavian vessels, esophagus, trachea, and brachial plexus. Failed recognition may result in long-term sequelae, including venous thromboembolism.59 Posterior dislocations may be clinically occult and difficult to identify radiographically. Plain film radiography poorly delineates the anatomy; therefore, CT is the imaging modality of choice and may reveal joint space widening and asymmetry along with associated mediastinal injuries.
Management includes orthopedic consultation with considerations for cardiothoracic and vascular surgery consultation for associated injuries.60 Immediate closed reduction is imperative if the involvement of mediastinal structures leads to hemodynamic instability, with procedural sedation or general anesthesia reserved for stable patients or those who fail closed reduction.61 Closed reduction consists of abducting and extending the arm while applying axial traction and using a towel clip to manipulate the medial clavicle.62 Post-reduction treatment includes a sling or figure-of-eight brace and consideration of operative management for those with recurrent instability, persistent pain, or limited range of motion.63
Shoulder Girdle Fractures
Proximal humerus fractures account for 50% of the humerus fractures diagnosed in U.S. emergency departments.64 Patients present with shoulder pain, swelling, and limited range of motion after a direct blow or fall on an outstretched hand. Physical examination should include an assessment of the axillary nerve (most commonly injured nerve), brachial plexus function, and distal circulation. Diagnosis is confirmed with plain film imaging to identify the fracture line, displacement, degree of angulation, or associated dislocation of the humeral head. CT may be required to delineate complex fracture patterns that may be difficult to appreciate on plain films and also can assess the articular surface.65
Proximal humerus fractures are classified based on the fracture pattern of four anatomic parts and associated displacement using the Neer classification system. The humeral shaft, articular surface, greater tuberosity, and lesser tuberosity comprise the four anatomic parts of the proximal humerus, and displacement is defined as 1 cm of fracture segment separation or greater than 45 degrees of angulation. This construct allows the grouping of fractures consisting of the number of fracture parts and degree of displacement.66
The majority of proximal humerus fractures are treated conservatively, especially if there is contact or impaction between the head and shaft, the humeral head is not dislocated, there is minimal varus or valgus angulation of the humeral head, there is minimal displacement of any tuberosity fracture, and there is minimal articular surface involvement.67 Conservative management includes sling immobilization followed by physical therapy and rehabilitation.
A Cochrane review of high-quality evidence found no difference in patient-reported function when comparing surgical and non-surgical intervention for most displaced fractures.68 Surgical management is required for open fractures, complex fracture patterns that may result in humeral head avascular necrosis, unacceptable functional impairment, or neurovascular compromise.69 Operative management may include open reduction internal fixation, hemiarthroplasty, or reverse shoulder arthroplasty.70 Open reduction internal fixation should occur within five days of the traumatic event to decrease complications, including humeral head avascular necrosis.71
Clavicle fractures comprise up to 4% of all emergency department fractures and result from direct impact or a fall onto the lateral aspect of the shoulder. The physical examination will reveal pain directly over the clavicle or the anterior shoulder associated with swelling, crepitus, or deformity over the clavicle. Skin tenting may be present and signifies an impending open fracture. Neurovascular assessment should include the subclavian vessels and brachial plexus.72
Diagnosis is confirmed by plain radiographs that reveal the location of the fracture, degree of angulation, displacement, communition, and amount of overlap in addition to AC and SC alignment, coracoclavicular distance, and glenohumeral joint abnormalities. Most clavicle fractures are mid-shaft, with distal clavicle fractures accounting for up to 30%.
Surgical management is indicated for open fractures, displaced fractures with skin tenting, associated vascular injury, or concomitant scapular neck fracture creating a floating shoulder. Midshaft fractures with greater than 2 cm of shortening are associated with decreased strength and endurance while those with greater than 100% displacement risk nonunion and may require surgical intervention.
