Coenzyme Q10 for Neurodegenerative Diseases
By Dónal P. O’Mathúna
Neurodegenerative diseases include a variety of neurological disorders such as Huntington’s disease, Parkinson’s disease, amyotrophic lateral sclerosis (ALS), and mitochondrial cytopathies. Although each disease manifests itself differently, a small number of biochemical processes are believed to be involved in all the disorders.1 Much evidence has accumulated suggesting that mitochondrial defects are involved in the pathogenesis of these diseases.2 This has led to a search for agents that can prevent or slow disease progression at the mitochondrial level. Coenzyme Q10 (also called CoQ10, ubiquinone, or ubidecarenone) is one such agent being investigated for its potential as a neuroprotective agent in a number of diseases.3 In addition, a committee at the National Institute of Neurological Disorders and Stroke recently identified CoQ10 as an agent warranting further clinical investigation for Parkinson’s disease.4
Biochemistry
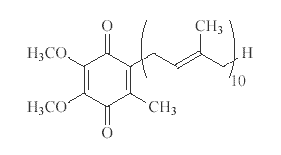
Coenzyme Q is the name given to a group of compounds containing a ring structure and a long chain made up of repeating five-carbon sections called isoprenoid units (see Figure).3 In the Figure, the parentheses enclose one isoprenoid unit, with the subscript indicating the number of isoprenoid units in the particular compound. Human coenzyme Q contains 10 isoprenoid units, hence the name CoQ10. The bacterial form is CoQ5, whereas the rodent form is CoQ9. Coenzyme Q is an essential cofactor in the electron transport chain (ETC) and a potent antioxidant.5 It carries out both roles within mitochondria, the powerhouses of all cells. The cofactor is highly lipid-soluble and lodges within the lipid layers of the inner membranes of mitochondria.
|
Mechanism of Action
The ETC in mitochondria replenishes the chemical energy molecule called adenosine triphosphate (ATP). The ETC is made up of several complexes, with CoQ10 playing a vital role in Complex I and Complex II/III.3 A group of people using synthetic opiate drugs developed symptoms of Parkinson’s disease.2 The drugs were later found to be contaminated with 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP), which selectively inhibits Complex I of the ETC.2 The parkinsonism produced by MPTP was reduced significantly when animals were given CoQ10 along with MPTP.3
These discoveries led to investigations into whether CoQ10 levels were changed in patients with Parkinson’s disease. Some studies found reduced CoQ10 levels, which were increased significantly by oral CoQ10 supplements.3 However, other studies found no significant differences between the CoQ10 serum levels in patients with Parkinson’s disease compared to controls.6 CoQ10 supplementation in animals also has been found to protect against experimentally induced forms of Huntington’s disease and ALS. The potential role of CoQ10 in Huntington’s disease is more poorly understood, although substantial evidence links impaired energy metabolism to disease development.7 All these results have led to proposals that CoQ10 has a neuroprotective effect both by improving ETC function in mitochondria and acting as an antioxidant.
Clinical Studies
In animal models of ischemia, ALS, Parkinson’s disease, and Huntington’s disease, CoQ10 administration increased animal survival and functionality.3 Based on these results, a small number of clinical studies have been conducted involving patients with Parkinson’s disease or Huntington’s disease. A multicenter randomized controlled trial (RCT) enrolled 347 patients in the early stages of Huntington’s disease.8 Subjects were randomized to receive either CoQ10 (300 mg bid), remacemide (200 mg tid), both, or neither. Remacemide is an antagonist of a receptor whose activation is suspected to play a role in the development of Huntington’s disease. Patients’ total functional capacity was evaluated every 4-5 months for 30 months. None of the interventions produced a significant impact on functional capacity. CoQ10 did show a 13% slowing of functional decline beginning one year into the trial, but this was not statistically significant (P = 0.15).
An open-label pilot study was conducted with 10 patients with Parkinson’s disease.9 All patients were given 100 mg bid CoQ10 capsules. After three months, no changes were measured using the Unified Parkinson Disease Rating Scale (UPDRS). However, this study used a relatively low dose of CoQ10 and the significance of UPDRS scores not deteriorating could not be evaluated because no control group was used.
A multicenter RCT was conducted with 80 patients with early Parkinson’s disease who were not receiving concomitant medications.5 Subjects were randomly assigned to receive placebo or CoQ10 at dosages of 300, 600, or 1200 mg/d. All medications were prepared in capsules containing 300 IU vitamin E and taken four times daily. Subjects were evaluated using the UPDRS every four months for 16 months, or until they required levodopa treatment. All groups taking CoQ10 showed slowed deterioration compared to placebo, but the difference was statistically significant only for those taking 1200 mg/d (P = 0.04). Slower decline occurred in all three parts of UPDRS: cognitive function, motor skills, and daily activities. Biological analyses showed highly significant increases in serum CoQ10 levels that were dose-dependent (P < 0.001) and increased mitochondrial ETC activity (P = 0.04).
Adverse Effects
Adverse effects in the clinical trials were all mild, primarily GI disturbances. However, in one study of 15 patients with Parkinson’s disease given varying CoQ10 doses, two patients taking 800 mg/d had abnormal urinalyses.10 They had 3-5 hyaline casts per low power field and trace protein upon repeat urinalysis. These changes were transient and of unclear clinical significance, but the authors recommended prudent monitoring of renal function on higher CoQ10 doses.
