Hanging and Strangulation Injuries in Intimate Partner Violence
December 15, 2023
Reprints
AUTHORS
Sreeja M. Natesan, MD, FACEP, Associate Professor, Duke Department of Emergency, Medicine Durham, NC
Megan J. Rivera, MD, Medical Instructor, Duke Department of Emergency Medicine, Durham, NC
Nina Angeles, MD, Resident Physician PGY2, Duke Department of Emergency Medicine, Durham, NC
Christopher J. Nash, MD, EdM, Medical Instructor, Duke Department of Emergency Medicine, Durham, NC
PEER REVIEWERS
Steven M. Winograd, MD, FACEP, Attending Emergency Physician, Trinity, Samaritan Hospital, Troy, NY
EXECUTIVE SUMMARY
- Strangulation is a serious escalation in intimate partner violence (IPV); the risk of homicide from IPV increases sevenfold after a nonfatal strangulation (NFS) episode.
- Surprisingly little force is required to compress the vital structures in the neck: venous blood flow (4-5 pounds), carotid blood flow (7-8 pounds), and the airway (22 pounds).
- Forty percent to 85% of NFS survivors lack visible injury, and only 15% have an injury of sufficient quality to be used as photographic evidence.
- Patients with little or no external signs of strangulation still are at risk for life-threatening internal injury.
- The recommended imaging modality is a computed tomography angiogram of the carotid and vertebral arteries, with abnormalities seen in approximately 2% to 7% of those studied.
- Social service or behavioral health evaluation should be considered in NFS victims.
- An NFS patient who is asymptomatic after four to six hours of observation may be a candidate for discharge to a safe environment, provided they are not considered a harm to themselves.
Definition of the Problem
Strangulation is considered one of the most lethal forms of intimate partner violence (IPV); however, it remains under-identified by responding police officers and healthcare providers.1,2 According to the American Academy of Forensic Sciences, strangulation encompasses hanging, manual strangulation, and ligature strangulation and is defined as the application of direct pressure against a person’s neck, occluding or injuring blood vessels and/or the airway.1,3,4 Hanging is a subtype of strangulation where the victim is suspended or near suspended in the air by a device around the neck. The incorporation of postural mechanisms, typically their body weight, causes compression of the neck structures.4 The severity of the injury is dependent on the amount and duration of pressure, as well as the modality.5
There are several categories of strangulation and hanging, described in Table 1.4,6,7
Table 1. Types of Strangulation and Hanging |
|
Types |
Mechanism |
Manual strangulation |
Injury is caused by direct pressure of the victim’s neck by a body part (i.e., hand[s], forearm, knee, or any combination). |
Ligature strangulation |
Injury is caused by using a rope-like object around the victim’s neck (i.e., rope, electrical cord, piece of clothing, patient’s long hair). |
Complete hanging |
Injury is a result of a fall from height and complete suspension of the body by a ligature device (i.e., previously seen in use for capital punishment [known as judicial hanging]). |
Near/incomplete hanging |
In contrast to complete hangings, incomplete or partial hangings do not have the associated drop, although they can involve partial or complete suspension of the body by a ligature device (i.e., suicide attempt by hanging). |
Relevance of the Problem to the Adult Population
Strangulation and hanging can result in serious morbidity and mortality due to the asphyxia and ischemia from airway closure or vascular injury.8 As emergency medicine providers, early identification through appropriate diagnosis, treatment, and access to resources is vital to helping this vulnerable population.9 Blunt cerebrovascular injury and subsequent stroke may occur in up to 20% of patients within 72 hours post-injury, further highlighting the importance of early and accurate diagnosis.10
The role of identifying injury has been persistently difficult for healthcare workers. Survivors of IPV present with a wide range of signs and symptoms, from undetectable to fatal injuries.5,11 Anchoring on external signs can be misleading as, when present, visible injuries usually are minor or overlooked by untrained providers.4,11 The majority of nonfatal strangulation (NFS) cases may not have external signs that demonstrate the trauma that occurred. While studies vary, it is reported that as many as 40% to 85% of cases of strangulation survivors lack any visible injuries, and only 15% of that population had an injury of sufficient quality to be used as photographic evidence.5,11,12
Strangulation also often is minimized by the survivor and underdiagnosed by the healthcare provider.9 Survivors may be reluctant to disclose IPV because of shame, fear of retaliation, or fear of further marginalization.1,13 This can result in the misperception that this vulnerable population may not want help.13 To further compound the issue, there are limited screening and assessment tools and few guidelines available for healthcare providers to use to identify IPV.1,13 Additionally, memory may be affected due to a hypoxic insult or the psychological trauma, further complicating accurate diagnosis and management.1 The underdiagnosis of strangulation and IPV despite their high prevalence combined with the challenges of managing hanging and strangulation cases make this topic of universal importance to the practicing emergency clinician.
Epidemiology
Since 2020, the World Health Organization reports approximately 6 million people have died due to IPV, meaning the number of deaths by homicide have exceeded the number of war-related deaths over the same period.14 Studies vary on the incidence of IPV by sex. According to the Centers for Disease Control and Prevention (CDC), in the United States, IPV affects 1 in 3 women and 1 in 4 men each year, yet some studies share an extreme sex disparity with rates 13 times higher in females than in males.4,15 IPV costs exceed $9.3 billion annually, including direct costs for medical care and indirect costs such as loss of productivity, ability to work, and earnings.11
Strangulation has been implicated as a way for the perpetrator to show dominance over the victim, with up to 68% of IPV survivors reporting having experienced NFS by an abuser.4,11 The COVID-19 pandemic, unfortunately, further exacerbated harm. Among women who had previous physical or sexual violence reported, more than half reported an increase in frequency and severity since February 2020.16 IPV and femicide also is known to disproportionately affect women of color, especially Black women, compared to their white counterparts.2
NFS has been called, horrifically, “the edge of homicide,” and for those patients who have experienced an NFS, their risk of attempted murder by the same abusive partner increases sevenfold, and risk of death increases by a factor of eight.4,9,17 Most survivors are strangled multiple times in their lives, and in one study nearly half reported being strangled between three and 20 times.13 Additionally, there are existing issues that are exacerbated for survivors of color, including the fact that injuries may be less visible due to the increased melanin in their skin.2
Hanging accounts for the second leading mechanism of self-harm in the United States and the most common method in parts of Europe and Asia.3,6,7,18,19 Since 1992, there has been an increase in the use of hanging as the modality for suicide among young people (age range 10-24 years).6 In fact, from the period of 2000 to 2015, the use of hanging as the method for suicide increased and is the second leading mechanism of self-harm. 18 For hanging, fatality rates range from 69% to 84%.6 Survival rates following any form of hanging have been estimated at around 30%; however, they are markedly lower when it results in out-of-hospital cardiac arrest.19
Etiology
The predominant risk factor for strangulation is IPV. Female victims of intimate partner homicide had the following risk factors: active pregnancy, having children not with the perpetrator, having less than a high school education, and/or substance use disorder.14 Depression and suicidal ideation risk factors have been implicated in hanging attempts.
