Special Feature: Critical Care Management of the Jehovah’s Witness Patient
Special Feature: Critical Care Management of the Jehovah’s Witness Patient
By Grant E. O’Keefe, MD
Few clinical situations place intensive care practitioners in a more uncomfortable position than does treating patients of the Jehovah’s Witness faith. The faith-based refusal of autogenous or allogenic blood transfusions conflicts with the typical life-saving intent implicit in the critical care environment. However, it is our obligation to have a basic level of understanding of the set of beliefs that leads to the choice to refuse this specific set of life-saving therapies, while accepting other aspects of modern medical care. In this article, I will review 4 areas in which critical care practitioners must be knowledgeable in order to care for these challenging patients. In addition to being based upon the published literature, I will make limited general reference to my own experiences in caring for Jehovah’s Witness patients and their families. The 4 areas are: 1) religious basis for not accepting blood transfusions; 2) ethical responsibilities for critical care providers; 3) effect of profound anemia on outcomes and; 4) treatment options.
Religious Basis for Not Accepting Blood Transfusions
Jehovah’s Witnesses view life as God’s gift that is represented by blood. They believe the Bible’s command that Christians must "abstain from blood" (New Testament; Acts 15:28,29). According to the Jehovah’s Witness faith:
"Blood is sacred in God’s eyes and the soul, or life, is in the blood. Jehovah requires that we abstain from blood. This means that we must not take into our bodies in any way at all other people’s blood or even our own blood that has been stored. True Christians will not accept a blood transfusion. They will accept other kinds of medical treatment, such as transfusion of non-blood products. They want to live, but they will not try to save their life by breaking God’s laws." (Taken from: http://www.watchtower.org/library/ rq/index.htm?article=article_12.htm)
Additional biblical passages are considered by Jehovah’s Witnesses to forbid the use of blood, which, while clearly not stated in medical terms, are viewed as ruling out transfusion of whole blood, packed red blood cells, and plasma, as well as white blood cell and platelet administration. The results of accepting these therapies are of great personal and spiritual consequence to those of the Jehovah’s Witness faith—the denial of eternal salvation.
Thus, Jehovah’s Witnesses will not accept treatments that involve the removal and storage of blood or blood products, including autotransfusion of stored blood or techniques of intra-operative hemodilution involving temporary blood storage. However, many will accept the transfusion of albumin and other blood components (coagulation factors, immune globulins, etc). Furthermore, it is felt that the Bible does not comment directly on organ transplantation nor do they infer that these biblical passages refer to organs or non-blood tissue. Therefore, receipt of organs and non-blood tissues is not prohibited, and is left to be decided by the individual.
Ethical Responsibilities for Critical Care Providers
There are many discussions of the ethical decision-making specifically relating to the treatment of Jehovah’s Witnesses or their children. Those included in the list of references provide an excellent discussion of these issues in more detail than presented here. While this is not meant to be a general discussion of biomedical ethics, it is important to consider how the issue of the right to refuse a blood transfusion for religious reasons is evaluated. One of the most widely used frameworks is that of the "4 principles", which include: 1) respect for persons or autonomy; 2) beneficence or maximizing benefits; 3) nonmaleficence or avoiding harm; and 4) justice or fairness in the distribution of risk and benefit.
The principle of respect for persons states that we must respect a competent individual’s decision-making autonomy, even if it may (or will) lead to their death. It could be argued that, in the case of refusal of a life-saving blood transfusion, the principle of respect for persons conflicts with the principle of beneficence. However, we must examine this conflict from the patient’s perspective, and when doing so it is evident that the harm of receiving a transfusion (denial of eternal salvation) is greater than the harm of refusal (end of mortal life), essentially placing these principles in congruence.1 Other approaches determining how to resolve this dilemma exist and essentially arrive at a similar conclusion although through different methods, for other reasons and often with considerable criticism of the "4 principles" approach.2
In contrast to the situation of competent adults deciding for themselves, the balance of both ethical and legal opinion regarding children and individuals not considered competent favors overriding a parent or guardian’s authority and using blood transfusions when medically necessary. In a 1944 ruling (Prince v Massachusetts) the United States Supreme Count determined that a Jehovah’s Witness parent could not neglect her child’s education in order to sell magazines. This ruling indicated that the right of religious freedom is limited insofar as it leads to child abuse, neglect or failure to respect the rights of children. Failing to provide life saving blood transfusions legitimately falls within this intent of this ruling. It is thus considered appropriate when necessary to save a child’s life, to override parental or guardian decisions regarding the use of blood and blood products.
