New Advances in Cardiac Arrest Treatment
August 1, 2023
Reprints
AUTHORS
Natalie Diers, MD, Resident, Emergency Medicine Residency Program, UCF/HCA Florida Healthcare GME (Greater Orlando/Osceola)
Shayne Gue, MD, MSMEd, FACEP, Director of Education, Emergency Medicine Residency Program, UCF/HCA Florida Healthcare GME (Greater Orlando/Osceola), Assistant Professor of Emergency Medicine, University of Central Florida College of Medicine
PEER REVIEWER
William J. Brady, MD, FACEP, FAAEM, Professor of Emergency Medicine and Medicine, Medical Director, Emergency Preparedness and Response, University of Virginia Operational Medical Director, Albemarle County Fire Rescue, Charlottesville, VA
EXECUTIVE SUMMARY
- Approximately 80% of sudden cardiac death is attributed to coronary artery disease, and most patients will sustain a cardiac arrest due to the occurrence of a fatal ventricular arrhythmia.
- The four fatal rhythms observed in the majority of cardiac arrest cases are ventricular fibrillation, pulseless ventricular tachycardia, pulseless electrical activity, and asystole.
- Cardiac arrest associated with acute coronary ischemia usually is from arterial plaque rupture leading to occlusion of one or more coronary arteries producing polymorphic ventricular tachycardia that degenerates into ventricular fibrillation.
- Cardiac arrest in patients with chronic ischemic heart failure is associated with monomorphic ventricular tachycardia caused by reentrant loops of electrical activity around areas of damaged and scarred myocardium.
- Dual sequential defibrillation may be useful in cases of refractory ventricular fibrillation.
- Maintaining normothermia in patients resuscitated from an out-of-hospital cardiac arrest is just as effective as targeted temperature management.
Definition of the Problem
Cardiac arrest is a clinical syndrome defined as loss of cardiac contractility and function leading to loss of cerebral and systemic perfusion.1 It can be due to anatomic, metabolic, hematologic, or infectious etiologies, which can lead to cardiac arrhythmia, myocardial dysfunction, or alterations to vascular tone. The International Liaison Committee on Resuscitation (ILCOR) and other reporting agencies for cardiac arrest recommend categorizing cardiac arrest into events with external causes (e.g., drowning, trauma, asphyxia, drug overdose) or internal (medical) causes.2 Four major rhythms observed in the majority of cardiac arrest patients are: ventricular fibrillation, pulseless ventricular tachycardia, pulseless electrical activity (PEA), and asystole.
Cardiac arrest requires emergent medical intervention, with the goal of perfusing the brain and other major organs while attempting to reverse the underlying etiology causing the arrest. Cardiac arrest typically is described in the literature as occurring in either one of two settings: out-of-hospital cardiac arrest (OHCA) or in-hospital cardiac arrest (IHCA). Both presentations share similar treatment algorithms; however, there are differences in etiology and, thus, treatment between these inpatient and outpatient populations. Emergency physicians most often manage OHCA patients who have been resuscitated, as well as those IHCA patients who arrest in the emergency department (ED) or inpatient unit.
Relevancy
Approximately 50% of all cardiac-related deaths in the United States are caused by sudden cardiac arrest.1 There are approximately 350,000 emergency medical services (EMS)-attended OHCAs and an additional 210,000 reported sudden cardiac deaths in the adult population annually. The estimated national survival for EMS-treated OHCA is 10.8%.3 Since 2019, there has been a 119% increase in OHCAs, likely secondary to the coronavirus pandemic.4 A meta-analysis of six studies found an overall mortality of approximately 85% during the 2020 coronavirus pandemic as compared to 62% in previous years.5
Risk factors for the development of cardiac arrest include structural heart disease, inherited arrhythmia syndromes, pre-existing congenital heart disease, and heart failure. Chronic heart failure has a four- to tenfold increase in risk of sudden cardiac death.1 Cardiovascular disease, specifically coronary artery disease (CAD), also plays a significant role in the risk of cardiac arrest and sudden cardiac death. Approximately 80% of sudden cardiac death is attributed to CAD, and most patients will sustain a cardiac arrest due to the occurrence of a fatal ventricular arrhythmia.6 Most of the risk factors related to sudden cardiac death are those that also have an association with the development of CAD, including hypertension, diabetes, hypercholesterolemia, obesity, and smoking.4
Epidemiology
As previously stated, there are 350,000 EMS-attended OHCAs in the United States each year.1 Approximately 52% of EMS-treated adult OHCAs had resuscitation attempted in 2019.7 In the National Emergency Department sample for 2014, the weighted national rate for ED visits that included a diagnosis of “cardiac arrest or ventricular fibrillation” was 127 per 100,000 people.4 In cardiac arrest data from 2020, researchers found that in EMS-attended OHCA, 16.7% of patients were in a shockable rhythm (e.g., ventricular tachycardia, ventricular fibrillation).8
Patients with a shockable rhythm have a much higher chance of short-term survival compared to patients with a non-shockable rhythm. Specifically, survival to hospital admission was 44.5% in those with a shockable rhythm compared to 32.1% for those in PEA and 14.4% for those in asystole. Patients presenting in a shockable rhythm had a greater chance of survival to hospital discharge, at 26.0%, compared to 10% for PEA and 2% for asystole.8 However, it is important to note that survival to hospitalization after cardiac arrest varied between academic medical centers and was higher in hospitals with higher cardiac arrest volume, higher surgical volume, greater availability of invasive cardiac services, and more affluent catchment areas.9
The Cardiac Arrest Registry to Enhance Survival (CARES) 2020 annual report provided additional epidemiologic data reporting OHCAs most commonly occurred at a home or residence (73.9%), followed by a public setting (15.1%) and nursing homes (10.9%).8 In the majority of cases (50.1%), collapse was not witnessed by bystanders. Both CARES and international data found that OHCA is more common in men, with the proportion of patients approximately 60% male.8,10 Interestingly, women who presented with OHCA were older, more commonly presented in a non-shockable rhythm (e.g., asystole or PEA), and were more likely to receive layperson cardiopulmonary resuscitation (CPR).10 Despite some factors that would reduce chances of survival in women, they have equivalent or higher rates of survival to hospital discharge compared to men.
