Lyme Disease in the United States — Good News, Bad News
By Stan Deresinski, MD, FACP, FIDSA
Clinical Professor of Medicine, Stanford University
Dr. Deresinski reports no financial relationships relevant to this field of study.
SYNOPSIS: The incidence of Lyme disease appears to have stabilized in states with known high incidences of the infection, but there is evidence of geographic expansion into neighboring states.
SOURCE: Schwartz AM, Hinckley AF, Mead PS, et al. Surveillance for Lyme disease — United States, 2008–2015. MMWR Surveill Summ 2017;66:1–12.
The CDC received 275,589 reports of Lyme disease from 2008-2015. Of these, 208,344 were confirmed and 66,755 were probable. An average of 8,344 probable cases were reported annually.
Fourteen Northeast, mid-Atlantic, and upper Midwest states (Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin) accounted for 95.2% of all reports. (See Figures 1 and 2.) Three-fourths of cases reported from these states were confirmed. There was no significant change in the median annual percentage change in the number of reported cases in these states over the period examined and, in fact, there was a decreasing trend in seven of the 14 states. (See Figure 1.) In contrast, in 11 states and the District of Columbia that neighbor the 14 high-incidence states, the overall median annual change in confirmed cases was 6.6% (range, -16.7% to 31.3%), with an increasing trend in eight of the 11 states. Thus, there is evidence of geographic expansion of the disease.
Peaks in incidence by age occurred bimodally, at 5-9 years and at 50-55 years. Erythema migrans was reported in 72.2% of patients, while 27.5% had arthritis and 1.5% had carditis. A neurological manifestation was reported in 12.5% of patients, with facial palsy in 8.4%, radiculoneuropathy in 3.8%, and meningitis in 1.3%. Less than 1.0% had encephalitis. The proportion of patients with erythema migrans was lower in low-incidence states (64.7%) than in high-incidence states (72.3%), while the reverse was true for neurological manifestations (20.0% and 12.2%, respectively).
COMMENTARY
With more than 30,000 cases each year, Lyme disease is the most frequently reported vector-borne disease in the United States. The apparent stabilization of the reported incidence of Lyme disease from 2008-2015 could be real or could be the result of changing case definitions over the period examined. Of note is that the definition has been changed again in 2017, with the hope of increasing specificity. At the same time that the incidence of infections apparently has stabilized in high-incidence states, there is evidence that it is increasing in neighboring states, a finding consistent with evidence of an increase in the range of established populations of Ixodes scapularis, the vector of Borrelia burgdorferi. In the upper Midwest, Borrelia mayonii also causes Lyme disease and is transmitted by the same tick species. In the western Pacific region, the vector is Ixodes pacificus.
The clinical differences noted in cases in high- and low-incidence states may be due to the increase in false positives when tests are applied to low-prevalence populations. In addition, skin manifestations resembling erythema migrans may occur in states, including some with low incidences of Lyme disease, in which southern tick-associated rash illness is seen.
The apparent stabilization of cases in high-incidence states is encouraging. However, the geographical expansion into neighboring states can only engender concern.