Closed midshaft fractures that are neurovascularly intact with less than 2 cm of shortening and displacement may be treated conservatively with a sling or figure-of-eight strap followed by physical therapy and rehabilitation.73
Distal clavicle fractures are prone to deforming forces from the musculature and ligamentous attachments and are classified based on fracture displacement and disruption of the coracoclavicular ligaments.74 Nondisplaced fractures with intact coracoclavicular ligaments are treated nonoperatively, displaced fractures with intact coracoclavicular ligaments may be treated conservatively or surgically, and displaced fractures with torn coracoclavicular ligaments require operative management.
Scapular fractures comprise 3% to 5% of traumatic shoulder girdle injuries and typically result from high-energy traumatic mechanisms, such as motor vehicle collisions or falls from heights.75 Patients present with the arm held in adduction with shoulder pain and tenderness over the scapula. These fractures may be difficult to appreciate on plain films of the chest and shoulder, with dedicated scapula CT imaging often required to determine the fracture morphology and associated glenoid involvement. Fracture morphology includes the involvement of the scapula process (coracoid, acromion, spine), scapula body, or glenoid fossa.76
Most scapula fractures may be managed conservatively with sling and early range of motion, with surgical intervention considered for medial displacement of the lateral border greater than 25 mm, angular deformity of greater than 45 degrees, intra-articular step of 3 mm to 5 mm, and displaced double disruption of the superior shoulder suspensory complex. Isolated fractures of the coracoid process or acromion also may benefit from surgical fixation.77
Point-of-Care Ultrasound
Point-of-care ultrasound (POCUS) provides a noninvasive method to visualize the anatomy and function of the musculoskeletal system while assisting with diagnosis and therapy. POCUS has reliable sensitivity and specificity among specialists and radiologists for assessing partial and full rotator cuff tears and improved accuracy of shoulder space injections compared to landmark-guided injections.78 Further, hand-held, pocket-sized ultrasounds offer a portable and affordable means to evaluate shoulder pathology in prehospital and resource-constrained environments.79
POCUS may diagnose complete supraspinatus rotator cuff tears by non-visualization of the tendon, focal tendon defects for full-thickness tears, and hypoechoic defects or flattening of the bursal surface for partial-thickness tears. POCUS also may reveal cortical irregularity of the greater tuberosity or effusion as secondary signs of rotator cuff pathology.80 Studies comparing ultrasound to MRI demonstrate no statistically significant difference in diagnostic sensitivity, specificity, or accuracy for supraspinatus tears.81
Optimal examination technique involves viewing the specific tendon in static longitudinal and transverse planes with a high-frequency 7 MHz to 12 MHz probe complemented by dynamic examination demonstrating tendon slide. The long head of the bicep, subscapularis, supraspinatus, infraspinatus, and glenoid labrum also may be evaluated.82
POCUS also is sensitive and specific for rapid identification of shoulder dislocations, reduction confirmation, and detection of associated fractures. Examination protocols include anterior assessment of the coraco-humeral distance, lateral assessment of the acromio-humeral distance, posterior view of the glenohumeral joint, or measurement of the glenohumeral separation distance.83
A simple posterior approach to visualize the relationship of the humeral head to the glenoid fossa can be performed in three steps. First, position the machine in front of the patient while placing a curvilinear probe over the scapular spine in a transverse plane with the probe marker toward the patient’s left. Second, identify the scapular spine as a hyperechoic line with a posterior shadow. Lastly, slide the probe laterally toward the glenohumeral joint and visualize the glenoid fossa and humeral head. Anterior dislocations will show the humeral head displaced to the far field while a posterior dislocation will show the humeral head displaced to the near field.84
Conclusion
Shoulder injuries account for a significant portion of musculoskeletal injuries evaluated in the emergency department.The incidence is projected to increase dramatically over the next decade because of changing population characteristics. Emergency medicine clinicians must be prepared to care for shoulder injuries from direct trauma and overuse from sporting activities or occupational injuries.
REFERENCES
- Lucas J, van Doorn P, Hegedus E, et al. A systematic review of the global prevalence and incidence of shoulder pain. BMC Musculoskelet Disord 2022;23:1073.