Pathophysiology
Both strangulation and hanging result in injury due to compression of the structures of the neck. Strangulation typically involves the perpetrator using their hands, forearms, body mass, or ligatures to impede the victim’s ability to breathe, leading to a disruption of oxygenated blood flow to the brain.2 The mechanism from hanging varies based on the height component.
Judicial hanging uses a drop from a distance precisely calculated from the person’s height and weight that would result in severe hyperextension and subsequent bilateral pedicle fracture of the second cervical vertebra and spinal cord injury, known as the hangman’s fracture.7 However, in suicide attempts, this fall from height is uncommon, and death typically is a consequence of occlusion of the vascular structures, compression of the trachea, or pressure on the baroreceptors of the carotid sinuses, resulting in vagally mediated cardiovascular suppression.7
Strangulation results in asphyxia due to the application of pressure to the neck, whether it is mechanical strangulation, ligature strangulation, or chokehold strangulation by an arm around the head.11 Due to the lack of skeletal protection, the relative exposure/accessibility of the airway, surrounding vessels, and spinal cord, the neck is particularly vulnerable to life-threatening injuries.11 Minimal force can affect the patient, and injury and/or death can occur within minutes.5 Very little pressure is required to compress the venous blood flow (2 kg; 4 lbs., 6 oz.), carotid blood flow (3.5 kg; 7 lbs., 11 oz.), and airway structures (10 kg; 22 lbs.), resulting in injury and even death with surprisingly little force.4,7
A wide array of injuries (as seen in Table 2) may present immediately or up to weeks after an occurrence.1,2,4,7 External injuries, when present, can range from superficial abrasions and lacerations to muscle injury and broken bones.6 More important are the internal structures that, when occluded, can lead to subsequent anoxia to the brain.
Table 2. Potential Injury from Strangulation |
|
Types |
Injuries |
Physical injury |
|
Neuropsychological injury |
|
The post-injury phase results in agitation, memory impairment, and loss of consciousness and can progress to airway edema and respiratory failure. Table 3 shows a timeline of the sequence of physiological events that occur during strangulation that involves occlusion of the arterial blood flow.
Table 3. Physiological Consequences from Occlusion of the Carotid Arteries |
|
Time |
Event |
0 |
Pressure applied to occlude carotid arteries |
5-10 seconds |
Onset of unconsciousness |
11-17 seconds |
Anoxic seizure |
15 seconds |
Urinary incontinence (loss of bladder control) |
30 seconds |
Rectal incontinence (loss of bowel control) |
60-160 seconds |
Respiration ceases/death |
Adapted from: Carter R, Smock B, Strack G, et al. Physiologic consequences of strangulation. Alliance for Hope International. https://www.familyjusticecenter.org/resources/physiological-consequences-of-strangulation-seconds-to-minute-timeline-2/ |
|
Clinical Features
Historical Features
History. An environment of safety and security is crucial for providing patient care and establishing rapport in situations associated with hanging and strangulations. Depending on the situation or concern for IPV, the interview and/or examination may be conducted after the partner has been asked to leave the room. If the partner is present, optimize privacy as much as can be allowed.
As little as 10% of victims are comfortable enough to openly disclose assault to medical staff, likely driven by a myriad of emotions, including fear, shame, and guilt, so partnering with the patient and using supportive language may increase the likelihood of obtaining an accurate history.1,20,21 A high index of suspicion for IPV should be maintained in patients with multiple emergency department (ED) visits or in patients with chief complaints of acute onset dysphagia, neck pain, headache, odynophagia, or hoarse voice.1,22 Routine IPV screening should be implemented in all women of childbearing age regardless of presentation.20
If there is immediate concern for the patient’s safety, hospital security and appropriate medical staff should be notified of the situation.20 For those whose injuries are from a possible suicide attempt, suicide precautions and a physician hold to prevent elopement should be enforced.
Strangulation. Patients who seek emergency care after strangulation do not necessarily have a uniform presentation. In fact, many patients may not mention strangulation in the history they relate to their medical providers. In many cases, the strangulation that occurred may leave no physical evidence, and patients may have a variety of reasons not to disclose that this had occurred, such as concerns for retribution, not wanting the perpetrator to be prosecuted, embarrassment, or fear of judgment or marginalization.1,13 In up to two-thirds of cases, patients may be asymptomatic from the strangulation and may not prioritize it in their history because they have sought care in the ED for reasons besides the strangulation itself — concerns for sexually transmitted infections or requesting pregnancy testing, for instance.23,24
Victims of strangulation may minimize the trauma of what occurred to them when speaking with healthcare providers, perhaps unaware of the gravity of what they have experienced or because of normalization of encounters like this through repeated prior experiences with aggressors.9 Additionally, survivors of strangulation may not be capable of providing a reliable linear history. Memory of the event may be imperfect because of the effects of drugs or alcohol, the extreme stress and duress of the experience, or from interruption of blood flow to the brain itself.1
For the medical provider, uncovering that strangulation has occurred may require thoughtful questioning coupled with a high index of suspicion in cases where the patient does not volunteer that it has occurred or where the physical exam does not provide clues. Asking open-ended questions may yield valuable information, but alternate strategies with closed-ended or direct questions (such as “Was any pressure applied to your neck?”) also may lead a patient to disclose more information about what occurred.9 If not explicitly endorsed or denied by the patient, it is important to directly question about whether a sexual assault has taken place, since this likewise may not be immediately volunteered by the patient, and timely medical care can be provided in that scenario.