Effect of Profound Anemia on Medical Outcomes
Although the results of recent studies in critically ill patients support minimizing the use of red blood cell transfusions and that it is safe (and perhaps appropriate) to permit mild-to-moderate anemia (hemoglobin ~ 7 g/dL), the safety of lower hemoglobin concentrations is uncertain.3 Observational studies of patients refusing blood transfusions give us some information in this regard. In a combined series of 300 surgical patients with post-operative hemoglobin values of 8 g/dL or less, the risk of death and major morbidity was related to hemoglobin concentration.4 Patients in this series had undergone a range of emergency and elective surgical procedures, mostly under general anesthesia. Overall postoperative mortality was 16%. As shown in the Figure below, the case-fatality rate was 100% for the most profoundly anemic patients (Hemoglobin 2 g/dL or less), although there were only 4 patients in this group. The case-fatality rate remained quite high for patients with a minimum postoperative hemoglobin value of 5 g/dL or less. The presence of preexisting cardiovascular disease had a marked effect on mortality in those with hemoglobin concentrations in the middle of this overall range (3.1-6.0 g/dL), increasing mortality almost 4-fold from 11% to 41%.
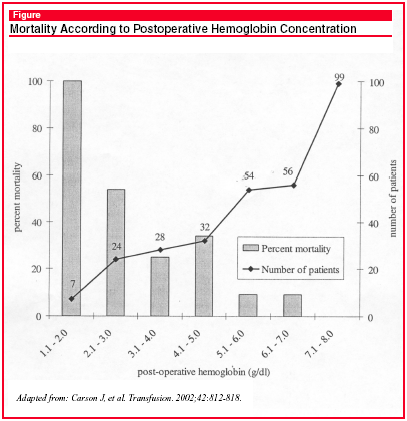
These data refer specifically to postoperative patients, and may not precisely reflect the effect of profound anemia on outcome in a more general critically ill group of patients. There is little information regarding profound anemia in the ICU, but it is clear that hemoglobin levels below 8.0 g/dL are associated with an increased mortality.5 While it is difficult to completely separate the effects of anemia from those of blood transfusions on ICU outcomes, since they are so highly correlated, there is some evidence suggesting independent effects of anemia.6 Thus, taken together, existing data allow us to provide families and patients with an estimate of how hemoglobin levels of less than 7-8 g/dL will influence outcome.
Treatment Options
Minimizing iatrogenic blood loss and considering therapeutic options that (while seemingly more invasive) more reliably control bleeding are appropriate and obvious considerations. Point-of-care systems exist for blood chemistry analysis that do not require that blood be removed from the patient. Whether these systems warrant the extra expense as compared to simply drawing smaller volumes of blood and limiting testing is uncertain. It may be helpful to have direct discussions with the Director of Laboratory Medicine to determine the minimum volumes of blood needed for various analyses.
It is also important to establish early in the course of the illness what is and is not acceptable to the patient. As indicated above, individuals may accept certain treatments, such as intra-operative blood salvage with immediate transfusion, whereas others may not. For many, the critical factor in accepting auto-transfusion is whether the system is closed, with the circuit and patient remaining in continuity. By ensuring this principle of keeping the blood in continuity with the patient, acute normovolemic hemodilution is often acceptable to a Jehovah’s Witness. This issue is particularly relevant in emergent and elective surgical procedures associated with large blood loss. It is thus important to discuss these specific issues with patients and their families early and often.
Often, these issues are introduced by the patient or by family members. It is my experience that Jehovah’s Witnesses are knowledgeable of their options and often have a contact person affiliated with a "bloodless medicine program," particularly if they live in a moderate- to large sized metropolitan area. Information about these programs is available through the Internet, although the quality and accuracy of the information likely varies widely. It is important for us as critical care clinicians to expect and accept a request by family members for us to discuss and consult with a representative of such a program. It is my experience that such consultations can be helpful, indicating to the patient and family that we will consider all options, and that the individuals involved in these programs are knowledgeable and not overbearing.