- Luime JJ, Koes BW, Hendriksen IJM, et al. Prevalence and incidence of shoulder pain in the general population; a systematic review. Scand J Rheumatol 2004;33:73-81.
- Oosterwijk AM, Nieuwenhuis MK, van der Schans CP, Mouton LJ. Shoulder and elbow range of motion for the performance of activities of daily living: A systematic review. Physiother Theory Pract 2018;34:505-528.
- Hecker A, Aguirre J, Eichenberger U, et al. Deltoid muscle contribution to shoulder flexion and abduction strength: An experimental approach. J Shoulder Elbow Surg 2021;30:e60-e68.
- Faria L, Campos B, Jorge RN. Biomechanics of the shoulder girdle: A case study on the effects of union rugby tackles. Acta Bioeng Biomech 2017;19:115-127.
- Yamamoto N, Itoi E. A review of biomechanics of the shoulder and biomechanical concepts of rotator cuff repair. Asia Pac J Sports Med Arthrosc Rehabil Technol 2015;2:27-30.
- Bouaicha S, Slankamenac K, Moor BK, et al. Cross-sectional area of the rotator cuff muscles in MRI — Is there evidence for a biomechanical balanced shoulder? PLoS One 2016;11:1-13.
- Bakhsh W, Nicandri G. Anatomy and physical examination of the shoulder. Sports Med Arthrosc Rev 2018;26:e10-e22.
- Sharereh B, Keener J, Levine W. Shoulder exam. Ortho Bullets. Updated Aug. 6, 2021. https://www.orthobullets.com/shoulder-and-elbow/3037/shoulder-exam
- Hegedus EJ, Goode AP, Cook CE, et al. Which physical examination tests provide clinicians with the most value when examining the shoulder? Update of a systematic review with meta-analysis of individual tests. Br J Sports Med 2012;46:964-978.
- Leong HT, Fu SC, He X, et al. Risk factors for rotator cuff tendinopathy: A systematic review and meta-analysis. J Rehabil Med 2019;51:627-637.
- Chianca V, Albano D, Messina C, et al. Rotator cuff calcific tendinopathy: From diagnosis to treatment. Acta Biomed 2018;89:186-196.
- Lewis J, McCreesh K, Roy JS, Ginn K. Rotator cuff tendinopathy: Navigating the diagnosis-management conundrum. J Orthop Sports Phys Ther 2015;45:923-937.
- McCreesh KM, Crotty JM, Lewis JS. Acromiohumeral distance measurement in rotator cuff tendinopathy: Is there a reliable, clinically applicable method? A systematic review. Br J Sports Med 2015;49:298-305.
- Athwal GS, Armstrong AD. Rotator cuff tears. OrthoInfo RC: American Academy of Orthopaedic Surgeons [Internet]. Last reviewed June 2022. https://orthoinfo.aaos.org/en/diseases--conditions/rotator-cuff-tears/
- Sher JS, Uribe JW, Posada A, et al. Abnormal findings on magnetic resonance images of asymptomatic shoulders. J Bone Joint Surg Am 1995;77:10-15.
- Patel M, Amini MH. Management of acute rotator cuff tears. Orthop Clin North Am 2022;53:69-76.
- Clement ND, Nie YX, McBirnie JM. Management of degenerative rotator cuff tears: A review and treatment strategy. Sports Med Rehabil Ther Technol 2012;4:48.
- Weber S, Chahal J. Management of rotator cuff injuries. J Am Acad Orthop Surg 2020;28:e193-e201.
- Alashkham A, Alraddadi A, Felts P, Soames R. Histology, vascularity and innervation of the glenoid labrum. J Orthop Surg (Hong Kong) 2018;26:2309499018770900.
- Ishikawa H, Henninger HB, Kawakami J, et al. A stabilizing role of the glenoid labrum: The suction cup effect. J Shoulder Elbow Surg 2023;32:1095-1104.
- Clavert P. Glenoid labrum pathology. Orthop Traumatol Surg Res 2015;101(1 Suppl):S19-24.
