Patients embrace use of kiosks for check-in
 |
Patients embrace use of kiosks for check-in
Payment option is next step
By Gail Mitchell, Director of Regional Access Services, Providence Health System, Portland, OR
(Editor's note: In this second segment of a two-part series, Gail Mitchell describes two access initiatives designed to simplify the registration process: check-in kiosks and centralized pre-registration. The first segment, by Rebecca Coplin, dealt with the infrastructure the organization has in place to ensure process improvement, including Six Sigma training and the creation of the Seamless Access department. It ran in the February 2006 issue of Hospital Access Management.)
In implementing self-service kiosks, the first of two Providence Health System initiatives aimed at improving revenue cycle and patient satisfaction scores, our goal was to reduce wait time in our outpatient areas by providing the option of self check-in.
The project team decided to pilot a kiosk with pre-registered patients receiving mammograms. Providence then started a relationship with the vendor Galvanon (now NCR) to build our model kiosk and determine how it would function and present to our patients.
The result is a custom, sleekly styled product that interfaces with our host health information system, presents aesthetically as state-of-art technology in our clinical areas, and provides a final product to our patients that is tailored to meet their needs and our goal of streamlined patient processing.
Use of the kiosk has a qualifier: The patient must be pre-registered prior to the date of service. Patients are informed about their ability to use the kiosk to check in at the time of pre-registration. To date, between 60% and 70% of patients who qualify actually use it on the day of service.
Patients who have been informed about the process can approach the freestanding chrome kiosk and either swipe a card with any magnetic identifier or type their name using the onscreen keyboard — much like an airport kiosk check-in application.
The kiosk prompts for date of birth verification and walks patients through a small number of screens, depending on their distinct registration needs.
The nine-page HIPAA form can be printed or is available from a rack on the side of the kiosk. Patients indicate that they have reviewed the form by using a stylus to sign onscreen, and may print a copy of the acknowledgment.
The conditions of service form also can be signed with the stylus. Both acknowledgements then feed automatically to the electronic medical record.
An access services representative, located nearby at her desk, can view what the patient at the kiosk is doing from her screen. She can see if the check-in is complete or if there are questions or problems. If at any point during kiosk check-in the patient is not able to complete all the steps, it instructs the person to step to the registration desk to complete check-in. If the check-in is completed as expected, the kiosk sends a message to the host information system that generates an order into that system so clinical staff know the patient has arrived and has checked in.
On the first days after the "go live" date, greeters were deployed to the kiosks to encourage usage and help patients through their first time. Little help was needed. Patients have embraced this technology easily. Coupons for the coffee carts were given to thank patients for trying it out.
The kiosks have received very favorable comments from patients, who say they want to use it for other services, not just the designated diagnostic imaging services now offered. Kiosks are in operation at three Providence Portland-based facilities for mammogram patients.
Next steps include the ability to take patient payments at the kiosk and to print maps from any location in the hospital for way finding. Plans for the next one to two years also include statewide rollout for all scheduled services.
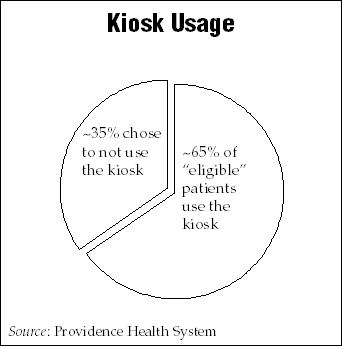 |
Central access services
Another tool created to improve patient satisfaction and the revenue cycle is the Central Access Services (CAS) department. This department, comprised of 70 employees, was created to support pre-registration and verification of benefits for services for all facilities in the state.
Staff in CAS function as members of one of four teams: customer service/pre-registration, verification, maternity, or special teams. The special teams group handles verification for all same-day admissions, either directly or from the emergency department, and re-verification for patient type changes or extended lengths of stay.
Notification of these changes to CAS is accomplished through system-generated reports that print directly to CAS and the ability to queue accounts directly to CAS worklists by entering system notes.
This department has been able to succeed with innovative software programs that queue up patients from the scheduling systems and present them in an automated, pre-designated worklist sort format. This ensures that no accounts are missed and that all accounts present to the customer service team as soon after scheduling as possible.
CAS has a goal of pre-registering and verifying 97% of all scheduled services prior to date of service. In 2005, this team surpassed its goal, with 98% completions.
The high completion rates are largely attributable to the fact that these employees are dedicated to this task only. When these duties are assigned to staff on site in facilities, many times employees are pulled away to cover for absent team members who staff a front desk for walk-in patients. In that scenario, patient pre-registration opportunities may be lost.
The additional goal of being two weeks out on pre-registration and verification is always a challenge but is most commonly the reality now that this team has matured. The 2% failure rate is related to patient unwillingness to call back or to pre-register over the phone.
The teams in CAS also can queue up printing of facesheets at any designated location either by a predetermined batch mode at designated times or on demand when required with updates noted. These teams also have access to real-time eligibility and batch eligibility exception reports on an ongoing and nightly basis to ensure clarity in account sponsorship.
[Editor's note: Gail Mitchell can be reached at (503) 215-7394 or by e-mail at [email protected].]
In implementing self-service kiosks, the first of two Providence Health System initiatives aimed at improving revenue cycle and patient satisfaction scores, ...Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