Drug Interactions
CoQ10 is chemically similar to vitamin K and may have similar pro-coagulant activity, with four cases of decreased effectiveness of warfarin reported and thought to be related to CoQ10.11 The HMG CoA reductase inhibitors (statins) inhibit cholesterol and CoQ10 synthesis, leading to lower CoQ10 levels. Whether this is clinically significant is unknown. There are some concerns that CoQ10 supplements may interfere with medications for hypertension or diabetes, but these effects are not believed to be widespread.11
Formulation
CoQ10 supplements are formulated as oil-based capsules, powder-filled capsules, tablets, and soft-gel capsules containing microemulsions.12 The highly lipophilic nature of CoQ10 makes its absorption poor, highly variable, and strongly dependent on the contents of the stomach. It is best taken with food, especially fat-rich foods. Its poor bioavailability has led to the development of solubilized formulations using soy bean oil or emulsifying agents. A bioavailability study of four commercially available products examined three solubilized products and one non-solubilized powder that is found in many OTC products.13 The three solubilized formulations produced significant and similar increases in plasma CoQ10 concentrations, but the powder led to barely detectable increases in plasma concentrations above baseline. Similar bioequivalence results have been produced previously.14
Although gel caps have been the favored form of CoQ10, wafers have become widely available. However, no data could be found to demonstrate whether wafers are absorbed as well as gel caps.
Conclusion
Much remains to be understood regarding the causes and treatment of various neurodegenerative diseases. Evidence indicates that mitochondrial defects play an important role. At the same time, CoQ10 supplementation is being shown to improve mitochondrial metabolism. CoQ10 is also well tolerated. However, the results of clinical trials designed to evaluate whether CoQ10 protects against disease progression have been mixed. In Huntington’s disease, a small but non-significant benefit was shown. In Parkinson’s disease, the highest dose used resulted in significant slowing of deterioration. However, the authors of this Parkinson Study Group trial noted that it is still premature to recommend CoQ10 for the treatment of Parkinson’s disease before their results are replicated in a larger Phase III study.5
Recommendation
Given the lack of significant benefit found to date, CoQ10 should not be recommended for patients in the early stages of Huntington’s disease. Whether it might be beneficial for those at risk of the disease, or in later stages, remains to be studied. For patients with Parkinson’s disease, the data to date are more promising, but the Parkinson Study Group still concluded it was too early to recommend that patients start using CoQ10 supplements. With the limitations of current medications, and the relative freedom of CoQ10 from adverse effects, CoQ10 may be a viable option once patients discuss their proposal with their neurologist.
Given that CoQ10 is readily available as a dietary supplement, patients may already be using it or planning to try it. In that case, they should be reminded that dietary supplements are not subject to the same quality and content regulations as pharmaceutical drugs. Patients with neurodegenerative diseases should be cautioned that at a dose of 600-1200 mg/d, CoQ10 supplements could easily cost more than $100 per month.8 Patients will therefore need help evaluating the quality of available brands, and should be actively monitored for potential adverse effects or drug interactions.
Dr. O’Mathúna teaches courses in bioethics and alternative medicine in Dublin, Ireland, and is Visiting Professor of Bioethics at the University of Ulster, Coleraine, Northern Ireland.
References
1. Tarnopolsky MA, Beal MF. Potential for creatine and other therapies targeting cellular energy dysfunction in neurological disorders. Ann Neurol 2001;49:561-574.
2. Beal MF. Bioenergetic approaches for neuroprotection in Parkinson’s disease. Ann Neurol 2003;53(suppl 3): S39-S47.
3. Beal MF. Coenzyme Q10 administration and its potential for treatment of neurodegenerative diseases. Biofactors 1999;9:261-266.
4. Ravina BM, et al. Neuroprotective agents for clinical trials in Parkinson’s disease: A systematic assessment. Neurology 2003;60:1234-1240.
5. Shults CW, et al. Effects of coenzyme Q10 in early Parkinson disease: Evidence of slowing of the functional decline. Arch Neurol 2002;59:1541-1550.
6. Jiménez-Jiménez FJ, et al. Serum levels of coenzyme Q10 in patients with Parkinson’s disease. J Neural Transm 2000;107:177-181.
7. Ferrante RJ, et al. Therapeutic effects of coenzyme Q10 and remacemide in transgenic mouse models of Huntington’s disease. J Neurosci 2002;22:1592-1599.
8. Huntington Study Group. A randomized, placebo-controlled trial of coenzyme Q10 and remacemide in Huntington’s disease. Neurology 2001;57:397-404.
9. Strijks E, et al. Q10 therapy in patients with idiopathic Parkinson’s disease. Molec Aspects Med 1997;18 (suppl):S237-S240.
10. Shults CW, et al. Absorption, tolerability, and effects on mitochondrial activity or oral coenzyme Q10 in parkinsonian patients. Neurology 1998;50:793-795.
11. Coenzyme Q-10. Available at www.naturaldatabase.com. Accessed Oct. 15, 2003.
12. Coenzyme Q10 (CoQ10). In: PDR for Nutritional Supplements. Montvale, NJ: Medical Economics, 2001:103-106.
13. Miles MV, et al. Bioequivalence of coenzyme Q10 from over-the-counter supplements. Nutr Res 2002; 22:919-929.
14. Chopra RK, et al. Relative bioavailability of coenzyme Q10 formulations in human subjects. Int J Vitam Nutr Res 1998;68:109-113.
O'Mathuna DP. Coenzyme Q10 for neurological diseases. Altern Med Alert 2003;6(12):133-136.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.