The Atherosclerosis Risk in Community (ARIC) study took place from 1985 to 2021 and measured how cardiovascular risk factors, access to health services, and outcomes varied by race, sex, location, and time.11 ARIC reported that 5.61% of Black and 2.95% of white participants experienced sudden cardiac death over the course of a 27-year follow-up. The authors also noted that patients with automatic implanted cardioverter defibrillators who developed ventricular dysrhythmias or sudden cardiac death within four years were higher among Black participants (42%) compared to white subjects (34%). Sudden cardiac death is 30% to 80% higher among residents in the lowest socioeconomic quartile compared with those in the highest, likely because of socioeconomic determinants of health, education/health literacy, and health access disparity.6
Pathophysiology
Two prospective autopsy studies of people with sudden cardiac death noted similar findings.12,13 One study analyzed patients with diagnosed heart failure or reduced ejection fraction (EF) after recent myocardial infarction (MI) enrolled in a randomized trial of valsartan therapy.12 The second was a community-based study from San Francisco of out-of-hospital sudden cardiac death.13 In each study, autopsy found approximately one-half of the deaths had no objective findings, in which case the cause of sudden cardiac death was presumed to be arrhythmic. In the other half of patients, there were objective findings at autopsy to support etiologies such as acute MI, cardiac rupture, acute heart failure, and pulmonary embolism. In the community-based study, when the initial rhythm recorded by EMS was found to be ventricular fibrillation or ventricular tachycardia, the autopsy findings were more likely to be consistent with sudden arrhythmic death. In contrast, those patients with an initial rhythm of PEA were far more likely to have anatomical cause of death (judged a non-arrhythmic sudden death), such as stroke, tamponade, pulmonary embolism, drug overdose, hemorrhage, etc.13
Coronary Artery Disease
CAD is a known risk factor for the development of sudden cardiac death. Based on the known progression of CAD, there are two major mechanisms that can explain fatal ventricular arrhythmias: acute coronary ischemia and ischemic cardiomyopathy. Acute coronary ischemia usually is associated with arterial plaque rupture leading to occlusion of one or more coronary arteries. This mechanism is more associated with polymorphic ventricular tachycardia, and these patients are more likely to have normal left ventricular (LV) function.6
Patients with previous MI who have developed an ischemic cardiomyopathy with decreased LV function are more likely to develop monomorphic ventricular tachycardia. These patients will develop reentrant loops around the areas of damaged and scarred myocardium.6 This usually takes years after the infarction to occur; the SWEDEHEART study published in 2020 found that the incidence of OHCA within 90 days of MI was
< 0.3%.14
Cardiomyopathy and Reduced LV Function
Cardiomyopathy is the distortion of normal cardiac myocyte anatomy. (See Figure 1.) There can be ischemic (as noted earlier) and non-ischemic etiologies leading to decreased LV function. Dilated ventricles lead to a disorganized dispersion of electrical currents through the cardiac conduction pathways. This can lead to “islands” of ventricular tissue to depolarize and repolarize at different rates, leading to reentrant pathways and facilitating ventricular tachyarrhythmias. Other anatomical distortions, such as left ventricular hypertrophy resulting from systemic hypertension and valvular disease or conduction disturbances such as left and right bundle branch blocks, can lead to similar life-threatening arrhythmias.3
Figure 1. Distortion of Normal Cardiac Myocyte Anatomy in Dilated Cardiomyopathy |
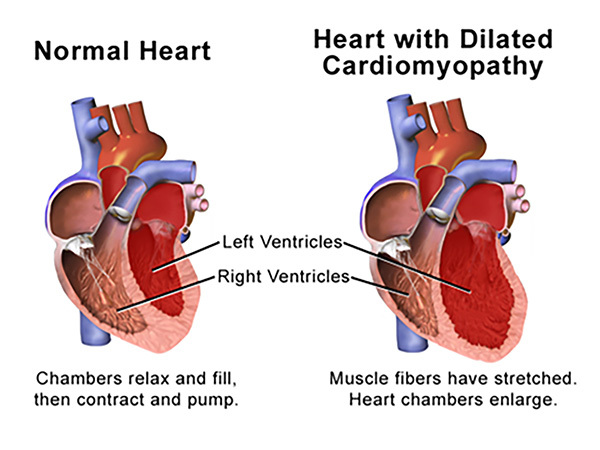 |
Source: Blausen.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). doi:10.15347/wjm/2014.010. ISSN 2002-4436. https://creativecommons.org/licenses/by/3.0/deed.en |
Hypertrophic cardiomyopathy (HCM) is the development of left ventricular hypertrophy associated with non-dilated ventricular chambers. (See Figure 2.) There is evidence for a strong genetic component leading to clustering in families. HCM has been estimated to increase risk of sudden cardiac death by approximately 1% each year.15
Figure 2. Left Ventricular Hypertrophy with Non-Dilated Ventricular Chambers in HCM |
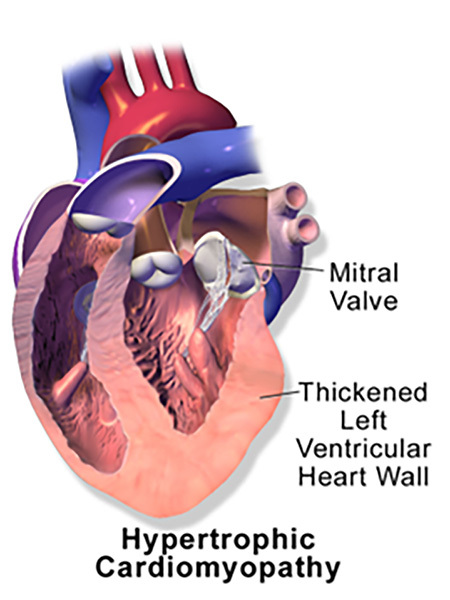 |
HCM: hypertrophic cardiomyopathy Source: Blausen.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). doi:10.15347/wjm/2014.010.ISSN 2002-4436. https://creativecommons.org/licenses/by/3.0/deed.en |
Arrhythmogenic right ventricular dysplasia (ARVD) is a rare hereditary form of cardiac muscle disease that is one of the more common causes of sudden cardiac death in athletes and young people. This disease results from a genetic mutation in desmosomal proteins leading to fibrofatty replacement of the myocardium.16 Patients with ARVD will subsequently develop right-sided heart failure causing arrhythmias of right ventricular origin.
The most common electrocardiogram (ECG) findings in ARVD are T wave inversion in the right precordial leads, V1-V3, and an epsilon wave seen in the ST segment(s) of V1 through V4. An epsilon wave (seen in Figure 3) is best described as a small deflection immediately following the QRS in the ST segment. This is a result of repolarization of the right ventricular myocytes. These ECG findings are either nonspecific (i.e., T wave inversions) or very subtle (i.e., epsilon wave); thus, it is difficult to detect and frequently not noted prior to sudden cardiac death. Patients diagnosed with ARVD usually will receive placement of an implantable cardioverter-defibrillator.17
Figure 3. Epsilon Wave of Arrhythmogenic Right Ventricular Dysplasia (ARVD) |
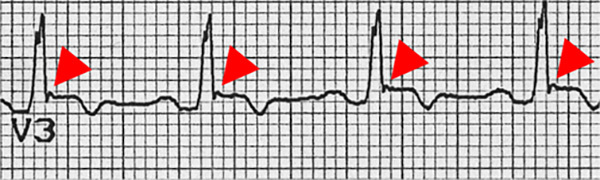 |
Source: https://commons.wikimedia.org/wiki/File:ARVD-Epsilon_wave.png; https://creativecommons.org/licenses/by-sa/3.0/deed.en |
Congenital Heart Disease
Advancements in healthcare screening and accessibility have improved life expectancy for children diagnosed with congenital heart disease (CHD). As a result, the population of adults with CHD has increased significantly. In the United States, it is estimated that approximately 40,000 infants per year will be affected with CHD, and 25% of those will require invasive treatment of CHD within the first year of life.4 For those children surviving to adulthood, the major complications from CHD include arrhythmias, infective endocarditis, and heart failure. Additionally, there is an increased risk of cardiac arrest in adults and children with obstructive left heart lesions, which include: transposition of the great arteries, Fontan circulations, repaired tetralogy of Fallot, aortic stenosis, and coarctation of the aorta.18 The risk of sudden cardiac death in adults with CHD, repaired or unrepaired, was estimated to be 24 times greater than in the general population.
