What’s the Buzz? Honey for Topical Wound Dressings
What’s the Buzz? Honey for Topical Wound Dressings
By Susan T. Marcolina, MD, FACP
PART II OF A SERIES ON APITHERAPY
Although wound salves containing honey were mentioned on Egyptian papyri dating back to 2500 BC, honey is not well recognized for its use as a topical medication in modern times.1 There has been a resurgence of interest in honey for this purpose, however, with the emergence and proliferation of antibiotic resistant microbes, such as methicillin-resistant Staphylococcus aureus and vancomycin-resistant enterococcus in non-healing wounds. Curiously, there appears to be something to it.
Honey Production
Bees gather nectar from flowering plants and transform it into honey with the addition of enzymes. One of these enzymes is invertase, which converts the sucrose in the nectar into glucose and fructose: The sucrose content of honey is generally just 1% of the total sugar content. Another enzyme is glucose oxidase, which is inactive in ripened honey and becomes activated with dilution to form hydrogen peroxide and gluconic acid from glucose. Hydrogen peroxide and gluconic acid impart antibacterial activity.
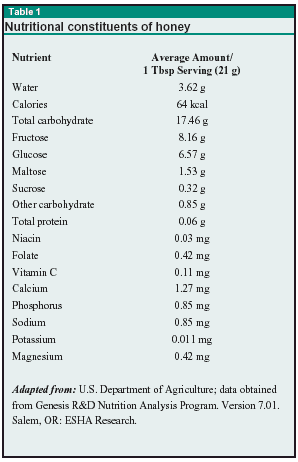
Bees store nectar in honeycomb cells and evaporate water from it by rapid wing ventilation. Once the water concentration is about 18%, the bees cap off the cells.2,3 Table 1 delineates the nutritional constituents of honey.
Properties Responsible for Antibacterial Activity
Table 2 outlines the therapeutic attributes and key properties of honey.2

The major antibacterial effects exerted by honey result from its glucose oxidase enzyme content. This enzyme catalyses the reaction, which produces acid (primarily gluconic acid) and hydrogen peroxide from glucose, water, and oxygen.4 In addition, several phytochemicals present in honey—including flavonoids, catalase, and ascorbic acid—perform antioxidant functions. They also function as nonperoxide antibacterial factors, which may account for honey’s antibacterial activity, even after inactivation of the glucose oxidase enzyme.5
Honey itself is not easily subject to bacterial activity. As a supersaturated solution of sugars, honey has a high osmotic pressure and low water activity (Aw) values, which range from approximately 0.5 (16% water) to 0.6 (18.3% water); most bacteria grow with an Aw between 0.94-0.99. The pH of honey ranges from 3.2-4.5, and this acidity also inhibits many bacterial pathogens. If honey is diluted by body fluids, however, its pH will increase, the osmolarity will decrease, and the acidity and osmolarity alone will no longer inhibit bacterial growth.
In Vitro Assessment of Antibacterial Potency
In vitro experiments show that honey stimulates peripheral proliferation of B lymphocytes and T lymphocytes at concentrations of 0.1%. Honey also stimulates monocytes to release cytokines, tumor necrosis factor-alpha, IL-1, and IL-6, which activate immune responses to infection.6,7
Allen et al analyzed 345 samples of New Zealand honeys from 26 different floral sources and found greater than a 30-fold difference in the range of antibacterial activity.8 Differences in floral origin and seasonal conditions are responsible for some variability. Studies have shown high antibacterial levels exist in a specific type of honey derived from the nectar of Leptospermum scoparium, locally known as the manuka bush, which grows uncultivated throughout New Zealand.9
Willex et al performed in vitro testing of the activity of a standardized New Zealand manuka honey of median antibacterial activity against seven species of bacteria, including clinical isolates of S. aureus, and found the minimal inhibitory concentration (MIC) ranged from 2% to 4%.10 Cooper et al tested the antibacterial activity of the median manuka honey against 20 infected wound isolates of Pseudomonas and found the MIC to range from 5.5% to 9.0%.11
Clinical Studies
Al-Waili et al performed a randomized controlled trial of 50 patients who had postoperative wound infections with gram-positive and gram-negative bacteria following cesarean section and hysterectomy.12 Twenty-six patients had honey dressings applied to their wounds and 24 had their wounds washed with 70% ethanol followed by application of povidone-iodine. The honey-treated group had complete healing with eradication of infection in less than half the time required by the antiseptic-treated group.
In two randomized clinical trials comparing the use of honey vs. silver sulfadiazine (SSD) gauze dressing in two groups of 52 patients13 and SSD cream in two groups of 25 patients,14 Subrahmanyam showed that honey was significantly superior to both SSD products in the treatment of superficial burn injuries with quicker wound sterilization, complete healing, and a lower incidence of hypertrophic scar and post-burn contracture. Allergic or other side effects were not observed. A major drawback of these studies was the lack of identification of floral source and antibacterial standardization of the honeys used.
Vardi et al performed an observational study of the effect of topical honey dressings in nine infants with large, infected, recalcitrant surgical wounds.15 Marked improvement was seen in all cases within five days and all wounds were cleared within 21 days. Again, the study identified neither a floral source nor antibacterial standardization for the honey. In addition, the honey used was not sterilized with gamma-irradiation. This study reported no adverse effects in terms of electrolyte imbalances, hyperglycemia, local tissue irritation, or wound botulism.
Formulation
Since the glucose oxidase enzyme is both thermolabile and light-sensitive, the antibacterial properties of honey can be affected both by processing and storage conditions. Most commercial food honeys have not been standardized for antibacterial potency and, therefore, are not suitable for use as topical wound therapy.16 Despite the fact that some unpasteurized floral types of honey in the United States have good antibacterial activity, commercial processing destroys this activity.
