Special Feature: End-of-life Decision Making: An Evidence-based Approach
Special Feature
End-of-life Decision Making: An Evidence-based Approach
By Leslie A. Hoffman, PhD, RN, Department of Acute/Tertiary Care, School of Nursing, University of Pittsburgh, is Associate Editor for Critical Care Alert.
When critical illness occurs, the primary goal is to assist patients to survive the acute threat to their lives. This goal is commonly achieved with 75%-90% of patients who are admitted to an intensive care unit (ICU) surviving to discharge.1 However, surveys also indicate that approximately 20% of all deaths in the United States occur during or after admission to an ICU.2 Following admission, it is important to insure that all appropriate care is provided and, at the same time, to be vigilant regarding the possibility that recovery consistent with patient values and preferences is no longer possible. This essay explores steps that can be taken to make this difficult transition easier for clinicians, patients, and families.
What Is Known about Communication?
Studies indicate that less than 5% of patients who are critically ill can participate in decision-making regarding their values and preferences.3 Consequently, the family is often placed in the role of surrogate decision-maker. This role can be challenging. Studies indicate that a substantial number of caregivers experience significant emotional distress, including anxiety, depression, or post-traumatic stress disorder, and are at risk for increased mortality.3 In a multicenter study that surveyed 920 family members 48 hours after patients had been admitted to a pediatric or adult ICU, 69% of family members reported symptoms of anxiety and 35% reported symptoms of depression.4 In a study that followed 41 family members for 3-12 months after the death of a patient in the ICU, more than one-third had at least one psychiatric illness, including major depression disorder (27%), generalized anxiety disorder (10%), or panic disorder (10%).5 The challenge, therefore, is to identify ways to ease this burden.
What Increases Family Satisfaction?
Opportunities to Share Concerns. When recovery may not be possible, it is common to schedule a family conference to discuss options and learn family values and preferences. Studies indicate that family conferences may not be fully achieving this goal. From a study enrolling 214 family members, 51 different families and 36 different physicians, findings indicated that physicians spoke 71% of the time and families 29% of the time.6 Increased time speaking on the part of families was associated with increased satisfaction with physician communication and decreased ratings of conflict with the physician. In this study, missed opportunities fell into three categories: 1) to listen and respond to the family; 2) to acknowledge and address family emotions; and 3) to pursue key principles of medical ethics and palliative care, such as the exploration of patient preferences, explanation of surrogate decision making, and affirmation of non-abandonment.6,7
Open Visiting Hours. Although open visiting hours have been identified by families as an important need, a recent regional survey conducted in New England, found that only 32% of ICUs followed this policy.8 Of these, the majority (66%) were non-teaching hospitals. The study also surveyed nurses in these ICUs and reported substantial resistance to open visiting hours. Based on focus-group input, nurses viewed open visiting hours as interfering with their ability to provide care, decreasing control over the environment, and promoting family anxiety due to the extent of time spent in the unit. The authors advocated several possible solutions, including staff education regarding the benefits of greater patient involvement for families and education directed toward improving communication skills when interacting with families. A recent qualitative study reported examples of family presence as calming and helpful during weaning from prolonged mechanical ventilation, beneficial in improving surveillance (e.g., detecting changes, raising concerns, and asking questions of clinicians), as well as a potential hindrance to the weaning process depending on individual family members' actions.9 Communication skill training may be a means of assisting staff to use strategies that optimally promote the benefits of family presence.
Timely Knowledge of Prognosis. Family members typically want to be informed about changes in the patient's condition, to be updated regarding the prognosis, and to have their questions answered honestly in terms that they can understand.3 When family conferences were audiotaped, comments indicated that physicians shared prognoses about quality of life and functional outcomes in almost all conferences. However, prognosis for survival was discussed only about one-third of the time. Less well educated families received the least amount of information about prognosis.10 This observation raises the possibility that less educated family members may be at risk for misunderstanding the gravity of the situation. However, the study provided no insight into whether providing prognostic information about survival would alter satisfaction.
What Should Be Communicated?
Curtis suggests a structured approach to end-of-life decision making based on a summary of available evidence and consensus of opinion:3
- Physicians have an obligation to disclose information about a patient's medical condition and prognosis.
- Family members are an important source of information about the patient's values and preferences.
- Family members should be counseled to use the principle of substituted judgment to guide decisions regarding what the patient would want.
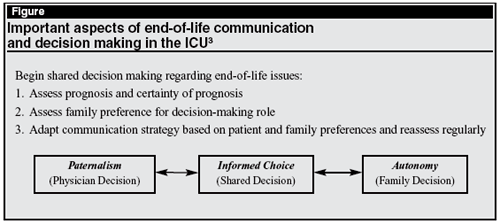
Curtis developed the conceptualization illustrated in the Figure (below) to depict differences in the way family members wish to be involved in end-of-life decision-making.3 In this conceptualization, preference ranges from paternalism (physician makes the decision with limited family input) to autonomy (family makes the decision with limited or no physician input) with a middle range that involves informed choice and joint decision making (shared decision). He advocated that discussions with the family be preceded by an assessment of the patient's prognosis and its certainty, an assessment of family communication preferences, and communication strategies based on this information. Because family preferences can change, the process includes periodic reassessment. This approach avoids a "one size fits all" approach.
Strategies to Make Communication More Effective
Few studies have tested interventions designed to better prepare families for withdrawal of life support. Although limited, evidence is emerging that suggests ways to make this difficult time easier for families before and after life support withdrawal.