For those patients who come in directly endorsing a strangulation, symptoms can vary depending on the severity of the strangulation itself. During the strangulation event itself, many patients describe a sensation of being unable to move, which is a phenomenon that has been described as far back as the 1940s.25 In severe strangulation, loss of consciousness, loss of bowel and bladder continence, and even seizures can occur. Patients may lose memory of the event, as previously noted, which can decrease their ability to relate linearly the events that took place prior to arrival.9
If patients arrive symptomatic to the ED, they may complain of neck pain, voice changes, difficulty swallowing, rashes on the face, changes in vision, chest pain, and/or dyspnea. Traumatic injuries to the head and neck may lead to pain and may be a chief concern for the patient. In cases where the strangulation has led to vascular injury, patients can present with strokes or stroke-like syndromes.9,23,24
Beyond the physical manifestations of the violence, strangulation is a terrifying ordeal for the survivor, and psychiatric symptoms also frequently are part of patient presentations to the ED, not only on their index visit in the form of an acute stress reaction, but also further into the future. Post-traumatic stress disorder and suicidal ideation can be seen as a result of strangulation.23 Special attention should be paid to this component of the patient encounter. While the physical manifestations of strangulation are critical to address, psychiatric concerns are equally important to treat as part of holistically caring for the patient after the traumatic event.
It also is important to note that accurate documentation of the encounter in the medical record is important, as notes may be used in criminal proceedings in the future.9
Near Hanging. For near hanging, any information gathered from the patient, bystanders, or emergency medical services (EMS) will be helpful in determining prognosis and will help dictate management.26 Near hangings, whether complete or incomplete, often lack significant structural injury, and harm/death is due to hypoxia.27,28 Symptom patterns in near hanging cases may mirror some of the symptoms mentioned earlier for patients who have been strangled, but other specific considerations need to be made when taking a history for a patient who has experienced a near hanging. Most cases of near hanging are from suicide attempts, so confirmation of the circumstances of the event is critical.29 Question the patient, bystanders, or EMS personnel about the height of the drop, as well as the position of the body when found. Significant force from the body weight is present when the body is suspended off the ground. Less force is present if the body is partially or completely in contact with the ground or floor. Most intentional hangings do not have a drop, in contrast to judicial hangings for capital punishment where the patient does fall a distance during the hanging, which increases the forces at play and the risk of significant structural damage to the neck.18,28,30 It is important to ask about whether the patient may have ingested any substances as part of their suicide attempt. Up to 70% of patients who come to the ED after near hanging have positive toxicological studies for ingestions of drugs.18
Physical Examination Findings
A thorough physical examination is critical to ensure all injuries are identified and strategies for assessment or intervention can be determined. A significant percentage of patients who have survived a strangulation or near hanging may arrive asymptomatic and, similarly, may have no outward signs of trauma on physical examination. In patients with darker skin complexion, external signs of bruising and petechiae may be more subtle than on lighter skin complexions.2,9 However, the absence of external signs such as bruising does not preclude the possibility of a significant internal injury, so careful examination is paramount.
On initial presentation, physical examination should focus on airway, breathing, and circulation (the ABCs) as in any patient who arrives after a trauma. Signs of airway or breathing compromise, such as drooling, subcutaneous air, muffled or absent voice, distortions of airway anatomy, or respiratory distress may necessitate immediate intervention, discussed later.9,24 Similarly, signs of vascular injury in the neck might include audible bruits on auscultation, or the neurological sequelae from neck vascular injury, such as stroke symptoms (focal neurological deficits) or Horner’s syndrome (unilateral ptosis, miosis, facial anhidrosis). In cases of particularly severe brain injury, a patient may have a globally reduced level of consciousness.
After securing the ABCs and assessing for neurological disability, a careful head-to-toe secondary assessment should occur. Examination of the patient should include inspection for ligature marks (see Figure 1), bruising, scratches (from the patient’s attempts to resist strangulation by the assailant), or other traumatic injuries to the neck.23 Subconjunctival hemorrhages and petechiae (known eponymously as Tardieu spots) above the level of the strangulation can occur from the increased intravascular pressure resulting from compression of the vessels of venous return in the neck.20,23,28,30 (See Tables 4 and 5.)
Figure 1. Ligature Marks |
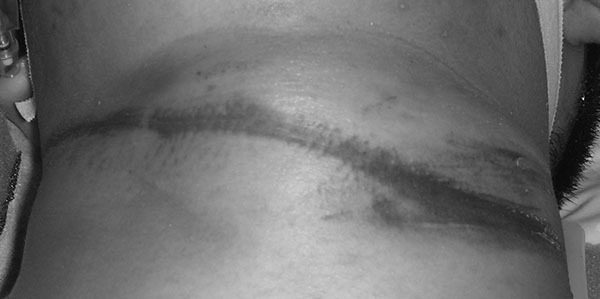 |
Image courtesy of J. Stephan Stapczynski, MD. |
Table 4. Symptoms with Strangulation/Near Hanging |
|
Type |
Symptoms |
Neurological |
|
Head, ears, eyes, nose, and throat |
|
Cardiovascular |
|
Respiratory |
|
Table 5. Physical Examination Findings with Strangulation/Near Hanging31 |
|
Type |
Findings |
Neurological |
|
Head, ears, eyes, nose, and throat |
|
Cardiovascular |
|
Respiratory |
|
Diagnostic Studies
Multiple organizations have created guidelines for the assessment and imaging of strangulation injuries. One valuable resource is the Family Justice Center Alliance (https://www.familyjusticecenter.org/about-us/). Therefore, history and clinical presentation, as well as institutional policy, should guide diagnostic studies and workup. It has been reported that strangulated patients with a normal Glasgow Coma Scale (GCS) score or those with no physical exam findings have a lower rate of clinically significant injury, and it has been suggested in the literature that clinicians implement a tailored approach for each patient depending on presentation.3 However, the practitioner should keep in mind that injuries may be harder to identify in patients with darker pigmented skin. Being intentional about identifying any injuries present may help mitigate known risks of health and racial disparities for those with darker complexions.2 It has been well documented that those with little to no physical signs of strangulation are at risk of an underlying life-threatening injury.12 Therefore, clinicians should maintain a high index of suspicion for potential injury in this patient population.