Long QT Syndrome
Long QT syndrome is a genetic channelopathy leading to development of prolonged QT interval, usually defined as a QTc > 460 msec in women and > 440 msec in men. This genetic disorder leads to a predisposition to ventricular tachyarrhythmias when the QTc is > 500 msec and most commonly presents with syncopal episodes or cardiac arrest. Patients also can develop acquired prolonged QT syndrome secondary to medications or metabolic changes. In patients found to have a prolonged QT in an ED from 2010 to 2011, the prolongation was attributable to known QT-prolonging medical conditions in up to 56% of patients, electrolyte disturbances in up to 51%, and QT-prolonging medications in up to 77%.19
Clinical Features
As noted, cardiac arrest typically results from development of one of four cardiac rhythms: pulseless ventricular tachycardia, ventricular fibrillation, PEA, and asystole. These often are divided into shockable vs. non-shockable rhythms; ventricular fibrillation and pulseless ventricular tachycardia are considered shockable rhythms, while PEA and asystole are considered non-shockable rhythms.
Ventricular fibrillation is the result of disorganized electrical activity, which produces similarly disorganized mechanical activity and, thus, ineffective contraction of the ventricles. There is no evidence of P waves or discernible QRS complexes on the ECG. If ventricular fibrillation is identified, return of spontaneous circulation is most successful following prompt defibrillation. CPR, with high-quality chest compressions, should be initiated and continued while preparing for defibrillation. CPR should continue for two minutes following defibrillation until subsequent rhythm check. See Figure 4 for an example of ventricular fibrillation on a 12-lead electrocardiogram.
Figure 4. Ventricular Fibrillation Displayed on 12-Lead Electrocardiogram |
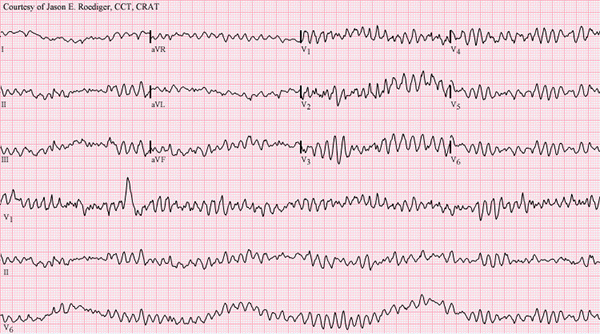 |
Source: https://commons.wikimedia.org/wiki/File:Ventricular_fibrillation.png; https://creativecommons.org/licenses/by-sa/3.0/deed.en |
Pulseless ventricular tachycardia is the result of ectopic ventricular foci, most commonly due to ischemic heart disease, acute MI, or hypoxia. Classically, the ECG will show a wide QRS with a regular rhythm at a rate of 150 to 200 beats per minute (bpm), frequently 170 to 180 bpm. See Figure 5 for an example of monomorphic ventricular tachycardia on electrocardiogram.
Figure 5. Electrocardiogram Showing Monomorphic Ventricular Tachycardia |
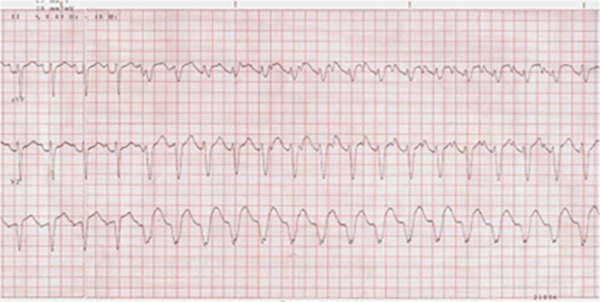 |
Source: CardioNetworks. https://commons.wikimedia.org/wiki/File:Vtach_%28CardioNetworks_ECGpedia%29.jpg; https://creativecommons.org/licenses/by-sa/3.0/deed.en |
There are variants of ventricular tachycardia, including bidirectional, alternating, polymorphic, and torsades de pointes. The initial management of pulseless ventricular tachycardia is the same as for ventricular fibrillation. The different variants of ventricular tachycardia are treated with the same algorithm as monomorphic ventricular tachycardia; torsades de pointes has a similar algorithm, with the noted addition of treatment of intravenous (IV) magnesium sulfate to prevent recurrence after restoration of sinus rhythm.
PEA describes the presence of identifiable electrical activity (other than ventricular tachycardia or ventricular fibrillation) visualized on a rhythm strip or cardiac monitor without a palpable pulse. Asystole is seen as a “flatline,” without evidence of any cardiac activity, organized rhythm, or palpable pulse; in fact, asystole is the absence of a cardiac rhythm or any activity. (See Figure 6.) Common etiologies for both include acute MI, severe acidosis, congestive heart failure (CHF), hypovolemia, obstructive shock, hypoglycemia, and hypoxia.19
Figure 6. Rhythm Strip Showing Asystole |
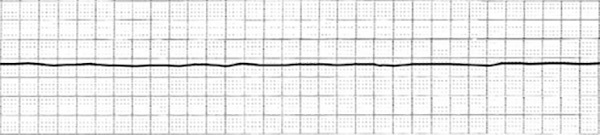 |
Source: https://commons.wikimedia.org/wiki/File:EKG_Asystole.jpg; https://creativecommons.org/licenses/by-sa/3.0/deed.en |
Initial management for both PEA and asystole should follow the American Heart Association (AHA) Advanced Cardiac Life Support (ACLS) guidelines, which include CPR with high-quality chest compressions. Chest compressions should continue for two uninterrupted minutes between assessments for presence of return of spontaneous circulation (ROSC) while epinephrine 1 mg IV or intraosseous (IO) is administered every three to five minutes, since early epinephrine is associated with higher rates of ROSC. Simultaneously, emergency medicine physicians should be considering the differential etiology of the arrest and identifying reversible causes that may be treated.20 (See Table 1.)