 Family Conferences. Prior studies suggest that strategies can make family conferences more effective. As noted previously, it is important to allow family members time to share their questions and concerns. If several members of the health care team will be present, it is helpful to have a "pre-conference" to insure that there is consensus within the interdisciplinary team with regard to goals of the conference, patient prognosis, and what treatments are indicated or not indicated. Statements that acknowledge the difficulty family members are experiencing are important, as well as clear statements that indicate that the patient will not be abandoned and will be kept comfortable. Additional suggestions are included in the Table (left).
Family Conferences. Prior studies suggest that strategies can make family conferences more effective. As noted previously, it is important to allow family members time to share their questions and concerns. If several members of the health care team will be present, it is helpful to have a "pre-conference" to insure that there is consensus within the interdisciplinary team with regard to goals of the conference, patient prognosis, and what treatments are indicated or not indicated. Statements that acknowledge the difficulty family members are experiencing are important, as well as clear statements that indicate that the patient will not be abandoned and will be kept comfortable. Additional suggestions are included in the Table (left).
Access to Written Information. Kirchhoff randomized 22 participants to receive printed information about what to expect during withdrawal of life support or to usual care without this information.11 When contacted by telephone 2-4 weeks later, families in the intervention group expressed greater satisfaction with the information they were provided. The usual-care group reported having to ask for information, not being prepared, and not understanding that time to death can be different for different patients. Rather than being emotion-provoking, the printed information proved to be comforting, based on questionnaire responses and unsolicited comments. The additional step of providing such information is a simple but important means of potentially decreasing grief and depression after the event.
Protocols to Promote Consistent Communication. Mosenthal et al randomized families of 286 patients admitted to a trauma ICU to an intervention—consisting of a palliative care assessment within 24 hours of ICU admission, which encompassed an assessment of the likely prognosis, advance directives, family needs, and surrogate decision-making concerns, and an interdisciplinary family meeting within 72 hours of ICU admission regardless of prognosis during which the likely outcomes, management, and goals of care were discussed—vs usual care, which consisted of family meetings and counseling by bereavement specialists on an "as-needed basis."12 Compared to usual care, rates of mortality, do-not-resuscitate orders, and withdrawal of life support did not change. However, do-not-resuscitate orders were instituted earlier and intervention patients had a shorter ICU and hospital length of stay. There was also a change in the qualitative content of rounds, reflected in more frequent discussions about pain and symptom management and goals of care.
In this study, several components of the intervention (bereavement support, family meetings) were already in use before the intervention was initiated. However, they were implemented in an ad hoc manner, typically when the patient was judged to be terminal. The intervention caused these components to become a standard part of ICU care and resulted in a significant culture change, as evidenced by more frequent discussions of pain and symptom management and goals of care. As with weaning from mechanical ventilation, the major factor causing the change appeared to be a protocol that required a systematized approach for all patients and their families.
Summary
An emerging body of evidence suggests that it is possible to improve the experience of ICU admission for families by implementing strategies that promote timely and open communication and greater access to the patient. Families appear to differ in their wishes for involvement in end-of-life decision making and may change preferences for involvement during the course of the illness. Several studies suggest that relatively minor changes in the way care is delivered can have a significant impact on family satisfaction. These include providing written information regarding what can be expected during withdrawal of life support and implementing a protocol that ensures a palliative care assessment and interdisciplinary team conference within 72 hours of ICU admission for all patients. Further testing is indicated to determine if these positive findings can be replicated in other settings.
References
- Truog RD, et al. Recommendations for end-of-life care in the intensive care unit: A consensus statement by the American Academy of Critical Care Medicine. Crit Care Med 2008;36:953-963.
- Angus DC, et al. Use of the intensive care unit at the end of life in the United States: An epidemiologic study. Crit Care Med 2004;32:638-643.
- Curtis JR, White DB. Practical guidance for evidence-based ICU family conferences. Chest 2008;134:835-843.
- Pochard F, et al. Symptoms of anxiety and depression in family members of intensive care unit patients: Ethical hypothesis regarding decision-making capacity. Crit Care Med 2001;29:1893-1897.
- Siegel MD, et al. Psychiatric illness in the next of kin of patients who die in the intensive care unit. Crit Care Med2008;36:1722-1728.
- McDonagh JR, et al. Family satisfaction with family conferences about end-of-life care in the intensive care unit: Increased proportion of family speech is associated with increased satisfaction. Crit Care Med 2004;32:1484-1488.
- Curtis JR, et al. Missed opportunities during family conferences about end-of-life care in the intensive care unit. Am J Respir Crit Care Med 2005;171:844-849.
- Lee MD, et al. Visiting hours policies in New England intensive care units: Strategies for improvement. Crit Care Med 2007;35:497-501.
- Happ MB, et al. Family presence and surveillance during weaning from prolonged mechanical ventilation. Heart Lung 2007;36:47-57.
- White DB, et al. Prognostication during physician-family discussions about limiting life support in intensive care units. Crit Care Med 2007;35:442-448.
- Kirchhoff KT, et al. Preparing families of intensive care patients for withdrawal of life support: A pilot study. Am J Crit Care 2008;17:113-121.
- Mosenthal AC, et al. Changing the culture around end-of-life care in the trauma intensive care unit. J Trauma 2008;64:1587-1593.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