Laboratory Studies
When suspicious for a strangulation-related injury, ancillary testing with laboratory and imaging studies can help diagnose and characterize the extent of injury. Laboratory evaluation typically is not required in the workup of strangulation or hanging; however, it can be added if deemed necessary in the clinical scenario. There are no reliable laboratory tests in the diagnosis of strangulation-related injuries.26
For stable patients who can give a history, no laboratory tests are necessarily needed. If the patient is cooperative, the provider should screen for intoxication or intentional drug overdose. If evidence is present, by the patient’s history, the patient’s behavior, or EMS description of the scene, obtain serum toxicology, urine drug screen, and electrocardiogram (ECG).18
For patients who are altered or unresponsive, additional laboratory tests like complete blood count (CBC), complete metabolic panel (CMP), coagulation screens, lactic acid, and blood gas should be collected as well. Pregnancy testing should be obtained in all biologically female patients of child-bearing age, since there is a high, and likely underreported, incidence of IPV and sexual assault in this population.30,32
Imaging
In patients for whom imaging is indicated, the first-line imaging is computed tomography (CT) scan. CT is the diagnostic modality of choice for evaluation of strangulation injuries, with CT angiogram (CTA) of the neck the most common diagnostic study performed in this population. It is the fastest and most useful in assessing for anoxic, structural, and vascular injuries for patients who are symptomatic or are asymptomatic with significant risk factors.18,30,33 This radiological study aims to identify both injury to bony/osseous structures as well as vulnerable neck vasculature.27 Although sensitivity and specificity of CTA for strangulation are not well documented, the diagnostic yield of CTA in this population ranges from 2% to 7%.27,33,34 This low yield is due in part to the infrequency of severe injury. In patients with a reassuring neurologic exam and low suspicion for blunt cerebrovascular injury (BCVI), it is reasonable to order a CT neck without angiography to evaluate for non-vascular injuries.35
There is limited utility of ultrasound, X-ray, or magnetic resonance imaging (MRI) for strangulation-related injury. MRI and ultrasound may be beneficial for soft tissue and vascular injury; however, due to the length of time required for MRI and the limitations inherent to technique for ultrasound compared to CT, these are regarded as adjunct studies that can be performed inpatient or on an outpatient basis.27,30 Nevertheless, sequelae of strangulation injuries and concomitant trauma should be evaluated with appropriate imaging based on the physical exam findings and presence of additional trauma.
Differential Diagnosis
The differential diagnosis for strangulation and hanging injuries is broad and affects multiple systems due to the structures of the neck. Table 6 demonstrates the systems-based approach to differential diagnosis after trauma to the neck.
Table 6. Hanging and Strangulation-Related Injuries |
Respiratory
Vascular/Neurologic
Cardiac
Soft Tissue/Musculoskeletal
Gastrointestinal
Endocrine
Psychiatric
Other
|
Management
Prehospital Management
Prehospital management of both strangulation and hanging victims follows the same essential blueprint: clear the scene, identify those in need of care, address immediate needs, and transport those requiring medical evaluation to the closest appropriate facility. However, each mechanism of blunt neck trauma is associated with different situations. Hanging often is seen as a method for a suicide attempt, while strangulation is more commonly seen in IPV. Each has different elements that EMS may encounter upon arrival to the scene.
In cases of potential NFS, if there still is concern for safety for either the patient or EMS staff, law enforcement should be present for deterrence or to manage any conflict that may ensue.26 Recognizing subtle signs and symptoms is crucial in identifying people in need of further evaluation.26 Assessment focused on ABCs, vital signs, and neurologic status should be completed promptly while gathering information from the patient or bystanders prior to transporting the patient to the nearest ED.
Cases of hanging or near hanging may require freeing the patient from the ligature without worsening existing or causing new injuries and while searching for signs of life. Stabilization of the head and neck should be maintained as assessment of ABCs is done and vitals are taken. If necessary and depending on local EMS protocols, support with supplemental oxygen delivered by nasal cannula, non-rebreather, or bag-valve-mask. Airway adjuncts like oropharyngeal airways, laryngeal mask airways, or endotracheal (ET) tubes can be considered to maintain adequate oxygenation as indicated.7 A mental note of the environment should be taken, since empty medication bottles or alcohol bottles nearby may suggest multiple concerns or suicide modalities at play and offer valuable information for emergency providers.18
Refusal of Transport
First responders, in addition to other health professionals, have a unique and potentially pivotal role in identifying and assessing IPV and NFS.13 While we cannot force people into coming to the ED for an assessment, efforts should be made to persuade high-risk individuals to come in for evaluation.
Some patients who are identified as victims of strangulation may be unaware of the potential of developing complications that stem from the assault or the significantly increased risk they have of homicide and require education to make a fully informed decision. Others may lack confidence in the medical team’s ability to provide safety.4 After even one incident of strangulation, a woman’s risk of death increases 750%, and complications from the episode may present as long as seven days after the insult.4,36 Any patient injured by strangulation or hanging should be transported via EMS to the closest ED, and concise reports of obtained information from the patient or bystanders, vitals, evidence of intent, and the extent of prehospital care should be given to the ED providers who are assuming care.18,26
Hospital Management
The initial stabilization and treatment of hanging and strangulation patients follow the same algorithm. Prior to patient arrival, trauma alert activation per facility policies and based on information received should be done to mobilize necessary services and resources for incoming patients. For those who arrive by private vehicle, activation should be done at time of triage based on presenting injuries if meeting local criteria. Initial assessment follows the Advanced Trauma Life Support (ATLS) algorithm, focusing on the ABCs, disability as defined by the GCS, and followed by a head-to-toe assessment of the patient.7 The overall goal of any emergency intervention during the primary survey is to prevent further hypoxia or hypoperfusion, thus protecting the brain and spinal cord from additional damage. Whether or not a formal trauma alert is activated, given the nature of injury and the associated risks, full-body assessment should be completed. History should be obtained from patients at an appropriate time and should not delay urgent intervention.