- Christensen DL, Elsenbeck MJ, Wolfe JA, et al. Risk factors for failure of nonoperative treatment of posterior shoulder labral tears on magnetic resonance imaging. Mil Med 2020;185:e1556-e1561.
- Steffes MJ, McCulloch PC. SLAP lesion. Ortho Bullets. Updated Jan. 8, 2023. https://www.orthobullets.com/shoulder-and-elbow/3053/slap-lesion
- Bassett A, Farmer K. Posterior labral tear. Ortho Bullets. Updated June 5, 2023. https://www.orthobullets.com/shoulder-and-elbow/3057/posterior-labral-tear
- Neviaser AS, Neviaser RJ. Adhesive capsulitis of the shoulder. J Am Acad Orthop Surg 2011;19:536-542.
- Ramirez J. Adhesive capsulitis: Diagnosis and management. Am Fam Physician 2019;99:297-300.
- Fields BKK, Skalski MR, Patel DB, et al. Adhesive capsulitis: Review of imaging findings, pathophysiology, clinical presentation, and treatment options. Skeletal Radiol 2019;48:1171-1184.
- Hanish SJ, Resnick ML, Kim HM, Smith MJ. Predictive factors for failure of injection in management of adhesive capsulitis of the shoulder. J Clin Med 2022;11:6212.
- Catapano M, Mittal N, Adamich J, et al. Hydrodilatation with corticosteroid for the treatment of adhesive capsulitis: A systematic review. PM R 2018;10:623-635.
- Leafblad N, Mizels J, Tashjian R, Chalmers P. Adhesive capsulitis. Phys Med Rehabil Clin N Am 2023;34:453-468.
- Willimon SC, Gaskill TR, Millett PJ. Acromioclavicular joint injuries: Anatomy, diagnosis, and treatment. Phys Sportsmed 2011;39:116-122.
- Gaillard F, Botz B, Knipe H, et al. Rockwood classification of acromioclavicular joint injury. Radiopaedia.org. Last revised March 16, 2021. https://doi.org/10.53347/rID-845
- Gorbaty JD, Hsu JE, Gee AO. Classifications in brief: Rockwood classification of acromioclavicular joint separations. Clin Orthop Relat Res 2017;475:283-287.
- Alyas F, Curtis M, Speed C, et al. MR imaging appearances of acromioclavicular joint dislocation. Radiographics 2008;28:463-479; quiz 619.
- Minkus M, Wieners G, Maziak N, et al. The ligamentous injury pattern in acute acromioclavicular dislocations and its impact on clinical and radiographic parameters. J Shoulder Elbow Surg 2021;30:795-805.
- Frank RM, Cotter EJ, Leroux TS, Romeo AA. Acromioclavicular joint injuries: Evidence-based treatment. J Am Acad Orthop Surg 2019;27:e775-e788.
- Boström Windhamre H, von Heideken J, Une-Larsson V, et al. No difference in clinical outcome at 2-year follow-up in patients with type III and V acromioclavicular joint dislocation treated with hook plate or physiotherapy: A randomized controlled trial. J Shoulder Elbow Surg 2022;31:1122-1136.
- Cutts S, Prempeh M, Drew S. Anterior shoulder dislocation. Ann R Coll Surg Engl 2009;91:2-7.
- Jones J, Ranchod A, Qreshi P, et al. Shoulder dislocation. Radiopaedia.org. Last revised Apr. 3, 2023. https://radiopaedia.org/articles/shoulder-dislocation
- Green A, Choi P, Lubitz M, et al. Proximal humeral fracture-dislocations: Which patterns can be reduced in the emergency department? J Shoulder Elbow Surg 2022;31:792-798.
- Dong H, Jenner EA, Theivendran K. Closed reduction techniques for acute anterior shoulder dislocation: A systematic review and meta-analysis. Eur J Trauma Emerg Surg 2021;47:407-421.
- Liechti DJ, Shepet KH, Glener JE, et al. A systematic review of acute irreducible shoulder dislocations in the 21st century. Orthop J Sports Med 2022;10:23259671221121633.
