Guafenesin and SAM-e for Fibromyalgia
Guafenesin and SAM-e for Fibromyalgia
By Sharon L. Kolasinski, MD, FACP, FACR
Fibromyalgia is a common disorder of unknown etiology characterized by chronic fatigue, diffuse pain throughout the body, and the presence, on physical examination, of multiple points that are tender to the touch.1 In addition, patients may suffer from irritable bowel syndrome, irritable bladder syndrome, headaches, and other symptoms related to altered sensory perception.2 The severity of symptoms varies considerably between patients, but constant pain and fatigue are typical.
There is no known cure for fibromyalgia and no one medication treats every aspect of the disorder, nor is any given therapy helpful in all patients. This has led patients with fibromyalgia to explore many types of treatments, including alternative therapies. A number of epidemiological surveys have shown that more than 90% of those with fibromyalgia use alternative therapies.3 Recently, this has come to include the use of guafenesin and S-adenosylmethionine (SAM-e), both readily available over the counter products.
Guafenesin: Rationale for Use
R. Paul St. Amand, MD, an endocrinologist in private practice for almost 40 years and clinical assistant professor of medicine at the University of California at Los Angeles Harbor campus, has championed the use of guafenesin for fibromyalgia. St. Amand has not authored any peer-reviewed publications regarding his observations of treatment with guafenesin, but his views are readily available for review on his web site, www.guaidoc.com. St. Amand was interviewed for this article. He has treated more than 2,000 patients with his guafenesin regimen.
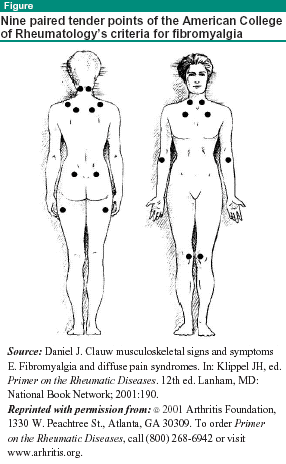
Occasionally, palpable muscle spasm can occur along with the signs and symptoms of fibromyalgia. Sometimes a patient will complain of the sensation of a "knot" under the skin with or without the presence of palpable spasm. Using an approach that is not standard in the rheumatology community, St. Amand focuses heavily on the presence of "distinct, swollen lesions" that he feels arise as a result of these muscular contractions in virtually all fibromyalgia patients. Although the standard evaluation of patients with fibromyalgia includes a determination of whether any of 18 pre-defined tender points (see Figure below) are present, St. Amand favors mapping the palpable lesions. He uses these maps as one of his most important outcome measures in gauging the response to guafenesin therapy.
St. Amand believes that fibromyalgia is an inherited disorder in which renal tubular resorption of phosphate is impaired. He hypothesizes that a cellular accumulation of phosphate occurs in patients with this defect and that ATP-dependent sarcomeric calcium pumps malfunction as a result. This, in turn, results in muscular contraction.
A further, nonstandard observation St. Amand claims to have made is that fibromyalgia symptoms improve when patients are treated with uricosurics. He further states that guafenesin is weakly uricosuric and, without laboratory evidence, that this is the basis of its beneficial effects. He claims that guafenesin is more effective and has fewer side effects than agents he previously tried, including probenecid and sulfinpyrazone. However, he does not feel that the benefit derives directly from being uricosuric, because he does not think uric acid is the etiologic factor in fibromyalgia. Rather, he feels that inorganic phosphate is at least partially to blame. No direct experimental evidence supports this contention. However, St. Amand states that he has collected 24-hour urine specimens that reveal increased excretion of phosphate, calcium, and oxalate from guafenesin-treated patients. He also cites work by others that showed modestly decreased ATP levels in the biopsied muscles of fibromyalgia patients4 as evidence that phosphate metabolism may be involved in the pathogenesis.
St. Amand begins patients on a dose of 300 mg PO bid and works up to doses as high as 600 mg PO tid. He reports that the symptoms of fibromyalgia are exacerbated when guafenesin therapy is initiated and that this represents the beginning of the therapeutic response. Palpable painful areas are mapped and doses are adjusted according to response. St. Amand describes guafenesin as innocuous and claims that lesions eventually are cleared and the disease is reversed. The time to reversal is proportional to the time that the patient has had the disease.
