Can One Be Certain About the Rhythm Diagnosis?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The 12-lead ECG and long lead II rhythm strip in the figure below was obtained from a patient who was hemodynamically stable. What is the rhythm in the figure? Why can one be virtually certain what the rhythm diagnosis is before attempting a vagal maneuver or using medication?
Since it is known this patient is hemodynamically stable, immediate cardioversion is unnecessary, and there is time to contemplate the diagnosis. The five key parameters to assess when interpreting any arrhythmia can be remembered easily by the saying, “Watch your Ps, Qs, and the three Rs.” Look for P waves (or, if no clear P waves are seen, look for atrial activity); determine if the QRS complex is wide or narrow; and assess the rate of the rhythm, regularity of the rhythm, and, if P waves are present, whether these P waves are related to neighboring QRS complexes. Clinicians often vary the sequence in which they look for these five parameters, depending on which ECG features are easiest to assess.
For this figure, the QRS complex is narrow. This means the rhythm is supraventricular. Normal sinus P waves are absent because one does not see a clearly positive P wave with constant and reasonable PR interval in lead II. However, there does appear to be atrial activity in the form of “extra deflections” in a number of leads. The ventricular rhythm is regular. The ventricular rate is approximately 150 beats/minute.
Therefore, there is a regular supraventricular tachycardia (SVT) at ~150 beats/minute without a clear sign of sinus P waves. At this point, the principal differential diagnosis includes: sinus tachycardia, reentry SVT, atrial tachycardia, and atrial flutter.
The most commonly overlooked sustained cardiac arrhythmia is atrial flutter. Because the atrial rate of untreated flutter usually is close to 300 beats/minute, and because the most common ventricular response to atrial flutter is 2:1, the ventricular rate with flutter usually will be close to 300/2 = 150 beats/minute. The best way not to overlook atrial flutter is to suspect it whenever one sees a regular SVT at ~150 beats/minute in the absence of sinus P waves.
The easiest way to identify nonsinus atrial activity is to use calipers. Set calipers to precisely half the R-R interval. Doing so for the rhythm in the figure should allow one to “walk out” regular 2:1 atrial activity in the form of two small positive deflections within each R-R interval in leads aVR and V1, and in the form of two negative deflections within each R-R interval in each inferior lead. This makes for an atrial rate of 150 × 2, or ~300 beats/minute. The only cardiac arrhythmia that results in regular atrial activity at this rate is atrial flutter.
NOTE: For more information about and further discussion on this case, please visit: http://bit.ly/2Tju90D.
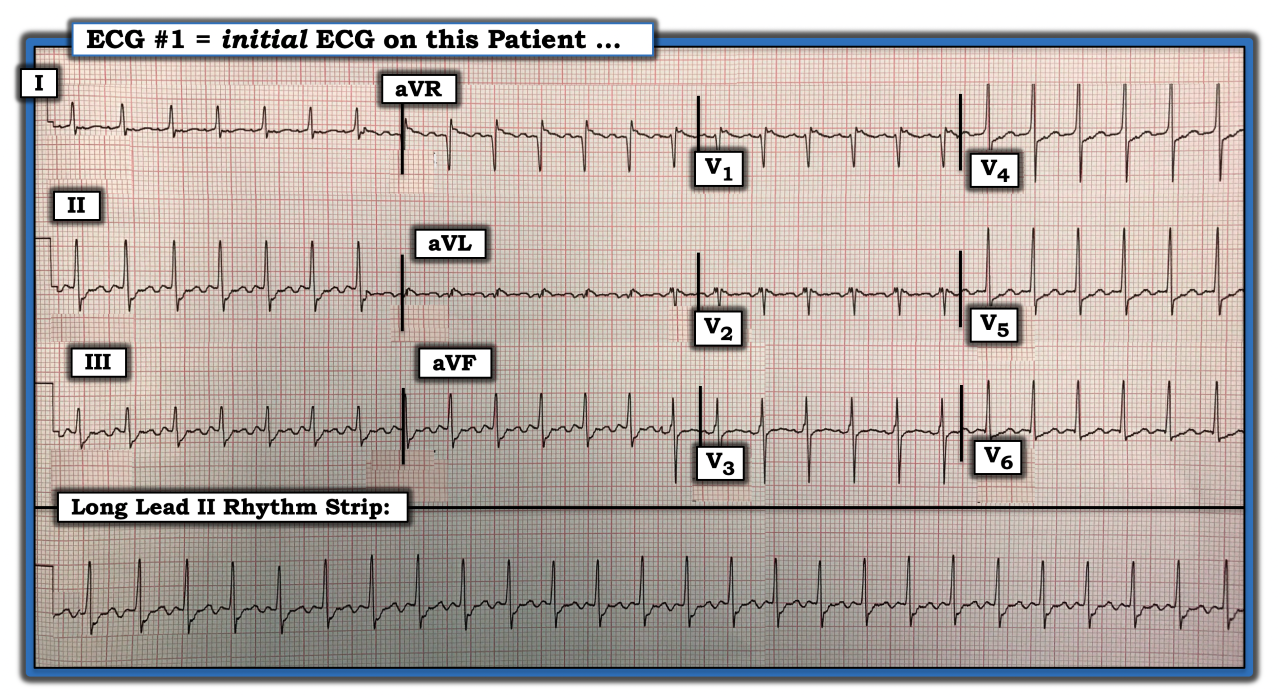
The 12-lead ECG and long lead II rhythm strip in the figure was obtained from a patient who was hemodynamically stable. What is the rhythm in the figure? Why can one be virtually certain what the rhythm diagnosis is before attempting a vagal maneuver or using medication?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