- Provencher M, Lin A. Posterior shoulder instability & dislocation. Ortho Bullets. Updated Nov. 29, 2021. https://www.orthobullets.com/shoulder-and-elbow/3051/posterior-shoulder-instability-and-dislocation
- Kammel KR, El Bitar Y, Leber EH. Posterior shoulder dislocations. In: StatPearls [Internet]. StatPearls Publishing; 2023 Jan-. Updated Sept. 12, 2022. https://www.ncbi.nlm.nih.gov/books/NBK441919/
- Yu TC, Ju WN, Wang CX, et al. Reduction of acute posterior shoulder dislocation with the FARES method: A case report and a review of the literature. Technol Health Care 2016;24:81-85.
- Longo UG, Ciuffreda M, Locher J, et al. Posterior shoulder instability: A systematic review. Br Med Bull 2020;134:34-53.
- Provencher MT, Frank RM, Leclere LE, et al. The Hill-Sachs lesion: Diagnosis, classification, and management. J Am Acad Orthop Surg 2012;20:242-252.
- Ladd LM, Crews M, Maertz NA. Glenohumeral joint instability: A review of anatomy, clinical presentation, and imaging. Clin Sports Med 2021;40:585-599.
- Gutkowska O, Martynkiewicz J, Urban M, Gosk J. Brachial plexus injury after shoulder dislocation: A literature review. Neurosurg Rev 2020;43:407-423.
- Wu F, Dhir R, Ng CY. Patterns of nerve injury and recovery rates of infraclavicular brachial plexus lesions following anterior shoulder dislocation. J Hand Surg Am 2022;47:1227.e1-1227.e7.
- Karnes JM, Bravin DA, Hubbard DF. Axillary artery compression as a complication of a shoulder dislocation. J Shoulder Elbow Surg 2016;25:e61-364.
- Daniel H, Thomas P, Peter C. Current concepts in sternoclavicular joint injuries. J Orthop Trauma 2023; Apr 27. doi: 10.1097/BOT.0000000000002625. [Online ahead of print].
- Morell DJ, Thyagarajan DS. Sternoclavicular joint dislocation and its management: A review of the literature. World J Orthop 2016;7:244-250.
- Chaudhry S. Pediatric posterior sternoclavicular joint injuries. J Am Acad Orthop Surg 2015;23:468-475.
- Varada SL, Popkin CA, Hecht EM, et al. Athletic injuries of the thoracic cage. Radiographics 2021;41:E20-E39.
- Weatherford B. Sternoclavicular dislocation. Ortho Bullets. Updated May 24, 2021. https://www.orthobullets.com/trauma/1009/sternoclavicular-dislocation?hideLeftMenu=true
- Fandridis E, Koutserimpas C, Raptis K, et al. Anterior dislocation of sternoclavicular joint: A novel surgical technique. Injury 2022;53:1562-1567.
- Chen X, Shafer D, Neeki AS, et al. Emergent management of traumatic posterior sternoclavicular joint dislocation: A case report and literature review. Cureus 2021;13:e18996.
- Carius BM, Long B, Gottlieb M. Evaluation and management of sternoclavicular dislocation in the emergency department. J Emerg Med 2021;61:499-506.
- Glass ER, Thompson JD, Cole PA, et al. Treatment of sternoclavicular joint dislocations: A systematic review of 251 dislocations in 24 case series. J Trauma 2011;70:1294-1298.
- Groh GI, Wirth MA. Management of traumatic sternoclavicular joint injuries. J Am Acad Orthop Surg 2011;19:1-7.
- Groh GI, Wirth MA, Rockwood CA Jr. Treatment of traumatic posterior sternoclavicular dislocations. J Shoulder Elbow Surg 2011;20:107-113.
- Kim SH, Szabo RM, Marder RA. Epidemiology of humerus fractures in the United States: Nationwide emergency department sample, 2008. Arthritis Care Res (Hoboken) 2012;64:407-414.
- Neer CS 2nd. Four-segment classification of proximal humeral fractures: Purpose and reliable use. J Shoulder Elb Surg 2002;11:389-400.