Table 1. The Hs and Ts Leading to Cardiac Arrest |
|
Hs |
Ts |
|
|
New Considerations for Management
The desired outcome from cardiac arrest resuscitation — “meaningful recovery” — is undergoing revision, specifically as it relates to neurological function. As the very definition of cardiac arrest involves lack of cerebral and systemic perfusion, cerebral injury and ischemia are the most common complications following cardiac arrest. Neurologic injury accounts for two-thirds of the deaths in patients following a cardiac arrest. Restoration of cardiac function without neurologic return is not a meaningful recovery. Ongoing research has identified several modifications in the standard management of cardiac arrest that may produce incremental improvement.
Head-Up CPR
Head-up CPR currently is undergoing evaluation as an alternative to traditional positioning during CPR. Instead of supine positioning, head-up CPR requires elevation of the head and thorax during compressions and resuscitation.21 Animal studies found improved hemodynamics during CPR and enhanced neurologic survival after resuscitation with head and thorax elevation compared to conventional supine CPR.22 Human studies suggest that head-up CPR is feasible for OHCA using a patient positioning device combined with automated chest compression and is associated with improved survival when applied within 18 minutes of the 911 call.23
The underlying physiologic theory is that elevation of the head/thorax will allow blood to drain more rapidly from the brain, allowing for increased venous return to the heart. This also would decrease intracranial pressure (ICP) and increase mean arterial pressure (MAP), subsequently leading to increased cerebral perfusion pressure (CPP). CPP is the difference between the arterial pressure driving blood into the brain and the venous backpressure. Typically, venous backpressure is a negligible contributor to elevated ICP during normal conditions; however, it often is significant during cardiac arrest.24 (See Figure 7.)
Figure 7. Theory for Physiologic Advantage of Head-Up CPR |
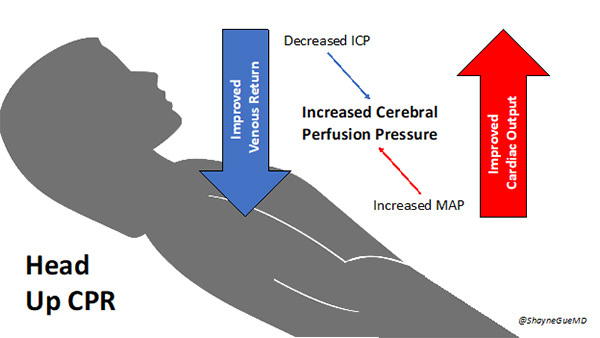 |
Created by Shayne Gue, MD, MSMEd |
Challenges are present with prolonged elevation of the head and thorax during CPR, particularly in attempting to generate enough force to overcome the gravitational gradient that occurs with upright positioning. Adjuncts, such as impedance threshold devices (ITD), were used in animal studies to address this concern.25 These porcine studies have evaluated changes in cerebral perfusion pressure, coronary perfusion pressure, and achievement of ROSC. The overall conclusion has been that those animals undergoing head-up CPR with ITD devices had higher rates of ROSC compared to traditional positioning.25,26
Evidence to support the use of head-up CPR in humans is limited to two larger scale human studies. The first evaluated the use of a mechanical compression device and ITD in OHCA and demonstrated doubling of resuscitation rates over the two years after implementation.27 A more recent study evaluated the impact of Automated Controlled Elevation CPR (ACE-CPR) with mechanical CPR devices and ITD on improved survival to hospital discharge compared with traditional CPR.23 Of those patients receiving ACE-CPR, 9.5% survived to discharge compared to 6.7% of patients in the conventional CPR group. Achievement of ROSC at any time was equal in each group, and favorable neurological outcome was 5.9% in the ACE-CPR group and 4.1% in the conventional CPR group.
The requirements for use of advanced equipment (mechanical CPR devices and ITD), as well as the significant education, training, and coordination that is required to use this equipment, makes this an expensive investment for most hospitals and healthcare delivery systems. Currently, there is no clinically relevant improvement in long-term outcomes, making it unlikely for healthcare stakeholders to implement the technique widely at this time. However, with continued technological advancements and increased research in this domain, head-up CPR may prove beneficial in the not-so-distant future.
Dual Sequential Defibrillation
As discussed earlier, defibrillation is a key component in the ACLS algorithm during cardiac arrest when shockable rhythms are identified, such as ventricular fibrillation or ventricular tachycardia.4 Refractory ventricular fibrillation typically is defined as ventricular fibrillation that does not convert with three or more single defibrillation attempts.28 It is estimated that 10% to 25% of cardiac arrest cases develop refractory or recurrent ventricular fibrillation. Although ventricular fibrillation and pulseless ventricular tachycardia have been associated with higher rates of survival and predictive of neurologically intact survival, the mortality for refractory ventricular fibrillation is estimated to be 97%.28
The most widely accepted theory is that refractory ventricular fibrillation results from the surge of catecholamines, which leads to continued myocardial instability. Dual sequential defibrillation (DSD) may improve conversion of refractory ventricular fibrillation based on several different concepts. One theory is that the first shock will lower the electrical threshold for myocardial depolarization, while the second shock will successfully depolarize and convert the patient.29 Another theory is that the change or increase in electrical vectors improves the likelihood for successful rhythm conversion. Anatomically, the left ventricle is further posterior in the mediastinum; therefore, having an anterior-posterior pad placement would change the vector of electricity while also adding another electrical vector to increase the likelihood of successful defibrillation. Lastly, the power theory of DSD is that the administration of more electrical joules during defibrillation allows for the conversion of all myocytes out of refractory ventricular fibrillation.30,31
Placement of pads for DSD involves placement of the first set of pads in the traditional location on the right anterior chest wall along the sternal border and at the cardiac apex. For placement of the second set of pads, there are two location options that have been described. The first is to have each pad immediately adjacent to the first set, without touching. The second option is to have an anteroposterior positioning where one is placed on the center of the patient’s back and one in the center of the anterior chest. It is important to note damage can occur to the defibrillator if the pads are touching. (See Figure 8 for pad placement options.)
Figure 8. Options for Additional Pad Placement in Dual Sequential Defibrillation |
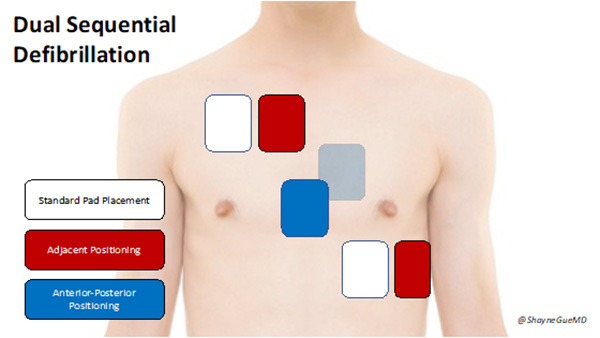 |
Created by Shayne Gue, MD, MSMEd |
The feasibility and safety of DSD was evaluated during the DOSE VF pilot trial in Ontario.32,33 This study involved four regional EMS services treating patients determined to be in refractory ventricular fibrillation during a nontraumatic OHCA. The study design was a three-arm, pilot, cluster randomization trial with crossover. The two interventions performed were DSD and vector change defibrillation, where pads were switched to the anterior-posterior position. Each EMS agency performed one technique for six months and then crossed over to one additional technique. Both were compared to standard care using ACLS protocols with the traditional anterior-lateral pad placement. ROSC was achieved in 25% of the standard care group, 39% in the vector change group, and 40% in the DSD group.
