OTC collections boosted with ‘enthusiasm of sports’
Hospital leads 20-facility system in collections
When Peggy O’Neill, admitting director for St. Helena Hospital in Deer Park, CA, began tackling the improvements involved in a major restructuring of the admitting department, she looked first at the bottom line. Very aware of the 18 new workstations, 18 new scanners, and assorted software that had been purchased — not to mention a new FTE (full-time equivalent) structure and additional staff — "the financial side of me" wanted to start paying those bills, O’Neill says.
"It’s not that we didn’t focus on other issues like denials and accuracy — those were moving along — but I wanted to show a return on investment by showing what we could do in over-the-counter [OTC] cash," she adds.
OTC goals met and exceeded
Going into 2002, the department’s upfront collections were averaging less than $5,000 a month, O’Neill reports. She was in the midst of reinventing the hospital’s admitting process, which was extremely decentralized, and some positions were not yet filled, she adds. "I didn’t have a supervisor until July 2002."
O’Neill set — and met — monthly OTC goals of $20,000 for January/February 2002; $30,000 for April/March 2002; $40,000 for April/May 2002; and $50,000 for July/August 2002. "After that, we took [the goal] up to $80,000 per month, which we had exceeded in July, and kept it there the rest of the year," she says. "We went up and down. Plotting out the goal is not an exact science when there is no history to build on."
Part of the process, O’Neill adds, was looking at the payer mix and patient volume in various areas to get a sense of the collection possibilities. And she gives her staff much of the credit for the initiative’s success. "I’m very blessed with a group of people who were committed to this," she says. "I have never been disappointed by them at all. You have to find the right person, and you have to use some tools that make it worth their while."
A couple of years ago, O’Neill notes, she asked the question, "How can we get the enthusiasm of weekend sports and apply it to the work environment?" Much of the answer, she discovered, was based on constant communication, beginning with creating charts on how much each person was collecting and looking at monthly goals and accomplishments. "A history started building, and momentum started building," O’Neill says. "Two-and-a-half years later, it’s so ingrained in this culture that no matter who comes and goes, on average, we exceed $80,000, and some months we’ve hit $138,000."
The figures for 2004 look even better, she notes. As of late June 2004, "we are 10% ahead against our [admitting collections] goal for the year. The first month we [collected] $155,000, and we’ve been averaging $98,000 a month for the first 5½ months." For two years running, O’Neill says, St. Helena has led the 20 hospitals in the Adventist Health system in OTC cash collection.
The right skills and technology
What has helped the collection effort, O’Neill says, is the right mix of skills on the front end, combined with the proactiveness that has been the theme of the entire admitting initiative. "We have two people — one in surgery and one in scheduled outpatients [diagnostics] — who do nothing but pre-registration of people who are coming in," she says. "That wasn’t being done when I got here. I had to convince the team leaders in the diagnostic outpatient area [radiology, cardiology, etc.] to transfer from pen-and-paper scheduling to a homegrown on-line system so the admission staff would have access to the schedule."
The shell of the on-line scheduling system came from software developed by an information systems analyst at a nearby Adventist Hospital, O’Neill notes. "It has any number of applications, but the most useful one is [scheduling]. I learned how to build the system so it could be customized to include the information each department needed."
The potential for customization helped sell the idea to the diagnostics team leaders, O’Neill says. "I said, Tell me what criteria you need, and let’s see if we can put this together.’ We went back and forth a couple of times."
For the women’s center, for example, there were places to indicate the location of the patient’s most recent mammogram films and whether she had breast implants or hip replacements, she adds. Although the need to schedule multiple visits at once has made use of the on-line scheduling system problematic for the physical therapy department, O’Neill notes, "I’m not giving up on it."
Eventually, every area except physical therapy changed over to the on-line scheduling process, she says. "That was the tool I needed to provide information upfront to the pre-registration staff so they could work one or two days out and then pass the patient’s information on to the financial counselor, who can call the insurance company to confirm coverage."