ABC Management
For stable, alert, and cooperative patients, an evaluation for airway patency through interview (i.e., ability of the patient to speak with a normal-sounding voice) and assessment of vital signs are sufficient in the initial ABC survey. For unstable or critically ill patients, a definitive airway should be established with consideration for neuroprotection against hypoxia and for prevention of aspiration. Evaluate all patients for the potential of spinal injury and institute immobilization as appropriate.
Airway. For those patients with inability to protect their airway, intubation is required. With patients with high concern for vascular injury, it is crucial to limit hypoxia and/or hypoperfusion to the brain, since this is a leading cause of morbidity and mortality for this patient population.7 A difficult airway should be anticipated, with emphasis on single-pass intubation and minimizing further damage to the surrounding structures. Suction, bag-valve-mask, and backup airway method, like a cricothyrotomy kit, should be ensured to be functional and present at the bedside. Cervical spine immobilization should be maintained during an intubation attempt, either by keeping a c-collar in place or via two-person manual in-line stabilization. Rapid sequence intubation (RSI) with hyperangulated video-assisted laryngoscope and a rigid stylet is recommended while c-spine precautions are in place. For patients with evidence of polytrauma and concern for midface instability, an alternative approach to intubation may be considered. A traditional laryngoscope can be used with staff maintaining c-spine immobilization when the c-collar is removed. Another alternative is the use of fiberoptic awake intubation to protect the remaining integrity of the facial bones while simultaneously allowing for internal visual assessment of the larynx.24 Fiberoptic intubation, especially if performed non-emergently, should only be used if time permits and if providers are sufficiently trained in the use of this equipment. Cricoid pressure should be avoided in hanging and strangulation patients since this may worsen existing injuries.
While maintaining c-spine precautions during intubation generally is recommended, in an unstable patient in whom intubation cannot be completed using the techniques mentioned earlier, it is reasonable to release neutral positioning of the neck to facilitate a definitive airway. The overall incidence of spine injuries is low, and the benefits of an established airway almost certainly outweigh the risk of additional injury. A chest X-ray will be required to assess placement of the endotracheal tube.
Breathing. Similar to the approach for all trauma patients, once the airway is established, the provider should transition to assessment of the respiration and circulation. Strangulation and hanging injuries typically do not affect the lungs. However, in IPV, there may be concomitant injuries to other parts of the body and, as such, a systematic approach is crucial. Listen to breath sounds as the patient breathes or the ventilator moves air. If there is concern for pneumothorax, adjuncts such as chest X-ray or ultrasound should be used to assess lung aeration and lung slide, respectively. If a pneumothorax or hemothorax is present, needle decompression is warranted if tension physiology is present. Subsequent chest tube placement should follow.
Circulation. For assessment of circulation, the blood pressure of critically ill patients should be augmented through fluid boluses with isotonic fluids, blood products, or vasopressors to achieve a strict mean arterial pressure (MAP) goal of > 85 mmHg for neuroprotection.7 Once stabilized, the secondary survey, or head-to-toe exam, may begin.
Disability. The GCS can help to guide management in this patient population. Patients with lower GCS on arrival are more likely to have sustained significant injuries.6 EMS GCS on scene, initial GCS on arrival, and any changes to GCS must be documented and can be used to direct further workup.
Secondary Survey
A complete physical examination should be conducted with close attention to the eyes, mouth, and neck.18 If missed on the primary survey, the presence of any “hard signs” associated with the neck or throat, such as a hoarse voice, inability to manage secretions, presence of subcutaneous emphysema, new thrill or bruit, or a rapidly enlarging mass, indicates significant airway injury and should prompt reconsideration of definitive airway management.7,18,30,37 A careful skin exam should be completed, looking for petechial hemorrhages or ligature marks.18 Thorough documentation of the extent of injury and, if the patient consents, pictorial documentation should be obtained as feasible to enhance continuation of care and can be useful in any legal proceedings that may occur.12 While a large majority of patients who experience blunt neck injury via strangulation or hanging lack bruising or ligature marks, this does not indicate the level of internal trauma, and this should be noted in documentation in addition to symptoms the patient experiences.4,12,38
Continued Management
After initial stabilization has occurred, additional steps should be taken in stable patients. Patients with suspected strangulation injuries also must be screened for sexual assault.39 For those who disclose sexual assault, a Sexual Assault Nurse Examiner (SANE) should be offered, if available, and within the allotted time frame.23 The timing of the SANE exam varies by state, but it is best done within 72 hours after the incident.4
Beyond ATLS, critically ill patients require continuous cardiac, oxygenation, and neurologic monitoring in addition to glycemic control until they are able to be transferred to the intensive care unit (ICU). Emphasis on lung protective ventilation and blood pressure management is associated with reduced mortality in patients with hanging injuries.7,40 Frequent GCS calculations and neurologic exams should be done to monitor for progressive damage in all stable patients. In those with traumatic brain injury (TBI), antiepileptic prophylaxis may be considered.
Imaging
Several organizations have developed imaging recommendations for the strangulation victim. The Family Justice Center Alliance recommends CT angiography of the carotid and vertebral vessels is the initial imaging study.41 However, many patients do not sustain clinically significant bodily injuries, and advanced imaging may not be indicated in all scenarios.26 The use of imaging should be guided by physical exam, mechanism of injury, and concern for concomitant traumatic injuries. Decisions on when to image stable, well-appearing patients can be augmented by clinical decision tools on a case-by-case basis. Tools such as the NEXUS criteria aid in determining the need for cervical spine imaging in stable patients, and the Denver or Memphis criteria are helpful for detection of blunt cerebrovascular injury.7
Several sources report a significant association between GCS and severe injury. All severe injury — vascular, laryngeal, and bony — occurred in patients with GCS less than 15 on presentation.18,27,35
Consults
Evidence of bony, laryngeal, or vascular injury should trigger a neurosurgery; ear, nose, and throat (ENT); or vascular surgery consult, respectively. Any patient awaiting surgical evaluation should remain NPO and avoid nonsteroidal anti-inflammatory drugs (NSAIDs) until a determination is made of whether a surgical procedure is needed.18 Patients with focal neurologic deficits or altered mental status should have a neurology consultation for additional considerations in management and treatment for the patient.18,42 Psychiatry should be consulted on patients who attempted suicide.