Figure 1. Number* of Confirmed and Probable Lyme Disease Cases, by State Surveillance Category† and Year — United States, 1992-2015§
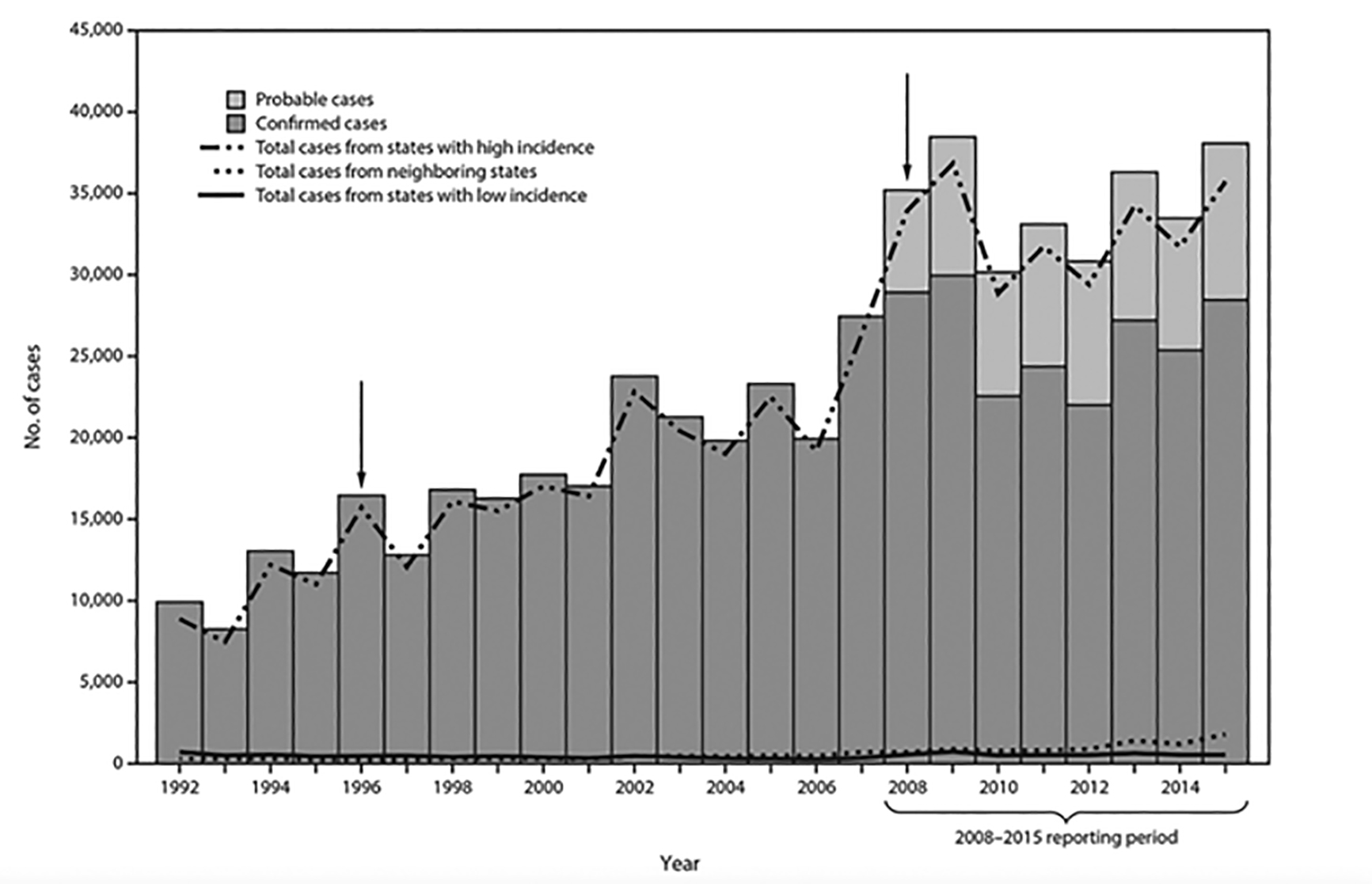
*N = 551,107
† State surveillance categories were determined using three classifications: high incidence, neighboring, and low incidence. States with an average annual incidence ≥10 confirmed Lyme disease cases per 100,000 population were classified as high incidence, states that share a border with those states or are located between states with high incidence were classified as neighboring, and all other states were classified as low incidence.
§ Arrows indicate notable changes in case definitions. The case definition was revised in 1996 to recommend a two-step testing method and in 2008 to increase specificity of laboratory evidence of infection and to include provision for report of probable cases.