The financial counselor looks up the patient’s deductible or copay, figures out the coinsurance based on the appropriate contract or plan, and then telephones the patient at home to work with them to procure an upfront deposit, O’Neill explains. If copay is due at registration, she puts a note on the account alerting the registrar, she says. If the patient is unable to pay, the financial counselor works out a payment plan, or determines if the person is eligible for MediCal. "We’re not successful with all cases, but there is a dramatic difference from what we were getting before."
The conversation, O’Neill continues, goes something like this: "I see from the notes here that so-and-so spoke with you and that you have a $250 copay today. How would you like to pay for that?"
While some employees felt comfortable right away asking for the payments, she notes, prepared scripts have helped others ease into the practice. Before the pre-registration process was instituted, she says, "the knowledge wasn’t there," and with 110 patients a day, it was difficult to make any serious effort toward collection. Now, O’Neill adds, between 96% and 98% of scheduled accounts are pre-registered.
The pre-registration initiative also has helped reduce patient wait time, she notes. "The information is solid, the verification has been done. The patient just signs the Conditions of Admission and consent form, and we get a copy of the insurance card." If the card has been scanned during an earlier encounter, she adds, "we don’t even have to do that."
While efforts were being made on the personnel side, there were also major changes taking place on the technological side, O’Neill points out. New Advance Beneficiary Notice software alerts staff up front about procedures that might not be covered by Medicare, helping reduce potential denials, she says. And as of a year ago, the hospital has on-line web access through the HDX system to eight or 10 commercial payers, as well as Medicare and MediCal, that tells staff what coverage the patient has and what the copay will be.
New scanning software allows employees to scan insurance cards and physician orders, O’Neill adds.
ACRP program boosts collections
St. Helena is one of the few hospitals in California that offers an inpatient stay for the treatment of chemical dependency, O’Neill says, and the Acute Chemical Rehabilitation Program (ACRP) has been a big contributor to its cash collection totals. A $12,000 payment is due up front if the patient has no insurance coverage. But before the recent OTC effort began, there was no organized approach to collecting or measuring upfront cash, O’Neill explains. "When I started, they were collecting between $70,000 and $90,000 a month."
"Usually, those kinds of programs are a little more lax in getting payment up front, which is deadly with dealing with behavioral health," she points out. "Nine times out of 10, you write it off if you don’t get it up front." If patients have a successful outcome with the program, but then later backslide, O’Neill adds, the attitude may become, "It’s not working for me. I’m not going to pay."
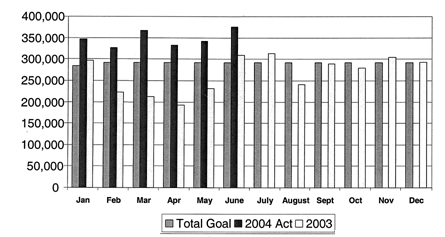
Now, she says, the OTC collections goal for that program is $162,000, and recent monthly totals have been $209,000 and $212,000. The highest monthly total to date for the combined OTC collections of admitting, ACRP, and the Center for Health Transformations, which treats conditions such as eating disorders and nicotine addiction, is $385,000, O’Neill says, which was reached in June 2004. (See chart.)
|
Combined Collection Goals and Actual Totals
|
Successful OTC collection, she notes, requires "a balancing act between looking at programs that are rich [and] can be mined for over the counter upfront cash, and focusing on the $12, $25, and $75 copays in the ED [emergency department]."
Although the ED’s OTC collections total for a weekend might be $700, while that for the Center for Health Transformations is $30,000, they are equally important, O’Neill adds. "If you are promoting teamwork, that $75 in the ED should be looked at in the same way as the larger amount," she says, "because, by and large, the same effort went into it. It’s about each one of the team members contributing, keeping everybody on the same team, and recognizing everybody for the result of that total team effort."
(Editor’s note: In the next issue of Hospital Access Management, look for more details on how O’Neill built a "best-practice" admitting department at St. Helena Hospital.)
When Peggy ONeill, admitting director for St. Helena Hospital in Deer Park, CA, began tackling the improvements involved in a major restructuring of the admitting department, she looked first at the bottom line.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.