- Neer CS 2nd. Displaced proximal humeral fractures. J Bone Joint Surg 1970;52:1077-1089.
- Robinson CM, Amin AK, Godley KC, et al. Modern perspectives of open reduction and plate fixation of proximal humerus fractures. J Orthop Trauma 2011;25:618-629.
- Handoll HH, Brorson S. Interventions for treating proximal humeral fractures in adults. Cochrane Database Syst Rev 2015;11:CD000434.
- Rudran B, Little C, Duff A, et al. Proximal humerus fractures: Anatomy, diagnosis and management. Br J Hosp Med (Lond) 2022;83:1-10.
- Yahuaca BI, Simon P, Christmas KN, et al. Acute surgical management of proximal humerus fractures: ORIF vs. hemiarthroplasty vs. reverse shoulder arthroplasty. J Shoulder Elbow Surg 2020;29:S32-S40.
- Siebenbürger G, Van Delden D, Helfen T, et al. Timing of surgery for open reduction and internal fixation of displaced proximal humeral fractures. Injury 2015;46(Suppl 4):S58-S62.
- Tarazona D, Ahn L, Sheth U. Clavicle fractures – midshaft. Ortho Bullets. Updated July 28, 2022. https://www.orthobullets.com/trauma/1011/clavicle-fractures--midshaft
- Serpico M, Tomberg S. The emergency medicine management of clavicle fractures. Am J Emerg Med 2021;49:315-325.
- Sandstrom CK, Gross JA, Kennedy SA. Distal clavicle fracture radiography and treatment: A pictorial essay. Emerg Radiol 2018;25:311-319.
- Tatro JM, Schroder LK, Molitor BA, et al. Injury mechanism, epidemiology, and hospital trends of scapula fractures: A 10-year retrospective study of the National Trauma Data Bank. Injury 2019;50:376-381.
- Huflage H, Fieber T, Färber C, et al. Interobserver reliability of scapula fracture classifications in intra- and extra-articular injury patterns. BMC Musculoskeletal Disord 2022;23:1-7.
- Limb D. Scapula fractures: A review. EFORT Open Rev 2021;6:518-525.
- Tat J, Tat J, Theodoropoulos J. Clinical applications of ultrasonography in the shoulder for the orthopedic surgeon: A systematic review. Orthop Traumatol Surg Res 2020;106:1141-1151.
- Lau BC, Motamedi D, Luke A. Use of pocket-sized ultrasound device in the diagnosis of shoulder pathology. Clin J Sport Med 2020;30:20-24.
- Papatheodorou A, Ellinas P, Takis F, et al. US of the shoulder: Rotator cuff and non-rotator cuff disorders. Radiographics 2006;26:e23.
- Farooqi AS, Lee A, Novikov D, et al. Diagnostic accuracy of ultrasonography for rotator cuff tears: A systematic review and meta-analysis. Orthop J Sports Med 2021;9:1-12.
- Selame LAJ, Matsas B, Krauss B, et al. A stepwise guide to performing shoulder ultrasound: The acromio-clavicular joint, biceps, subscapularis, impingement, supraspinatus protocol. Cureus 2021;13:e18354.
- Gottlieb M, Russell F. Diagnostic accuracy of ultrasound for identifying shoulder dislocations and reductions: A systematic review of the literature. West J Emerg Med 2017;18:937-942.
- Marrero-Zeda R, Rivera-Morales M, Rivera F, Rosario J. POCUS for shoulder pain in the emergency department. ACEP EUS Section Simulation Subcommittee. April 2, 2021. American College of Emergency Physicians. https://www.acep.org/emultrasound/newsroom/apr2021/pocus-for-shoulder-pain-in-the-emergency-department/
Shoulder injuries account for a significant portion of musculoskeletal injuries evaluated in the emergency department.The incidence is projected to increase dramatically over the next decade because of changing population characteristics. Emergency medicine clinicians must be prepared to care for shoulder injuries from direct trauma and overuse from sporting activities or occupational injuries.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
