Can You Interpret This Rhythm?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The long lead II rhythm strip in the figure below was obtained from a middle-aged woman with syncope and hypotension. What can you say about the rhythm?
This is not an easy rhythm to interpret. That said, several statements can be made about this rhythm, and these should allow one to narrow the differential diagnosis. The five key parameters to assess when interpreting any arrhythmia can be easily remembered with the saying, “Watch your Ps, Qs, and the three Rs.” This saying serves to remind one to always look for P waves (determine if the QRS complex is wide or narrow) and assess the “three Rs” — rate of the rhythm, regularity of the rhythm, and if P waves are present, whether these P waves are related to neighboring QRS complexes. Although it may not always be possible to be certain about the interpretation of some complex arrhythmias, by addressing these five key parameters, one usually will arrive at the most likely possibilities.
Using calipers is the easiest way to measure intervals between successive P waves (i.e., the P-P interval), between successive QRS complexes (i.e., the R-R interval), and between P waves and neighboring QRS complexes (i.e., the PR interval). This instantly allows one to determine whether atrial and ventricular rates are regular and to quickly tell if at least some P waves are conducted (in which case, a similar PR interval will be seen).
Applying these five parameters to the rhythm in the figure, one could say:
- Many P waves are present. These P waves are upright in lead II, as they should be with sinus rhythm. There are R-R intervals within which we see two P waves in succession (i.e., within the R-R intervals of beats 1-2; 2-3; 3-4; and 8-9);
- The P-P interval for each noted place where we see two P waves in succession is fairly constant. Setting calipers to this P-P interval distance suggests that regular P waves occur throughout this tracing;
- The QRS complex is narrow. This reveals this rhythm is supraventricular. The QRS rhythm is irregular; the heart rate varies. In places, the rhythm is quite slow (i.e., the R-R interval between beats 2 and 3 is more than six large boxes in duration, corresponding to a heart rate of less than 50 beats per minute);
- Many P waves do not conduct because they either are not followed by a QRS complex or the PR interval preceding the next QRS complex is too short to conduct (i.e., as it is preceding beat 2);
- One may strongly suspect that at least some P waves are conducting because the PR intervals preceding beats 1, 4, 6, and 9 are equal.
Although complete interpretation of this complex arrhythmia is exceedingly difficult, consider this:
- There is bradycardia with some degree of AV block because many P waves are not conducted. But the fact that the PR interval preceding beats 1, 4, 6, and 9 is constant and the finding of definite irregularity of the ventricular response suggests this is not complete AV block. The rhythm is some form of high-grade, second-degree AV block;
- It appears there is significant ST segment elevation in this lead II rhythm strip, which suggests the reason for this patient’s syncope and her rhythm disturbance may be acute inferior infarction. This must be verified with a complete 12-lead ECG;
- Statistically, the finding of second-degree AV block, in association with a narrow QRS complex and acute inferior infarction, almost always is the result of Mobitz Type I (AV Wenckebach). In contrast, Mobitz Type II AV block is most often associated with QRS widening in a patient with acute anterior infarction.
For further discussion on and more information about this case, please visit: http://bit.ly/35fMyhL.
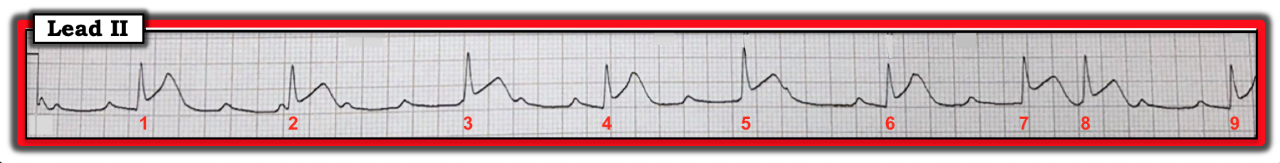
The long lead II rhythm strip in the figure was obtained from a middle-aged woman with syncope and hypotension. What can you say about the rhythm?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
