ECG Review: Nothing More than Nonspecific Changes?
ECG Review
Nothing More than Nonspecific Changes?
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
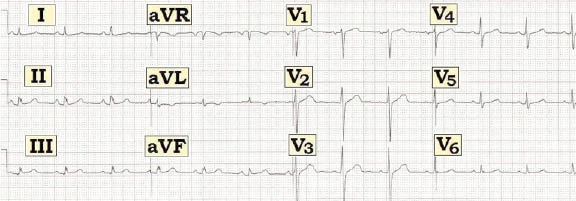
Scenario: The ECG shown above was interpreted as essentially "normal," showing nothing more than minimal nonspecific ST-T wave changes. Do you agree?
Interpretation: The rhythm is sinus at a rate just under 75/minute. All intervals and the mean QRS axis are normal. There is low voltage in the limb leads (ie, QRS amplitude does not exceed 5 mm in I, II, III, aVR, aVL, or aVF). There is no chamber enlargement. Regarding Q-R-S-T changes there may be a tiny q wave in lead III. R wave progression is normal, with transition being slightly delayed to between leads V3-to-V5.
The interesting findings relate to the inferior leads. There is subtle but real ST segment elevation in leads II, III and aVF. ST segment deviations are judged with respect to the preceding PR segment baseline and the takeoff of the J-point in each of the inferior leads is above this baseline. Support that this finding is real comes from the subtle ST segment coving and shallow, symmetric T- wave inversion in lead aVL.
Given the small amplitude and admittedly subtle nature of the above findings we are not at all certain that they represent acute inferior infarction. However, this possibility should be considered. Clinical correlation and comparison with prior tracings is needed to clarify the situation. If this patient had presented with new-onset chest pain and no prior tracings serial troponins and repeat ECG would be needed to rule out an acute event. Even without a history of new-onset chest pain, this tracing should not be interpreted as "normal." Clinical correlation is essential before determining disposition of the patient.
The ECG shown above was interpreted as essentially "normal," showing nothing more than minimal nonspecific ST-T wave changes. Do you agree?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