The follow-up prospective trial showed similar outcomes with improved survival to hospital discharge in the vector change and DSD groups, but only DSD was associated with an increased number of patients being discharged with good neurologic outcome compared to standard care.34 No instance of defibrillator damage was reported in this study.34
The majority of the remaining evidence for DSD is comprised of case studies and reports. In a meta-analysis of 39 cases, 77% of these patients had ventricular fibrillation successfully terminated with DSD, 54% achieved ROSC, and 28% of those achieving ROSC at admission had a Cerebral Performance Categories score of less than 2 at the time of hospital discharge.35-39
Additional defibrillation strategies have been described and trialed for refractory ventricular fibrillation. Vector change defibrillation as described earlier has been compared to the DSD strategy in a 2019 study.34 This style of defibrillation has been described most prominently in electrophysiology (EP) labs in the treatment for atrial fibrillation. In this 2019 study, the primary outcome was survival to hospital discharge. Patients were randomized to receive either standard defibrillation, vector change defibrillation or dual sequential external defibrillation. Results showed that DSD had a higher percentage of patients with good neurological outcomes. However, in patients who sustained refractory ventricular fibrillation, their survival to hospital discharge did occur more often in either the DSD or vector change group compared to the conventional defibrillation group.34
There have been some confounding variables discussed, since vector change and DSD have been used as a last resort in cardiac arrest with refractory ventricular fibrillation, particularly in instances of long resuscitation times or late application of the defibrillation strategy where meaningful recovery was unlikely.
There still are many limitations to the available evidence and ongoing research to distinguish true efficacy, but DSD may serve as an additional, low-resource tool for the treatment of cardiac arrest and refractory ventricular fibrillation. The 2020 American Heart Association ACLS Guidelines (currently in effect) state that the usefulness of DSD for refractory shockable rhythm has not been established and it is premature for this technique to be incorporated into routine clinical practice.40 If DSD is performed, the defibrillator should be taken out of service and checked for damage. Note that certain manufacturer warranties may be invalidated by DSD. It is strongly encouraged to check and be aware of the warranty for the device prior to considering this strategy.
Extracorporeal Membrane Oxygenation
Extracorporeal membrane oxygenation (ECMO) is one of the mechanical devices being used more and more frequently for organ and circulatory support during refractory cardiac arrest.41 An ECMO circuit consists of a blood pump, gas exchange device, conduit tubing that connects to arterial and venous vascular access, and a heat exchanger for temperature control. (See Figure 9.)
Figure 9. Example of an Extracorporeal Membrane Oxygenation Unit |
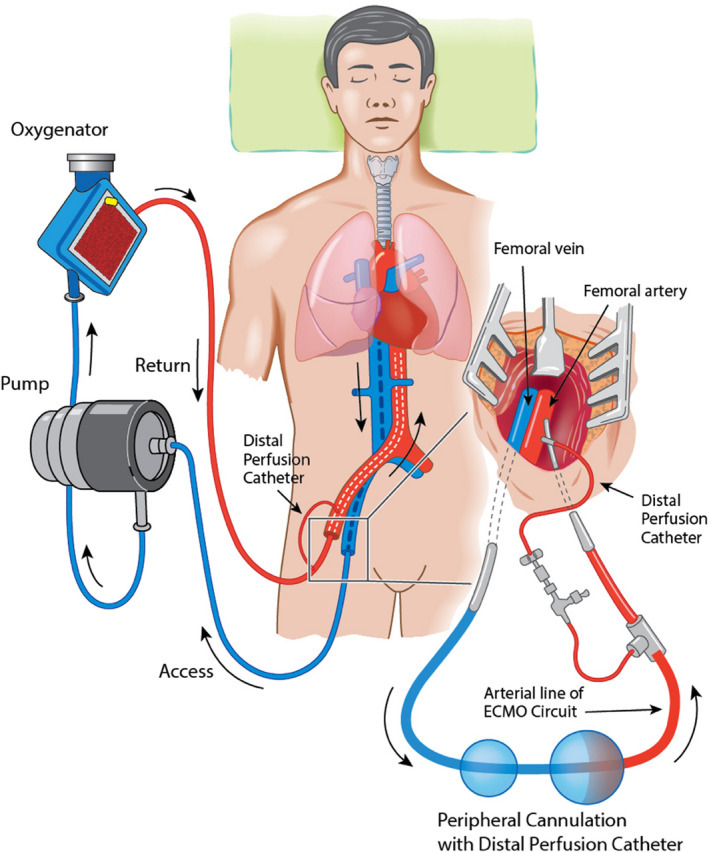 |
Source: Dennis M, Lal S, Forrest P, et al. In-depth extracorporeal cardiopulmonary resuscitation in adult out-of-hospital cardiac arrest. J Am Heart Assoc 2020;18;9:e016521. doi: 10.1161/JAHA.120.016521. Epub 2020 May 6. https://creativecommons.org/licenses/by/4.0/ |
The ECMO machine will withdraw blood from a venous cannula (often referred to as the drainage cannula), pump blood through an extracorporeal membrane lung, and return the newly oxygenated blood to the patient through the arterial cannula (or return cannula).42 There are several different variations and additional set-ups can be added for additional circulatory support. An example of one such variation is the addition of another venous cannula to help increase cardiac output or the addition of a return cannula to an upper body site in the setting of hypoxia.
The ARREST (advanced reperfusion strategies for patients with out-of-hospital cardiac arrest and refractory ventricular fibrillation) trial compared survival between 30 patients in refractory ventricular fibrillation who were treated with ECMO with immediate coronary angiography and catheterization compared to standard ACLS.43 This took place at a single center as an open-label, adaptive, safety and efficacy randomized clinical trial. This included patients with OHCA with refractory ventricular fibrillation without ROSC after three shocks, mechanical CPR with a LUCAS device, and transport time less than 30 minutes. The ECMO group went immediately to the catheterization lab (regardless of ROSC on hospital arrival), and ECMO cannulas were placed by a cardiologist, perfusion was started, and coronary angiography was completed. The standard ACLS group continued treatment in the ED following standard ACLS protocols. Resuscitation was discontinued based on arterial blood gas measurements of ETCO2 < 10 mmHg, PaO2 < 50 mmHg or O2 < 85%, or lactic acid > 18 mmol/L.