Source: Centers for Disease Control and Prevention
Figure 2. Average Annual Number of Confirmed Lyme Disease Cases, by County of Residence* — United States, 2008-2015†
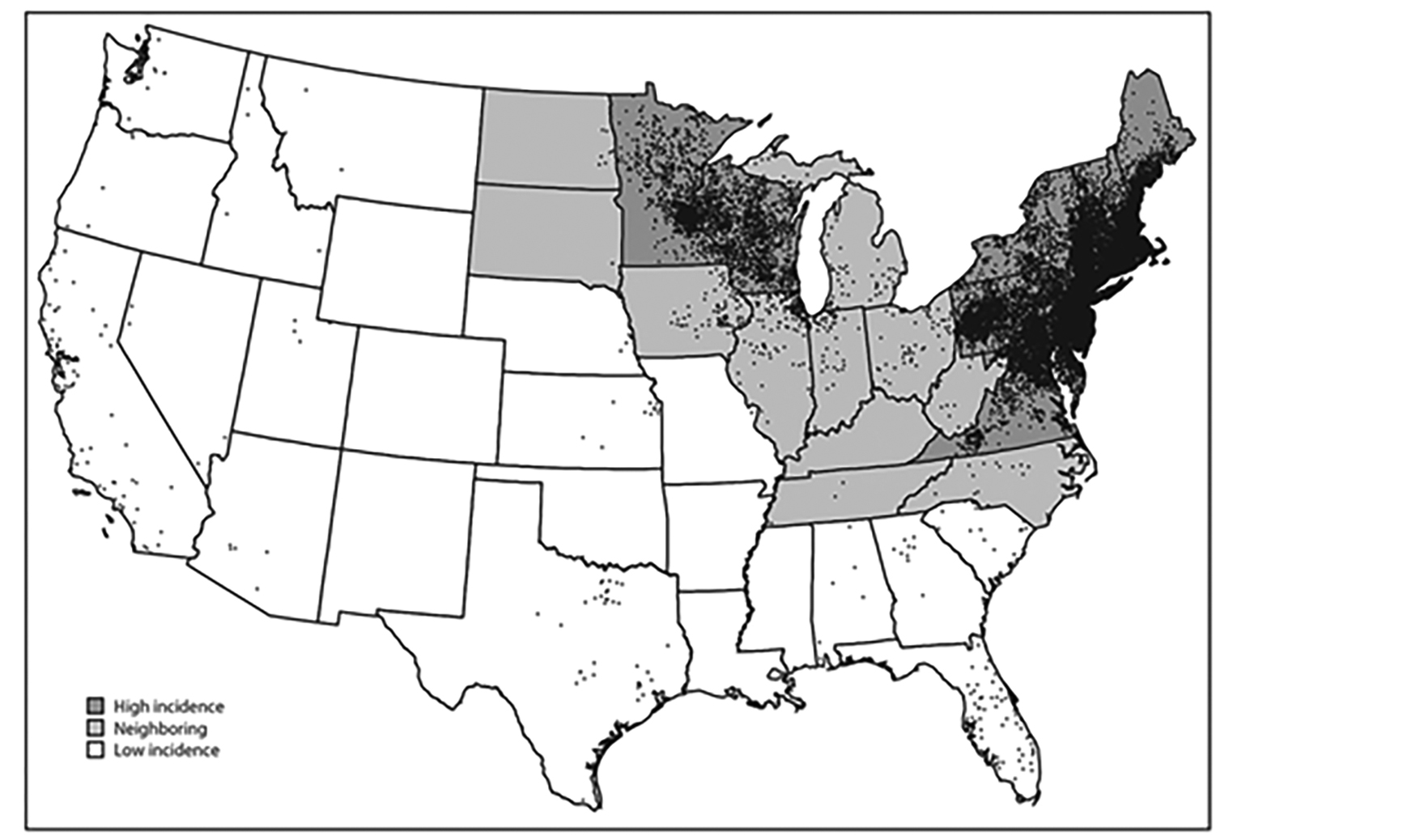
* Each dot represents one confirmed case according to the patient’s county of residence.
† State surveillance categories were determined using three classifications: high incidence, neighboring, and low incidence. States with an average annual incidence ≥ 10 confirmed Lyme disease cases per 100,000 population were classified as high incidence, states that share a border with those states or are located between states with high incidence were classified as neighboring, and all other states were classified as low incidence.
Source: Centers for Disease Control and Prevention
The incidence of Lyme disease appears to have stabilized in states with known high incidences of the infection, but there is evidence of geographic expansion into neighboring states.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