Consider both the present physical injuries and the social situation of the patient. If the patient is presenting because of or if there is concern for IPV, social work/case management should be consulted. With a single event of strangulation with IPV, the risk of homicide significantly increases.12 In addition, the presence of IPV further complicates the patient’s case, as emotional, financial, and other interpersonal factors may be involved in coercive control and require many additional resources outside of the medical system for which social workers and case managers may be indispensable.5
Additional Aspects
The preference of an adult patient must be honored regarding reporting or police involvement after a strangulation assault. The exception is with minors, people with intellectual disabilities, or elderly populations, for whom healthcare providers are mandatory reporters of abuse. There is varying jurisdiction in such situations; however, it is important to inform the patient when reporting takes place, since this alone can pose safety concerns and fear of retaliation.9 In patients who experienced a self-inflicted hanging injury, proper measures should be pursued to ensure their safety. State legislation will vary regarding psychiatric holds, and the clinician should follow local guidelines. After medical stabilization of the patient with self-inflicted injuries, emergency providers can refer to mental health professionals for continuation of the patient’s care.
ED response to the strangulated patient varies, and victims can be apprehensive about seeking care.43 This is perpetuated by lack of training, stigma, and fear of ED staff to engage patients who have experienced strangulation.13 Although it is common practice for EDs to screen for IPV, generalized screening can miss those who have been strangled or are at an increased risk of strangulation. Collaboration through interdisciplinary teams can help to advance awareness of NFS as a result of IPV and also allow for the dissemination of resources and clinical tools.1 It has been recommended that validated screening tools that include strangulation-related questions be used.44 Such screening tools include the Abuse Assessment Screen and the Danger Assessment-5.45,46 There are no current screening tools for men.
Because injuries related to strangulation can be subtle, it is of paramount importance that staff screen, recognize, and document their findings. The act of specifically inquiring about details of the strangulation or elements within assault that lead to an increased risk of strangulation potentially can be life-saving.47 Furthermore, explicit documentation has been shown to be helpful for victims for both follow-up care and legal proceedings.44 This is particularly important for patients who lack overt signs, symptoms, or objective injury secondary to strangulation.48
The medical care for a strangulated patient continues after the initial ED visit. Complications and sequelae from strangulation injuries are likely underreported and can take weeks to present, highlighting the importance of follow-up care.12 Beyond physical injury, those who have had a strangulation injury furthermore have been shown to perform more poorly in memory testing, suggesting that strangulation can result in a spectrum of traumatic brain injury.49
The care of a patient who has been strangled is complex and multidisciplinary, requiring input from clinicians, nurses, and social workers. There are no standardized guidelines for the care of such patients, underscoring the urgent need for the development of best practice recommendations.
Complications
Cardiac Arrest. Cardiac arrest is a usually irreversibly fatal complication of strangulation or hanging. A large portion (up to half) of critically ill hanging victims decompensate into cardiac arrest.50 Survival rates to discharge drop to as little as 3% when this occurs, and those who do survive often have moderate to severe disability. Unfortunately, the increase in bystander initiation of cardiopulmonary resuscitation (CPR) has not translated to improved outcomes at this time.19 Targeted temperature management, when employed, is controversial in this patient population.50,51
Neurogenic Shock. A rare but serious complication of severe neck injury is neurogenic shock. Neurogenic shock should be considered as a diagnosis of exclusion, meaning that other causes of hypotension (hypovolemic, cardiogenic, obstructive, and septic) should be considered and treated before making a definitive diagnosis.28
Stroke. Stroke can be an immediate or late presenting complication of hanging or strangulation. Both hemorrhagic and ischemic/watershed stroke types can occur from arterial ruptures and decreased oxygenation, respectively.52,53 Blunt cerebrovascular injury (BCVI) may occur in both strangulation and hanging, occurring in up to 3% of polytrauma patients, and increases the risk of stroke up to 40% in the first week after injury.10,37 For patients who do not have obvious injury on imaging, consider initiating aspirin to prevent the development of stroke.54 Further management and treatment decisions can be made in conjunction with a neurology consultant.
Disposition
Admission
Admission may be required depending on the severity and complexity of injury identified or the need for continued observation. Consider admission to intensive care units for patients who require airway monitoring or close neurovascular monitoring. For those who initially are stable, if symptoms develop or persist during the ED observation period of four to six hours despite lack of imaging findings, the patient should be considered for admission.3,30
Transfer
Patients presenting after strangulation may require transfer to a trauma center if resources at the current hospital are limited or insufficient regarding the patient’s injuries, not solely because of the mechanism of injury.29 For example, for stable patients who present after a failed suicide attempt, transfer to another facility for inpatient psychiatric care can occur after their initial workup and observation if the resource for the workup is available.37 Additionally, the prognosis may help dictate the ability or utility of transferring critically ill patients. For example, those who go into cardiac arrest secondary to a hanging injury have an exceedingly low survival rate to hospital discharge.55 Clinicians may elect to proceed with a shared decision-making discussion with family of critically ill/post-cardiac arrest patients and consults to decide together whether to pursue transfer to a tertiary care facility. Information regarding prognosis and potential sacrifices on the patient/family side with distance (such as potential inability to spend time together) can be considered as factors in this decision.29
Discharge
In the event a patient is observed for four to six hours without symptoms, and they are not considered a harm to themselves or others, they may be a candidate for discharge. These patients should be discharged into the care of trusted family or friends who are able and willing to monitor for symptoms over the next 12-36 hours, since this is when most complications or lethal symptoms appear, and bring them back to the ED if they do develop.4,30 Both parties should be educated on symptoms, need for evaluation and intervention, any safety plans developed with specialists, risks of non-compliance, and importance of primary care follow-up.9 Physical discharge instructions should include a list of symptoms, any follow-up appointments, and any resources provided from consultants, social workers, and case managers.