The primary outcome measure was survival to hospital discharge, with results indicating survival in 43% of patients in the ECMO group compared to 7% in the ACLS group. At six months, all survivors had good functional assessment scores with a modified Rankin Scale score of < 3. Because of significant survival differences and other benefits observed in the early ECMO group, the study was terminated early because the National Heart, Lung, and Blood Institute (NHLBI) deemed it unethical to continue to expose patients to ACLS treatment in the presence of a mature ECMO program.
The INCEPTION (Early Initiation of Extracorporeal Life Support in Refractory OHCA) trial was conducted as a multicenter, randomized controlled trial in the Netherlands.44 Published in 2023, the trial assessed ECMO CPR compared to conventional CPR with the primary outcome measure being survival with a favorable neurological outcome. At 30 days, survival with a Cerebral Performance Categories score of 1 or 2 was reported in 20% of patients in the ECMO CPR group compared to 16% of patients in the conventional CPR group. Survival with a favorable outcome was similar in both groups at six months. This more recent study challenges the conclusions of the ARREST trial, indicating no statistically significant difference between groups.
In the INCEPTION trial, the median interval between patient arrival and initiation of cannulation was 16 minutes, and the interval between start of cannulation and start of ECMO was 20 minutes, both longer than the intervals in the ARREST trial, with a mean time from arrival to ECMO initiation of seven minutes.43,44 The authors of the INCEPTION trial attributed these longer intervals to the ARREST study being completed at a center with higher caseloads, contributing to a more experienced team and improved logistics. An additional limitation observed during the INCEPTION trial was the lack of EMS-specific protocols for OHCA during the trial, but the authors noted that EMS teams were aware of the trial, which may have prompted them to proceed to intra-arrest transport earlier than usual. There also was no standardized trial protocol for ECMO; therefore, each site relied on previously established routines, but no center-specific effect was observed.
ECMO achieves three main goals in patients with refractory cardiac arrest. It will normalize perfusion reliably, provide cardiopulmonary support, and can aid in the identification and serve as a bridge to invasive management of CAD (with angiography and potential percutaneous coronary intervention), the most common cause of refractory ventricular fibrillation. It also has the potential to serve as a bridge for patients in the intensive care unit (ICU) when multi-organ injury is incurred because of prolonged resuscitation.45
ECMO is underused in most community EDs because of the high resource need and requirement for experienced interventional cardiac care teams. ECMO is labor- and resource-intensive, requiring specialized equipment and significant coordination for optimal patient outcomes, limitations observed in the INCEPTION trial. In contrast, the ARREST trial highlighted the importance of well-orchestrated collaboration and coordination of care for the well-being of patients within a community. Further, some systematic reviews and meta-analyses have suggested that patients treated with ECMO from an OHCA, found in a shockable rhythm, demonstrated twice the odds of survival with favorable neurological outcome compared to non-shockable rhythms.42,46,47
In the available studies comparing ECMO in refractory cardiac arrest, shorter time to ECMO initiation has shown more favorable outcomes, usually within 60 minutes of pulselessness. There still are limitations in the available evidence and no consensus for practice recommendations regarding optimal timing for initiation of ECMO CPR. It also must be pointed out that a portion of the literature is based on studies performed in western Europe, where physicians regularly staff EMS units and initiate cannulation and/or ECMO prior to ED arrival. Such a model is not feasible in the United States at the present time.
In patients presenting in cardiac arrest with refractory ventricular fibrillation, an estimated 70% to 85% will have CAD, which, combined with poor perfusion during CPR, decreases the chance of ROSC and meaningful recovery. ECMO may serve as a bridge to maintain systemic and cardiac perfusion during cardiac arrest while investigations into the primary cause are explored and treated.42,48 ECMO also is an expensive tool, with complex requirements for training, collaboration, and care coordination not available at the majority of community centers. ECMO CPR remains a topic of active investigation.
Targeted Temperature Management
Targeted temperature management (TTM), previously referred to as therapeutic hypothermia, in cardiac arrest has been a routine part of post-ROSC care in EDs and ICUs around the globe, with evidence of this practice dating back to 2002.49 TTM refers to the therapeutic lowering of a patient’s core temperature below 36°C. The physiologic theory was that lowering a patient’s core body temperature would ultimately slow biological processes and inflammatory changes leading to organ damage. In 2002, there were two major prospective, randomized controlled trials published that found notable differences in short- and long-term survival in cardiac arrest patients and improvements in their neurological outcomes; these studies set the basis for today’s TTM.50,51
The pathophysiologic theories behind recommendations for TTM are based on the goals of decreasing metabolic changes and cellular damage that can occur systemically after prolonged hypoperfusion and ischemia. In a patient experiencing cardiac arrest and resultant hypoperfusion, cells shift to anaerobic metabolism, leading to the creation and accumulation of lactic acid, free radicals, and other toxic byproducts. Specific to the brain, the accumulation of these anaerobic metabolism waste products can accelerate cerebral cell death. Hypothermia may decrease the metabolic rate by about 5% to 7% for every 1°C decrease in core temperature.52 Reperfusion injury is another feared complication in patients who achieve ROSC following prolonged cardiac arrest. With reperfusion, there is a massive increase in the formation of free radicals, which are known to target neurons and contribute to neuronal and inflammatory damage.
The induced hypothermia trial in 2002 was the initial evidence used for recommendations of TTM. Hypothermia was initiated by prehospital EMS personnel, continued in the hospital to a core temperature of 33°C, and maintained for 12 hours, followed by active external rewarming.50 The only patients included were those presenting with an initial rhythm of ventricular fibrillation. The primary outcome was survival to hospital discharge with “sufficiently good neurologic function.” Initial data were favorable, setting the standard for TTM; however, further reviews indicated major limitations, since only patients with ventricular fibrillation were included and those with a poor prognosis were excluded.