Honey intended for wound care is extracted and processed in facilities that use specialized machinery for filtering out small particulates such as pollen while exposing the honey to minimal heating to protect the heat-labile components. According to Molan et al, the honey is then gamma-irradiated, which effectively destroys any clostridial spores without compromising its antibacterial activity.17
Safety Issues
Like other natural products, the composition of honey is not constant. It often contains pollen particulates, bee parts, non-pathogenic Bacillus bacteria species, and, importantly, clostridial spores. Such spores, if ingested, can cause infant botulism or may be inoculated into a wound causing further damage.18 The other particulates may cause granuloma formation if embedded in healing wounds. Honeys specifically formulated for wound care are commercially available and only these honeys should be used for this purpose.19
Adverse Effects
Both proteins derived from pharyngeal and salivary secretions of honeybees and pollen proteins contained in honey can cause allergic reactions. Therefore, persons with pollen and honey allergies should avoid the use of topical honey therapy for wounds.20
In papers describing the application of topical honey to open wounds, a few instances of a stinging sensation have been reported in a few instances, possibly secondary to the acidity of the honey after initial application. In general, however, the application of topical honey has been reported to be soothing and analgesic.4 Honeys used for wound therapy should be gamma-irradiated to ensure sterilization of clostridial spores, which could, in theory, be responsible for wound botulism if inoculated into healing wounds.15,17
Regulation
In May 1999, the Therapeutic Goods Administration of Australia approved the use of Medihoney, which is 100% standardized manuka honey as a primary wound dressing.21
Conclusion
At the present time, in Australia and New Zealand, specific honey that has been found in laboratory testing to have high antibacterial potency is being marketed (in Australia, with medical approval) for topical wound care. Despite laboratory studies that document the bactericidal effects of a specific type of honey and favorable outcomes in several clinical studies in patients with recalcitrant wounds of various etiologies, the unselected, nonstandardized honeys used make the clinical data difficult to interpret and impossible to duplicate due to lack of documentation.
Though the laboratory investigations and the micro-bacteriologic sensitivities merit careful consideration of honey for use as a wound dressing, more clinical research with different honeys of standardized antibacterial potency needs to be performed to elucidate the patients and types of wounds that would benefit most from intervention with a particular honey.
Recommendation
Further in vitro testing is necessary to identify and standardize other types of honey with high antibacterial and antioxidant potency. Such honey should be tested against currently used topical wound therapies in blinded, randomized, controlled trials in order to elucidate the most effective situations in which to use this dressing. Studies done to date do not support its general clinical use, but certain types of honey remain promising possibilities for future wound care treatment.
Dr. Marcolina is a board-certified internist and geriatrician in Issaquah, WA.
References
1. Jones R. Honey and healing throughout the ages. In: Munn P, Jones J, eds. Honey and Healing. Cardiff, United Kingdom: International Bee Research Association, 2001.
2. Honey Health and Therapeutic Qualities. Available at: www.nhb.org.
3. The Biology of the Honeybee, Apis mellifera. Available at: http://koning.ecsu.ctstateu.edu.
4. Honey as an antimicrobial agent. Available at: http://honey.bio.waikato.ac.nz/honey_intro.shtml.
5. Cooper RA, et al. Antibacterial activity of honey against strains of Staphylococcus aureus from infected wounds. J R Soc Med 2000;92:283-285.
6. Abuharfeil N, et al. The effect of bee honey on the proliferative activity of human B and T lymphocytes and the activity of phagocytes. Food Agric Immunol 1999; 11:169-177.
7. Tonks A, et al. Stimulation of TNF-alpha release in monocytes by honey. Cytokine 2001;14:240-242.
8. Allen KL, et al. A survey of the antibacterial activity of some New Zealand honeys. J Pharm Pharmacol 1991;43:817-822.
9. Molan PC. The role of honey in the management of wounds. J Wound Care 1999;8:415-418.
10. Willix DJ, et al. A comparison of the sensitivity of wound-infecting species of bacteria to the antibacterial activity of manuka honey and other honey. J Appl Bacteriol 1992;73:388-394.
11. Cooper RA, et al. The use of honey as an antiseptic in managing Pseudomonas infection. J Wound Care 1999;84:161-164.
12. Al-Waili NS, Saloom KY. Effects of topical honey in post-operative wound infections due to gram positive and gram negative bacteria following cesarean section and hysterectomy. Eur J Med Res 1999;4:126-130.
13. Subrahmanyam M. Topical application of honey in treatment of burns. Br J Surg 1991;78:497-498.
14. Subrahmanyam M. A prospective randomized clinical and histological study of superficial burn wound healing with honey and silver sulfadiazine. Burns 1998; 24:157-161.
15. Vardi A, et al. Local application of honey for the treatment of neonatal post operative wound infection. Acta Paediatr 1998;87:429-432.
16. Medihoney. Available at: www.medihoney.com/woundcare.htm.
17. Molan PC, Allen KL. The effect of gamma-irradiation on the antibacterial activity of honey. J Pharm Pharmacol 1996;48:1206-1209.
18. Midura TF, et al. Isolation of Clostridium botulinum from honey. J Clin Microbiol 1979;9:282-283.
19. Where to get honey for medical use. Available at http://honey.bio.waikato.ac.nz/where.shtml
20. Bauer L, et al. Food allergy to honey: Pollen or bee products? J Allergy Clin Immunol 1996;97:65-73.
21. Honey treatment approved. Available at: http://www-personal.buseco.monash.edu.au/~agribiz/.
Marcolina S. What's the buzz? Honey for topical wound dressings. Altern Med Alert 2003;6(3):30-33.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