Summary
Strangulation encompasses hanging, manual strangulation, and ligature strangulation and is defined as the application of direct pressure against a person’s neck, occluding or injuring blood vessels and/or the airway. Labeled “the edge of homicide,” for those patients who have experienced an NFS, the victim has a sevenfold increased risk of attempted murder by the same abusive partner, and the risk of death increases by a factor of eight. Strangulation and hanging injuries are underidentified by healthcare providers, often because of the lack of external physical signs of trauma. A systematic approach to clinical evaluation and treatment, using an interdisciplinary team, is important to ensure positive outcomes for this vulnerable patient population.
References
- Bergin A, Blumenfeld E, Anderson JC, et al. Describing nonfatal intimate partner strangulation presentation and evaluation in a community-based hospital: Partnerships between the emergency department and in-house advocates. J Head Trauma Rehabil 2022;37:5-14.
- Brady PQ, Zedaker SB, McKay K, Scott D. The darker the skin, the greater the disparity? Why a reliance on visible injuries fosters health, legal, and racial disparities in domestic violence complaints involving strangulation. J Interpers Violence 2023;38:7602-7629.
- Matusz EC, Schaffer JT, Bachmeier BA, et al. Evaluation of nonfatal strangulation in alert adults. Ann Emerg Med 2020;75:329-338.
- Hartlaub T, Castro B, Frey M. Nonfatal strangulation: More than meets the eye. J Forensic Nurs 2022;18:189-192.
- Brady PQ, Fansher AK, Zedaker SB. How victims of strangulation survived: Enhancing the admissibility of victim statements to the police when survivors are reluctant to cooperate. Violence Against Women 2022;28:1098-1123.
- Berke DM, Helmer SD, Reyes J, Haan JM. Injury patterns in near-hanging patients: How much workup is really needed? Am Surg 2019;85:549-555.
- Coombs AE, Ashton-Cleary D. Hanging and near-hanging. BJA Educ 2023;23:358-363.
- Jacob B, Cullen N, Haag HL, et al. Assault by strangulation: Sex differences in patient profile and subsequent readmissions. Can J Public Health 2020;111:492-501.
- Victoire A, De Boos J, Lynch J. ‘I thought I was about to die’: Management of non-fatal strangulation in general practice. Aust J Gen Pract 2022;51:871-876.
- Kim DY, Biffl W, Bokhari F, et al. Evaluation and management of blunt cerebrovascular injury: A practice management guideline from the Eastern Association for the Surgery of Trauma [published correction appears in J Trauma Acute Care Surg 2020;89:420]. J Trauma Acute Care Surg 2020;88:875-887.
- Jordan KS, Murphy JA, Romine AJ, Varela-Gonzalez L. A case of nonfatal strangulation associated with intimate partner violence. Adv Emerg Nurs J 2020;42:186-195.
- De Boos J. Review article: Non-fatal strangulation: Hidden injuries, hidden risks. Emerg Med Australas 2019;31:302-308.
- Donaldson AE, Hurren E, Harvey C, et al. Front-line health professionals’ recognition and responses to nonfatal strangulation events: An integrative review. J Adv Nurs 2023;79:1290-1302.
- Matias A, Gonçalves M, Soeiro C, Matos M. Intimate partner homicide: A meta-analysis of risk factors. Aggression and Violent Behavior 2020;50:101358.
- Centers for Disease Control and Prevention. Fast Facts: Preventing intimate partner violence. Centers for Disease Control and Prevention. Last reviewed Oct. 11, 2022. https://www.cdc.gov/violenceprevention/intimatepartnerviolence/fastfact.html
- Bugeja L, Rowse J, Cunningham N, Parkin JA. Non-fatal strangulation and COVID-19 common symptoms and signs: Considerations for medical and forensic assessment. Forensic Sci Med Pathol 2022;18:165-169.
- Bichard H, Byrne C, Saville CWN, Coetzer R. The neuropsychological outcomes of non-fatal strangulation in domestic and sexual violence: A systematic review. Neuropsychol Rehabil 2022;32:1164-1192.
- Dorfman JD. Near hanging: Evaluation and management. Chest 2023;163:855-860.
- Alqahtani S, Nehme Z, Williams B, et al. Temporal trends in the incidence, characteristics, and outcomes of hanging-related out-of-hospital cardiac arrest. Prehosp Emerg Care 2020;24:369-377.
- Sachs CJ. Intimate partner violence and abuse. In: Walls R, Hockberger R, Gausche-Hill M, et al. Rosen’s Emergency Medicine: Concepts and Clinical Practice, 10e. Elsevier Health Science; 2022:2438-2445.
- Basheer MB, Bell R, Boyle AA. Systematic review of the effectiveness of advocacy interventions for adult victims of domestic violence within an emergency department setting. Cureus 2022;14:e25599.
- Giusti R, Ravi A. Strangulation as a cause of dysphagia. Am Fam Physician 2021;104:118-119.
- Buchanan JA, Selby ST. Sexual assault. In: Walls R, Hockberger R, Gausche-Hill M, et al. Rosen’s Emergency Medicine: Concepts and Clinical Practice,10e. Elsevier Health Science; 2022:2421-2437.
- Bean AS. Trauma to neck. In: Tintinalli JE, Ma O, Yealy DM, et al eds. Emergency Medicine: A Comprehensive Study Guide, 9e. McGraw Hill; 2020:1722-1729.
- Kabat H, Anderson JP. Acute arrest of cerebral circulation in man: Lieutenant Ralph Rossen, (MC), U.S.N.R. Arch NeurPsych 1943;50:510-528.
- Stellpflug SJ, Weber W, Dietrich A, et al. Approach considerations for the management of strangulation in the emergency department. J Am Coll Emerg Physicians Open 2022;3:e12711.