A final hypothetical point that St. Amand stresses is that exposure to salicylates in virtually any form can interfere with the effectiveness of guafenesin. He cautions that use of aspirin or salicylate-containing drugs or use of topical salicylate-containing compounds can block completely the uricosuric effects of guafenesin. Again, this is without experimental evidence. In addition, St. Amand lists on his web site numerous brand name products and commercially available herbal preparations that should not, theoretically, be used in combination with guafenesin.
Pharmacology
There is little in the medical literature detailing the pharmacology of guafenesin. One animal study suggested that guafenesin could potentiate the effect of aspirin in reducing inflammation.5 The outcome variable reported was rat paw edema induced by subcutaneous injection of a 5% bentonite solution, not a commonly used outcome measure in animal arthritis research. The author did not report on the number of animals used in the experiments, how many times each experiment was repeated, or what statistical analysis was used. No clinically relevant conclusions can be drawn from this work.
A human trial assessing pharmacokinetic effects of guafenesin on paracetamol absorption was based on previous observations published in Czechoslovakia that guafenesin had muscle-relaxing and anxiolytic properties in mice.6 This human study involved seven healthy volunteers who took a single dose of one of three paracetamol-containing preparations: paracetamol and guafenesin; paracetamol, guafenesin, and caffeine; or paracetamol alone. The authors reported that the rate of absorption of paracetamol was increased significantly by a 200 mg combination dose of guafenesin, but not by the 130 mg combination dose of guafenesin with caffeine. This corresponded to the fact that absorption of paracetamol was completed about 20 minutes sooner in the presence of guafenesin, but not when caffeine was present, compared to taking paracetamol alone. Bioavailability of paracetamol was not altered. No published reports are available on the effect of guafenesin on the pharmacokinetics of other analgesics, nor on efficacy of any analgesics.
Currently, in addition to over-the-counter cough and cold preparations, guafenesin commonly is used in equine anesthesia. Intravenous guafenesin in a dose of 100 mg/kg is given during anesthetic induction in horses as an alternative to the use of benzodiazepines.7
Clinical Study
Only one clinical trial has been carried out to assess the efficacy of guafenesin in fibromyalgia. This was reported in abstract form in 1996 and is available for review in its entirety at www.myalgia.com/guaif2.htm.8
This double-blind randomized controlled trial enrolled 40 female subjects with fibromyalgia. Subjects were randomly assigned to receive guafenesin 600 mg or placebo tablets twice daily. Outcome measures included Fibromyalgia Impact Questionnaire score, tender point score, and an assessment of renal tubular function. Subjects were treated for 48 weeks.
Eight patients dropped out of the trial. The intention-to-treat analysis revealed no difference in response between the placebo and guafenesin groups. No subjects rated themselves cured and there was no improvement in FIQ or number of tender points. The authors were unable to confirm the purported mechanism of action for guafenesin, since there was no detectable increase in uric acid or phosphate excretion in those who received guafenesin. Toxicity was not reported.
Adverse Effects
As with other widely available, over the counter products, it is easy for consumers and physicians alike to conclude that guafenesin is safe. However, no systematic study has been performed assessing the safety of treating fibromyalgia with guafenesin, and long-term effects are unknown.
SAM-e: Rationale for Use
In contrast to guafenesin, SAM-e is a physiologic molecule, normally present in cells, with known biologic effects. It acts as a methyl group donor and precursor to endogenous sulfated products, including cartilage proteoglycans.9 These properties have led to its use in the treatment of osteoarthritis, with success in symptom reduction in some clinical trials.9,10
Three decades ago, SAM-e was serendipitously observed to alter mood and it has been studied subsequently as an antidepressant in a limited number of trials.11 Because of the link noted by others between psychological factors and symptoms in fibromyalgia, an Italian group became the first to use SAM-e in a preliminary trial12 and two additional randomized controlled trials have followed. There also has been interest in investigating the use of SAM-e for the treatment of liver disease since, as a glutathione precursor, SAM-e has been shown to attenuate liver injury caused by alcohol in animal models.