The Targeted Temperature Management (TTM) trial in 2013 was the first trial to have its results challenge the established protocol for post-ROSC therapeutic hypothermia.53 This trial compared patients with TTM to 33°C and 36°C. Temperatures were maintained for 28 hours and then patients were rewarmed to 37°C, followed by maintenance of temperatures below 37.5°C for 72 hours. There were no significant benefits identified between the two groups.53
The TTM2 trial, published in 2021, compared outcomes in patients with induced hypothermia at 33°C to targeted normothermia at 37.5°C.54 Temperatures were maintained for 28 hours following ROSC, and then patients were rewarmed to 37°C over the following 72 hours. The study concluded that therapeutic hypothermia did not lead to lower mortality compared to normothermia. There was no definitive improvement in neurological outcomes of these patients based on the modified Rankin Scale. A major complication was the increased incidence of arrhythmia in the hypothermia group compared to normothermia, further supporting existing literature that moderate hypothermia can be pro-arrhythmic.52,54
The CAPITAL CHILL trial evaluated whether targeted hypothermia at even lower temperatures would lead to more profound outcomes.55 Patients were randomized to groups with TTM at 31°C and 34°C for 24 hours and then rewarmed to 37°C. Ultimately, there was no difference in neurological outcomes, mortality, and adverse events between the two groups.55
Despite the results of these more recent studies, current guidelines continue to recommend TTM for all patients experiencing both OHCA and IHCA who achieve ROSC. The European Resuscitation Council (ERC) and European Society of Intensive Care Medicine (ESICM) recommend a target temperature between 32°C and 36°C for 24 hours following ROSC and avoiding fever, temperature > 37.7°C for 72 hours after ROSC.56 The 2020 AHA guidelines recommend TTM between 32°C and 36°C for at least 24 hours for all cardiac rhythms in OHCA and IHCA.40
Cooling is done through external measures or intervascular devices. Currently, both guidelines do not recommend routine rapid infusion of chilled IV fluids in the prehospital setting. Regarding the association of hyperthermia and poor neurological outcomes in post-cardiac arrest patients, there have been no randomized controlled studies yet to examine controlling fever in these patients. Most guidelines suggest prevention of fever and maintenance of temperature below 37.5°C in patients who have achieved ROSC following cardiac arrest.57
The basis of recommendations for therapeutic hypothermia in cardiac arrest patients originated more than 20 years ago in often underpowered studies. Numerous more recent studies have not demonstrated any benefit of therapeutic hypothermia compared to normothermia.58
Conclusion
After more than 50 years of study, incremental improvements have been made in survivability and neurologic outcome in OHCA. Bystander CPR, publicly available automated defibrillators, rapid emergency medical service response, and specialized post-arrest facilities all have produced benefits. One potential advance discussed in this article — DSD — likely is applicable to a limited group of patients: those with refractory ventricular fibrillation. Further improvements applicable to a wider range of patients will require a major investment in equipment and training.
Disclaimer: This research was supported (in whole or in part) by HCA Healthcare and/or an HCA Healthcare affiliated entity. The views expressed in this publication represent those of the author(s) and do not necessarily represent the official views of HCA Healthcare or any of its affiliated entities.
REFERENCES
- Albert C, Sauer WH. Cardiovascular collapse, cardiac arrest, and sudden cardiac death. In: Loscalzo J, Fauci A, Kasper D, et al, eds. Harrison’s Principles of Internal Medicine, 21e. McGraw Hill; 2022.
- Wyckoff MH, Singletary EM, Soar J, et al. 2021 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations: Summary from the Basic Life Support; Advanced Life Support; Neonatal Life Support; Education, Implementation, and Teams; First Aid Task Forces; and the COVID-19 Working Group. Resuscitation 2021;169:229-311.
- Ornato JP. Sudden cardiac death. In: Tintinalli JE, Ma O, Yealy DM, et al, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 9e. McGraw Hill; 2020.
- Tsao CW, Aday AW, Almarzooq ZI, et al. Heart Disease and Stroke Statistics-2022 Update: A Report from the American Heart Association [published correction appears in Circulation 2022;146:e141]. Circulation 2022;145:e153-e639.
- Lim ZJ, Ponnapa Reddy M, Afroz A, et al. Incidence and outcome of out-of-hospital cardiac arrests in the COVID-19 era: A systematic review and meta-analysis. Resuscitation 2020;157:248-258.
- Chugh SS, Reinier K, Teodorescu C, et al. Epidemiology of sudden cardiac death: Clinical and research implications. Prog Cardiovasc Dis 2008;51:213-228.
- Benjamin EJ, Muntner P, Alonso A, et al. Heart Disease and Stroke Statistics-2019 Update: A Report from the American Heart Association [published correction appears in Circulation 2020;141:e33]. Circulation 2019;139:e56-e528.
- Cardiac Arrest Registry to Enhance Survival. 2020 Annual Report. https://mycares.net/sitepages/uploads/2021/2020_flipbook/index.html?page=1
- Kurz MC, Donnelly JP, Wang HE. Variations in survival after cardiac arrest among academic medical center-affiliated hospitals. PLoS One 2017;12:e0178793.
- Bougouin W, Mustafic H, Marijon E, et al. Gender and survival after sudden cardiac arrest: A systematic review and meta-analysis. Resuscitation 2015;94:55-60.
- Wright JD, Folsom AR, Coresh J, et al. The ARIC (Atherosclerosis Risk In Communities) Study: JACC Focus Seminar 3/8. J Am Coll Cardiol 2021;77:2939-2959.
- Pouleur AC, Barkoudah E, Uno H, et al. Pathogenesis of sudden unexpected death in a clinical trial of patients with myocardial infarction and left ventricular dysfunction, heart failure, or both. Circulation 2010;122:597-602.
- Tseng ZH, Olgin JE, Vittinghoff E, et al. Prospective countywide surveillance and autopsy characterization of sudden cardiac death: POST SCD Study. Circulation 2018;137:2689-2700.
- Faxén J, Jernberg T, Hollenberg J, et al. Incidence and predictors of out-of-hospital cardiac arrest within 90 days after myocardial infarction. J Am Coll Cardiol 2020;76:2926-2936.
- Frenneaux MP. Assessing the risk of sudden cardiac death in a patient with hypertrophic cardiomyopathy. Heart 2004;90:570-575.
- Basso C, Corrado D, Marcus FI, et al. Arrhythmogenic right ventricular cardiomyopathy. Lancet 2009;373:1289-1300.
- Azaouagh A, Churzidse S, Konorza T, Erbel R. Arrhythmogenic right ventricular cardiomyopathy/dysplasia: A review and update. Clin Res Cardiol 2011;100:383-394.
- Moore B, Yu C, Kotchetkova I, et al. Incidence and clinical characteristics of sudden cardiac death in adult congenital heart disease. Int J Cardiol 2018;254:101-106.
- Anderson HN, Bos JM, Haugaa KH, et al. Prevalence and outcome of high-risk QT prolongation recorded in the emergency department from an institution-wide QT alert system. J Emerg Med 2018;54:8-15.
- Durila M. Reversible causes of cardiac arrest 4 “Ts” and 4 “Hs” can be easily diagnosed and remembered following general ABC rule, Motol University Hospital approach. Resuscitation 2018;126:e7.
- Rezaie S. In the pipeline: Head up CPR in OHCA? REBEL EM blog. May 1, 2021. https://rebelem.com/in-the-pipeline-head-up-cpr-in-ohca/
- Moore JC. Head-up cardiopulmonary resuscitation. Curr Opin Crit Care 2023;29:155.
- Moore JC, Pepe PE, Scheppke KA, et al. Head and thorax elevation during cardiopulmonary resuscitation using circulatory adjuncts is associated with improved survival. Resuscitation 2022;179:9-17.