- Hopkins B, Wang A, McKendy K, et al. A retrospective analysis of the clinical use and utility of advanced imaging in the evaluation of near-hanging and strangulation injuries at a Canadian Level One Trauma Centre. Injury 2023;54:110978.
- Hua A, Shah KH, Garg M, et al. A hanging and its complications. J Emerg Med 2016;51:691-696.
- Mitra B, Maiden MJ, Read D, et al. Definitive management of near-hanging at major versus non-major trauma centres. Emerg Med Australas 2023;35:849-854.
- Dunn RJ, Sukhija K, Lopez RA. Strangulation injuries. In: StatPearls. StatPearls Publishing; April 22, 2023.
- Rozzi HV, Riviello R. How to evaluate strangulation. ACEPNow. Published April 17, 2019. https://www.acepnow.com/article/how-to-evaluate-strangulation/
- Román-Gálvez RM, Martín-Peláez S, Martínez-Galiano JM, et al. Prevalence of intimate partner violence in pregnancy: An umbrella review. Int J Environ Res Public Health 2021;18:707.
- Patch M, Dugan S, Green W, Anderson JC. Emergency evaluation of nonfatal strangulation patients: A commentary on controversy and care priorities. J Emerg Nurs 2022;48:243-247.
- Zuberi OS, Dixon T, Richardson A, et al. CT angiograms of the neck in strangulation victims: Incidence of positive findings at a level one trauma center over a 7-year period [published correction appears in Emerg Radiol 2020;27:577]. Emerg Radiol 2019;26:485-492.
- Ribaute C, Darcourt J, Patsoura S, et al. Should CT angiography of the supra-aortic arteries be performed systematically following attempted suicide by hanging? J Neuroradiol 2021;48:271-276.
- Pelucio MT, Salzman J, Dragoo D. Dissemination strategies of a nonfatal strangulation program: Success of an interagency initiative. J Emerg Med 2022;63:426-454.
- Newton K, Claudius I. Neck trauma. In: Walls R, Hockberger R, Gausche-Hill M, et al. Rosen’s Emergency Medicine: Concepts and Clinical Practice, 10e. Elsevier Health Science;2022:368-375.
- Sharman LS, Fitzgerald R, Douglas H. Medical evidence assisting non-fatal strangulation prosecution: A scoping review. BMJ Open 2023;13:e072077.
- Cannon LM, Bailey JM, Ernst SD, et al. Examining trends in non-fatal strangulation among sexual assault survivors seeking Sexual Assault Nurse Examiner care from 2002 to 2017. Int J Gynaecol Obstet 2020;149:106-107.
- Tharmarajah M, Ijaz H, Vallabhai M, et al. Reducing mortality in near-hanging patients with a novel early management protocol. Am J Emerg Med 2018;36:2050-2053.
- Family Justice Center Alliance. Recommendations for the medical/radiographic evaluation of acute adult non/near fatal strangulation. Oct. 13, 2023. https://www.familyjusticecenter.org/resources/recommendations-for-the-medical-radiographic-evaluation-of-acute-adult-adolescent-non-near-fatal-strangulation/
- Heimer J, Tappero C, Gascho D, et al. Value of 3T craniocervical magnetic resonance imaging following nonfatal strangulation. Eur Radiol 2019;29:3458-3466.
- Patch M, Anderson JC, Campbell JC. Injuries of women surviving intimate partner strangulation and subsequent emergency health care seeking: An integrative evidence review. J Emerg Nurs 2018;44:384-393.
- Patch M, Farag YMK, Anderson JC, et al. United States ED visits by adult women for nonfatal intimate partner strangulation, 2006 to 2014: Prevalence and associated characteristics. J Emerg Nurs 2021;47:437-448.
- Laughon K, Renker P, Glass N, Parker B. Revision of the abuse assessment screen to address nonlethal strangulation. J Obstet Gynecol Neonatal Nurs 2008;37:502-507.
- Messing JT, Campbell JC, Snider C. Validation and adaptation of the Danger Assessment-5: A brief intimate partner violence risk assessment. J Adv Nurs 2017;73:3220-3230.
- McKee GB, Gill-Hopple K, Oesterle DW, et al. New perspectives on risk factors for non-fatal strangulation and post-assault imaging. J Interpers Violence 2022;37:NP8226-NP8236.
- Reckdenwald A, Powell KM, Martins TAW. Forensic documentation of non-fatal strangulation. J Forensic Sci 2022;67:588-595.
- Valera EM, Daugherty JC, Scott OC, Berenbaum H. Strangulation as an acquired brain injury in intimate-partner violence and its relationship to cognitive and psychological functioning: A preliminary study. J Head Trauma Rehabil 2022;37:15-23.
- de Charentenay L, Schnell G, Pichon N, et al. Outcomes in 886 critically ill patients after near-hanging injury. Chest 2020;158:2404-2413.
- Kim JG, Choi HY, Kang GH, et al. Prognostic value of targeted temperature management on outcomes of hanging-induced out-of-hospital cardiac arrest: A nationwide observational study. Medicine (Baltimore) 2022;101:e28688.
- Sabrinskas R, Hamilton B, Daniel C, Oliffe J. Suicide by hanging: A scoping review. Int J Ment Health Nurs 2022;31:278-294.
- Bonow RH, Witt CE, Mossa-Basha M, et al. Aspirin versus anticoagulation for stroke prophylaxis in blunt cerebrovascular injury: A propensity-matched retrospective cohort study. J Neurosurg 2021;135:1413-1420.
- Turner J, Brown A, Boldy R, et al. Out-of-hospital cardiac arrest due to hanging: A retrospective analysis. Emerg Med J 2022;39:106-110.
- Messing JT, Campbell J, AbiNader MA, Bolyard R. Accounting for multiple nonfatal strangulation in intimate partner violence risk assessment. J Interpers Violence 2022;37:NP8430-NP8453.
Strangulation and hanging injuries are underidentified by healthcare providers, often because of the lack of external physical signs of trauma. A systematic approach to clinical evaluation and treatment, using an interdisciplinary team, is important to ensure positive outcomes for this vulnerable patient population.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