The management of bleeding patients (as in gastrointestinal hemorrhage, blunt abdominal trauma, etc) requires experienced surgical decision-making-particularly in this era of newer, nonoperative approaches for treating hemorrhage. In many circumstances, operative treatment (eg, splenectomy for trauma or surgical ligation of a bleeding duodenal ulcer) is the most "conservative" and appropriate option, that should be considered earlier then may otherwise be the case. In other circumstances, an earlier and more aggressive approach to the use of newer nonsurgical approaches (eg, trans-cathether angioembolization, vascular stent graft placement, etc) may seem warranted. However, there is a near absence of information, even in the form of case reports and case series, addressing the safety of such newer approaches in patients in whom our options for blood product use are limited. Therefore, any decisions to use these newer options for bleeding control or management of vascular emergencies must include input from all clinical services potentially involved in managing the problem at hand (eg, surgery, interventional radiology, gastroenterology, etc).
In all cases, attempts to maximize erythropoiesis are warranted and should be started early. Iron supplementation with oral ferrous sulfate (325 mg by mouth 3 times daily, providing a total of 195 mg of elemental iron) is often recommended, but gastrointestinal absorption is questionable in severely ill patients, particularly those with ongoing evidence of shock or those with an ileus.7 Therefore, it is reasonable to consider parenteral iron supplementation. Our approach has been to use iron sucrose (100 mg intravenously once daily for a maximum of 10 days). The risk of anaphylaxis appears to be less with iron sucrose or iron gluconate than with iron dextran. Whether parenteral iron provides greater availability, higher hemoglobin concentrations, and better outcomes is completely unknown.
Recombinant human erythropoietin has been evaluated in clinical trials involving a wide range of diseases associated with anemia including critical illness. The drug has been shown to increase hemoglobin concentrations and to reduce the need for red blood cell transfusions in anemic critically ill patients.7,8 Although it is not our standard practice to use erythropoietin in our general population of critically ill patients, we will use it early in Jehovah’s Witness patients. The recommended dose is 40,000 U weekly for anemic critically ill patients. For critically ill Jehovah’s Witness patients, other authors have suggested more aggressive strategies involving more frequent (up to daily) and somewhat higher (600 U/kg body weight) doses. Our approach has been to use 40,000 U daily for 3 days and then return to a once-weekly schedule. After administration, reticulocytosis often begins within 5 days and peaks around 8 days. Increases in hemoglobin concentrations are generally not seen until 8-12 days after administration.9
Hemoglobin substitutes represent an emerging therapy that seems ideally suited for critically ill and anemic Jehovah’s Witness patients. Cothren and colleagues reported on a seriously injured patient whom they treated with recombinant erythropoietin and Polyheme, an stroma-free polymerized and pyridoxalated hemoglobin solution (Northfield Laboratory, Ill).10 However, it will be some time before this and other artificial hemoglobin products are approved and/or available for general use. Furthermore, while this particular substitute appears safe, the cumulative benefits in improving outcomes in addition to other aspects of care are suggestive but not established.11,12 n
References
1. Macklin R. J Med
Ethics. 2003; 29(5):275-280.
2. Callahan D. Principlism and communitarianism. J Med Ethics 2003; 29(5):287-291.
3. Hebert PC, et al. N Engl J Med. 1999;340(6):409-417.
4. Carson JL, et al. Transfusion. 2002;42(7):812-818.
5. Corwin HL, et al. Crit Care Med. 2004;32(1):39-52.
6. Hebert PC, et al. Am J Respir Crit Care Med. 1997; 155(5):1618-1623.
7. Corwin HL, et al. JAMA. 2002;288(22):2827-2835.
8. Corwin HL. Semin Hematol. 2001;38(3 Suppl 7):24-32.
9. Cheung W, et al. Eur J Clin Pharmacol. 2001; 57(5):411-418.
10. Cothren C, et al. N Engl J Med. 2002;346(14): 1097-1098.
11. Gould SA, et al. J Am Coll Surg. 1998;187(2):113-120.
12. Gould SA, et al. J Am Coll Surg. 2002;195(4):445-452.
Grant E. O’Keefe, MD, Department of Surgery, Harborview Medical Center, University of Washington, is Associate Editor of Critical Care Alert.
Few clinical situations place intensive care practitioners in a more uncomfortable position than does treating patients of the Jehovahs Witness faith. The faith-based refusal of autogenous or allogenic blood transfusions conflicts with the typical life-saving intent implicit in the critical care environment. However, it is our obligation to have a basic level of understanding of the set of beliefs that leads to the choice to refuse this specific set of life-saving therapies, while accepting other aspects of modern medical care.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
