ECG Review: "Painful" Heart Block
By Ken Grauer, MD
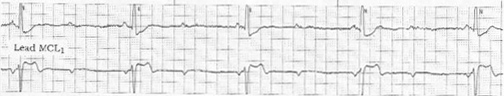
Figure. Simultaneously recorded lead II and lead MCL1 rhythm strip
obtained from a middle-aged man with vomiting and severe pain.
Clinical Scenario: The simultaneously recorded lead II and lead MCL1 rhythm strip shown in the Figure was obtained from a middle-aged man in severe pain from a musculoskeletal disorder. He was not having chest pain, and had no known history of cardiovascular disease. He had an episode of vomiting shortly before this tracing was recorded. Is there evidence of "heart block?" If so, what type? What might you specifically look for on additional telemetry tracings to confirm your diagnosis of the arrhythmia?
Interpretation/Answer: The ventricular rhythm is slow and fairly regular at a rate just under 30 beats/minute. The QRS complex is narrow. P waves are present in both monitoring leads. These P waves are fairly consistent in morphology and upright in lead II. This suggests a sinus mechanism for the underlying rhythm, albeit at a slow and somewhat variable atrial rate. There appear to be two P waves for each QRS complex. However, attention to the PR interval just preceding each QRS complex reveals a constant and normal PR interval duration. This suggests that at least every other P wave is being conducted to the ventricles. The rhythm is therefore 2° AV block with 2:1 AV conduction.
Several points are deserving of mention. First, slight variation in the atrial rate is commonly seen in patients with 2° AV block. This phenomenon is known as a ventriculophasic sinus arrhythmia, which may be related to slight variation in sinus node perfusion caused by the AV block.
The second key point relates to classification of the various types of AV blocks. The mildest form is 1° AV block, in which each sinus impulse is conducted to the ventricles, albeit with some delay (manifested by prolongation of the PR interval to beyond 0.20 second). Complete (ie, 3°) AV block occurs when no sinus impulses are conducted to the ventricles. Since some P waves in the Figure are being conducted while others are not, the rhythm in the Figure must represent some type of 2° AV block. The most common of the three forms of 2° AV block (by far!) is Mobitz type I (ie, AV Wenckebach), which is characterized by progressive lengthening of the PR interval in consecutively conducted beats until an impulse is blocked. Because the defect with Mobitz I tends to occur at a higher level in the conduction system (usually at the AV node), the QRS complex will usually be narrow, the disorder is more likely to reverse with Atropine (which acts primarily on the AV node), and long-term prognosis is generally good. In contrast, Mobitz II 2° AV block is characterized by the presence of consecutively conducted beats with a constant PR interval before sudden non-conduction of one or more sinus impulses. The QRS complex will usually be wide with Mobitz II, reflecting its generally lower (usually ventricular) site of origin. Because of a very high risk of abrupt progression to complete AV block or ventricular standstill, cardiac pacing is recommended for most patients with Mobitz II 2° AV block, whereas pacing will usually not be needed for Mobitz I patients who are hemodynamically stable.
It is important to appreciate that a third type of 2° AV block also exists, in which the presence of 2:1 AV conduction makes distinction between the Mobitz I and Mobitz II forms much more difficult (because consecutively conducted impulses do not occur, one cannot tell if the PR interval is "lengthening" prior to the dropped beats). This is the situation shown in the Figure. Despite persistent 2:1 AV conduction, several factors still favor the less severe (Mobitz I) conduction abnormality in this case. The patient in question has no known history of heart disease. Marked vagal stimulation (from pain or other stimuli) can of itself temporarily depress AV nodal conduction enough (even in normal subjects) to produce varying degrees of AV block, especially Mobitz I. Statistically, Mobitz I is much more common than Mobitz II, especially in patients without underlying heart disease. And finally, the fact that the QRS complex is narrow makes it much more likely that the conduction disturbance is Mobitz I. Attention to other rhythm strips recorded on this patient could confirm our clinical suspicion if clear evidence of Wenckebach conduction was found, since it would be rare indeed for a patient to switch back and forth between Mobitz I and Mobitz II forms of 2° AV block. Adequate treatment of the patient’s pain in this case resulted in swift resolution of the conduction disturbance.
Dr. Grauer, Professor, Assistant Director, Family Practice Residency Program, University of Florida, is Associate Editor of Internal Medicine Alert.
The rhythm strip shown in the Figure was obtained from a middle-aged man in severe pain from a musculoskeletal disorder. He was not having chest pain, and had no known history of cardiovascular disease. He had an episode of vomiting shortly before this tracing was recorded. Is there evidence of heart block? If so, what type?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
