Oral Contraceptive Mortality
Abstract & Commentary
Vessey, Painter, and Yeates from the University of Oxford used the prospective cohort of women enrolled in the Oxford Family Planning Association Study to assess mortality in users and nonusers of oral contraceptives. By the end of the year 2000, 889 deaths had occurred in 17,032 women in England and Scotland enrolled in the study. There was no increase in breast cancer associated with oral contraceptives in either smokers or nonsmokers. However, death from cervical cancer was increased with oral contraceptive use (although the confidence intervals were very wide because of small numbers). Mortality from endometrial cancer and ovarian cancer were reduced in the oral contraceptive users, a result consistent with many previous reports. Comparing never users and users, there was an 80% overall reduction in endometrial cancer deaths and a 60% reduction in ovarian cancer deaths. The risk of deaths from all causes was significantly increased only in smokers (especially with 15 or more cigarettes daily), and the risk increased with increasing age (Vessey M, Painter R, Yeates D. Lancet. 2003;362:185-191).
Comment by Leon Speroff, MD
The conclusions of this prospective cohort study are limited by the small numbers of deaths in the various categories, as indicated by the wide confidence intervals. However, the results are consistent with a very large literature and further strengthened because they are derived from a single cohort of women. It is important to point out that the data are derived largely from the use of products containing 50 mg ethinyl estradiol, a dose that is now considered to be high. For this reason, the overall safety of oral contraceptives in this report is reassuring, and we would expect even better results with modern, low-dose formulations.
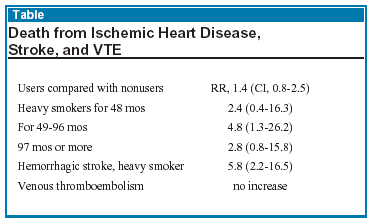
This report confirms previous reports (especially the publications from the World Health Organization and the Nurses’ Health Study) that the risk of cardiovascular mortality associated with oral contraceptives is confined to smokers. It is very likely that this risk is present only in current users, an observation that could not be documented in the Oxford study because of the design.
The accumulated literature over many years has consistently established an increased risk of venous thrombosis associated with oral contraceptives. The Oxford report identified no deaths from venous thromboembolism that could be attributed to oral contraceptive use. Most deaths from this condition are linked to trauma, surgery, or a major illness.
The experience with oral contraceptives, in my view, emphasizes the importance of good patient screening. The occurrence of arterial thrombosis is essentially limited to older women who smoke or have other cardiovascular risk factors, especially hypertension. Avoiding the use of oral contraceptives in older smokers and hypertensive women requires effective interaction between the patient and a clinician (not necessarily a physician). Providing oral contraceptives over the counter would bypass this vital interaction, and undoubtedly there would be deaths that could have been avoided.
Dr. Speroff is Professor of Obstetrics and Gynecology Oregon Health Sciences University Portland.
Vessey, Painter, and Yeates from the University of Oxford used the prospective cohort of women enrolled in the Oxford Family Planning Association Study to assess mortality in users and nonusers of oral contraceptives.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