- Powers WJ. Cerebral blood flow and metabolism: Regulation and pathophysiology in cerebrovascular disease. In: Mendelow AD, Sacco RL, Wong LKS, et al. Stroke. 6e. Elsevier; 2016.
- Rojas-Salvador C, Moore JC, Salverda B, et al. Effect of controlled sequential elevation timing of the head and thorax during cardiopulmonary resuscitation on cerebral perfusion pressures in a porcine model of cardiac arrest. Resuscitation 2020;149:162-169.
- Ryu HH, Moore JC, Yannopoulos D, et al. The effect of head up cardiopulmonary resuscitation on cerebral and systemic hemodynamics. Resuscitation 2016;102:29-34.
- Pepe PE, Scheppke KA, Antevy PM, et al. Confirming the clinical safety and feasibility of a bundled methodology to improve cardiopulmonary resuscitation involving a head-up/torso-up chest compression technique. Crit Care Med 2019;47:449-455.
- Sarkozy A, Dorian P. Strategies for reversing shock-resistant ventricular fibrillation. Curr Opin Crit Care 2003;9:189-193.
- Miraglia D, Miguel LA, Alonso W, Ayala JE. Double sequential defibrillation for out-of-hospital refractory ventricular fibrillation: A scoping review. Am J Emerg Med 2020;38:1211-1217.
- El Tawil C, Mrad S, Khishfe BF. Double sequential defibrillation for refractory ventricular fibrillation. Am J Emerg Med 2017;35:1985.e3-1985.e4.
- Ramzy M, Hughes PG. Double defibrillation. In: StatPearls. StatPearls Publishing; Updated April 7, 2023.
- Cheskes S, Dorian P, Feldman M, et al. Double sequential external defibrillation for refractory ventricular fibrillation: The DOSE VF pilot randomized controlled trial. Resuscitation 2020;150:178-184.
- Morgenstern J. Double sequential defibrillation (The DOSE VF trial). First10EM. Published March 2, 2020. https://doi.org/10.51684/FIRS.12331
- Cheskes S, Verbeek PR, Drennan IR, et al. Defibrillation strategies for refractory ventricular fibrillation. N Engl J Med 2022;387:1947-1956.
- Sena RC, Eldrich S, Pescatore RM, et al. Refractory ventricular fibrillation successfully cardioverted with dual sequential defibrillation. J Emerg Med 2016;51:e37-e40.
- Bell CR, Szulewski A, Brooks SC. Make it two: A case report of dual sequential external defibrillation. CJEM 2018;20:792-797.
- Boehm KM, Keyes DC, Mader LE, Moccia JM. First report of survival in refractory ventricular fibrillation after dual-axis defibrillation and esmolol administration. West J Emerg Med 2016;17:762-765.
- Leacock BW. Double simultaneous defibrillators for refractory ventricular fibrillation. J Emerg Med 2014;46:472-474.
- Hajjar K, Berbari I, El Tawil C, et al. Dual defibrillation in patients with refractory ventricular fibrillation. Am J Emerg Med 2018;36:1474-1479.
- Panchal AR, Bartos JA, Cabañas JG, et al. Part 3: Adult Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2020;142(16_suppl_2):S366-S468.
- Klee TE, Kern KB. A review of ECMO for cardiac arrest. Resusc Plus 2021;5:100083.
- Dennis M, Lal S, Forrest P, et al. In-depth extracorporeal cardiopulmonary resuscitation in adult out-of-hospital cardiac arrest. J Am Heart Assoc 2020;9:e016521.
- Yannopoulos D, Bartos J, Raveendran G, et al. Advanced reperfusion strategies for patients with out-of-hospital cardiac arrest and refractory ventricular fibrillation (ARREST): A phase 2, single centre, open-label, randomised controlled trial. Lancet 2020;396:1807-1816.
- Suverein MM, Delnoij TSR, Lorusso R, et al. Early extracorporeal CPR for refractory out-of-hospital cardiac arrest. N Engl J Med 2023;388:299-309.
- Astin M, The ARREST Trial: ECMO or EC-No for refractory cardiac arrest? REBEL EM blog. March 4, 2021. https://rebelem.com/the-arrest-trial-ecmo-or-ec-no-for-refractory-cardiac-arrest/
- Scquizzato T, Bonaccorso A, Swol J, et al. Refractory out-of-hospital cardiac arrest and extracorporeal cardiopulmonary resuscitation: A meta-analysis of randomized trials. Artif Organs 2023;47:806.
- Kiyohara Y, Kampaktis PN, Briasoulis A, Kuno T. Extracorporeal membrane oxygen-facilitated resuscitation in out-of-hospital cardiac arrest: A meta-analysis of randomized controlled trials. J Cardiovasc Med 2023;24:414.
- De Charrière A, Assouline B, Scheen M, et al. ECMO in cardiac arrest: A narrative review of the literature. J Clin Med 2021;10:534.
- Omairi AM, Pandey S. Targeted temperature management. In: StatPearls: StatPearls Publishing; Aug. 28, 2022.
- Bernard SA, Gray TW, Buist MD, et al. Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. N Engl J Med 2002;346:557-563.
- Hypothermia After Cardiac Arrest Study Group. Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N Engl J Med 2002;346:549-555.
- Schubert A. Side effects of mild hypothermia. J Neurosurg Anesthesiol 1995;7:139-147.
- Nielsen N, Wetterslev J, Cronberg T, et al. Targeted temperature management at 33°C versus 36°C after cardiac arrest. N Engl J Med 2013;369:2197-2206.
- Dietrichs ES, McGlynn K, Allan A, et al. Moderate but not severe hypothermia causes pro-arrhythmic changes in cardiac electrophysiology [published correction appears in Cardiovasc Res 2020;116:1322]. Cardiovasc Res 2020;116:2081-2090.
- Le May M, Osborne C, Russo J, et al. Effect of moderate vs mild therapeutic hypothermia on mortality and neurologic outcomes in comatose survivors of out-of-hospital cardiac arrest: The CAPITAL CHILL Randomized Clinical Trial. JAMA 2021;326:1494-1503.
- Nolan JP, Sandroni C, Böttiger BW, et al. European Resuscitation Council and European Society of Intensive Care Medicine guidelines 2021: Post-resuscitation care. Intensive Care Med 2021;47:369-421.
- Helman A, Morgenstern J, Morrison M. Journal Jam 19 – Therapeutic Hypothermia After Cardiac Arrest – Mixed Evidence. Emergency Medicine Cases. Oct. 5, 2021. https://emergencymedicinecases.com/journal-jam-therapeutic-hypothermia-cardiac-arrest
- Lüsebrink E, Binzenhöfer L, Kellnar A, et al. Targeted temperature management in postresuscitation care after incorporating results of the TTM2 trial. J Am Heart Assoc 2022;11:e026539.
Cardiac arrest requires emergent medical intervention, with the goal of perfusing the brain and other major organs while attempting to reverse the underlying etiology causing the arrest.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