Pharmacology
The development of sensitive and specific assays for SAM-e led to the observation that it is normally present in brain tissue. It is now known to be an important methyl donor in numerous methyltransferase reactions, making it somewhat difficult to isolate a pharmacologic action in any given tissue. Nonetheless, SAM-e interacts with catecholamines, fatty acids and phospholipids, proteins, nucleic acids, polysaccharides, and porphyrins. Interestingly, after demethylation to S-adenosyl-L-homocysteine, it can inhibit methylation reactions, and it subsequently can be metabolized to cysteine and glutathione, both intracellular antioxidants.
Limited pharmacologic studies reveal a 90-minute serum half-life after intravenous administration in humans. Intramuscular bioavailability is about 85%, but oral bioavailability is only 1% in rats. Detectable levels of SAM-e can be found in the brain of rats after IM administration and in the cerebrospinal fluid of humans after large daily IV administration. A number of studies have failed to show clear and consistent changes in monoamine metabolism, although clinical trials have suggested that SAM-e is as efficacious as tricyclic antidepressants in the treatment of depression.11
Clinical Studies
Tavoni and colleagues were the first to report on the effects of SAM-e in fibromyalgia patients.12 Twenty-five patients attending their outpatient clinic, who had at least three tender points, were enrolled in a randomized, double-blind crossover protocol. They received either placebo or SAM-e 200 mg IM once daily for 21 days, underwent a two-week washout, and were switched to the other agent for 21 additional days. Outcome measures included the number of trigger points plus painful anatomic areas (an undefined parameter) and administration of questionnaires assessing depression.
Only 17 subjects completed the trial with six leaving for unexplained reasons and two developing injection site abscesses. Eleven of 17 subjects were depressed at baseline. SAM-e treatment was associated with a significant decrease in the number of trigger points plus painful anatomic areas and with a reduction in scores on the depression scales. Interpretation of these results is limited by the small sample size, the number of dropouts, and the confounding effect of depression on pain symptoms and outcome assessment.
Danish investigators sought to establish the degree of efficacy of an oral formulation of SAM-e.13 Subjects were required to have at least four tender points on physical examination for study entry. Participants were randomly assigned to receive placebo or SAM-e 400 mg bid for six weeks and were "encouraged not to use their usual analgetic [sic], anti-inflammatory, or antidepressant drugs concomitantly." However, eight patients used analgesics during the trial, including six who used narcotics. Five patients withdrew during the trial: Three SAM-e-treated subjects withdrew because of gastrointestinal upset and one for dizziness; one placebo-treated subject withdrew because of headache. The investigators found a significant decrease in visual analog scale measurements for resting pain in the last week of the study and fatigue. However, they found no differences in number of tender points, muscle strength, pain during physical activity, quality of sleep, overall well-being, or Beck Depression Index. The authors noted that poor bioavailability may have limited the effects of the oral preparation and that higher doses might be required.
Several years later, the same Danish group published additional results on the use of SAM-e for fibromyalgia, this time with an intravenous preparation.14 Subjects in this study met American College of Rheumatology criteria for the diagnosis of fibromyalgia,1 thus having 11 of 18 tender points. Thirty-four participants were randomized to receive an intravenous injection of either 15 mL of placebo or a solution containing SAM-e 600 mg on the following schedule: daily injection for six days, one day off, daily injection for four days, washout for 11 days, repeat the injection schedule with the other agent. Four actively treated subjects withdrew: three due to gastrointestinal symptoms, one due to anaphylaxis. One placebo-treated subject withdrew because of the travel distance. No statistically significant differences were noted in the number of tender points, the primary outcome measure, nor in severity of fatigue, quality of sleep, morning stiffness, depression assessment scales, or need for rescue medication.
Adverse Effects
The use of injectable SAM-e has been associated with considerable gastrointestinal side effects, including nausea, vomiting, and diarrhea that required hospitalization. Anaphylaxis has been reported after the first injection. The oral preparation also been associated with gastrointestinal side effects severe enough to cause withdrawal from a study, as well as dizziness.
Conclusion
Guafenesin is a readily available, over-the-counter expectorant available in tablet and liquid formulas. It has been promoted for use in fibromyalgia by a practitioner with many years of experience with the medication, but there is little scientific evidence to substantiate its purported mechanism of action or its efficacy. The only trial of use in subjects with fibromyalgia was well-designed and failed to show efficacy.
The rationale for the use of SAM-e in the treatment of fibromyalgia is that benefit might accrue due to neuropsychiatric effects. However, these trials have not demonstrated improvement in either signs or symptoms of fibromyalgia or of depression in fibromyalgia patients. Studies have been inadequately powered to answer the questions posed and appropriate dose-finding studies remain to be carried out. Furthermore, the applicability of the findings to what might be expected in an outpatient population with ready access to oral SAM-e is limited because only one study used an oral preparation. Severe side effects have been reported, including anaphylaxis, nausea, vomiting, and diarrhea requiring hospitalization.
Recommendation
Guafenesin is not recommended for use in patients with fibromyalgia. However, because it is commercially available and its popularity is widespread, treating physicians should be aware that it may be one of many alternative treatments used by fibromyalgia patients. Regular discussion of the use of over-the-counter products with all patients is recommended.
SAM-e is not recommended for use in patients with fibromyalgia. Studies to date do not support its use and side effects may be significant.
Dr. Kolasinski is Assistant Professor of Medicine; Director, Rheumatology Fellowship Program; and Chief of Clinical Service, Division of Rheumatology, University of Pennsylvania School of Medicine in Philadelphia.
References
1. Wolfe F, et al. The American College of Rheumatology 1990 Criteria for the Classification of Fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum 1990;33: 160-172.
2. Clauw D. Fibromyalgia and diffuse pain syndromes. In: Primer on the Rheumatic Diseases. 12th ed. Atlanta, GA: Arthritis Foundation; 2001:188-193.
3. Pioro-Boisset M, et al. Alternative medicine use in fibromyalgia syndrome. Arthritis Care Res 1996;9:13-17.
4. Bengtsson A, Henriksson KG. The muscle in fibromyalgia— a review of Swedish studies. J Rheumatol Suppl 1989;16: 144-149.
5. Marek J. On the non-specific antiinflammatory effects of other-than-antirheumatic drugs. Psychotropic drugs, inflammation and antiinflammatory drugs. Int J Tiss Reac 1985; 7:475-504.
6. Perlik F, et al. The effect of guaiphenesin on absorption and bioavailability of paracetamol from composite analgesic preparations. Int J Clin Pharmacol Ther Toxicol 1988;26: 413-416.
7. Brock N, Hildebrand SV. A comparison of xylazine-diazepam-ketamine and xylazine-guafenesin-ketamine in equine anesthesia. Vet Surg 1990;19:468-474.
8. Bennett R, et al. A one-year double-blind, placebo-controlled study of guafenesin in fibromyalgia. Arthritis Rheum 1996; 39:S212.
9. Di Padova C. S-adenosylmethionine in the treatment of osteo-arthritis. Am J Med 1987;83(5A):60-65.
10. Bradley JD, et al. A randomized, double blind, placebo controlled trial of intravenous loading with S-adenosylmethionine (SAM) followed by oral SAM therapy in patients with knee osteoarthritis. J Rheumatol 1994;21:905-911.
11. Baldessarini RJ. Neuropharmacology of S-adenosyl-L-methionine. Am J Med 1987;83(5A):95-103.
12. Tavoni A, et al. Evaluation of S-adenosylmethionine in primary fibromyalgia. A double-blind crossover study. Am J Med 1987;83(5A):107-110.
13. Jacobsen S, et al. Oral S-adenosylmethionine in primary fibromyalgia. Double-blind clinical evaluation. Scand J Rheumatol 1991;20:294-302.
14. Volkmann H, et al. Double-blind, placebo-controlled cross-over study of intravenous S-adenosyl-L-methionine in patients with fibromyalgia. Scand J Rheumatol 1997;26: 206-211.
Kolasinski SL. Guafenesin and SAM-e for fibromyalgia. Altern Med Alert 2003;6(5):55-59.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
