B-Complex Vitamins for Depression
B-Complex Vitamins for Depression
October 2001; Volume 4; 112-114
By Barak Gaster, MD
When friends find out how little time is spent learning about diet and nutrition in medical school, they usually are surprised. Patients also come to the clinic with questions about what they should eat and what vitamins they should take, and they may be shocked to find their doctors are not sure what to say.
Among patients suffering from depression, the situation can be more intense. "But what about B-complex vitamins, Doc? I’ve heard that’s all I need to turn me around." Meeting a question like that with a blank stare can put a kink in your therapeutic relationship.
Although depression researchers have been interested in a possible role for B-complex vitamins since the 1960s, few clinical trials have been performed. Thus, although B-vitamin supplementation in patients with depression may be helpful and appears to be safe, there is no good evidence that such treatment is effective.
Mechanism of Action
The B-complex vitamins are a group of sub- stances that must be obtained from the diet. They serve as cofactors for numerous enzymatic pathways in the body. B vitamins have been linked to depression by virtue of their central role in the synthesis of neurotransmitters.1 Specifically, thiamin (B1), riboflavin (B2), pyridoxine (B6), cobalamin (B12), and folate (sometimes referred to as B9) all participate in important steps in the synthetic pathways of norepinephrine, dopamine, and serotonin (see Table).
| Table: The B-complex vitamins | |
| B Vitamins
Implicated in Depression |
Recommended
Intake* Males/Females |
| Thiamin (B1) | 1.2/1.1 mg/d |
| Riboflavin (B2) | 1.3/1.1 mg/d |
| Pyridoxine (B6) | 1.3/1.3 mg/d |
| Cobalamin (B12) | 2.4/2.4 mcg/d |
| Folate (B9) | 0.4/0.4 mg/d |
| B Vitamins Not Implicated in Depression |
|
| Niacin (B3) | 16/14 mg/d |
| Pantothenic acid (B5) | 5/5 mg/d |
|
|
|
| * Higher limits for those 14 years and older to reduce risk of deficiency. | |
| Source: Dietary Reference Intakes 2000: Applications in Dietary Assessment. Washington, DC: National Academy Press; 2000. | |
|
|
|
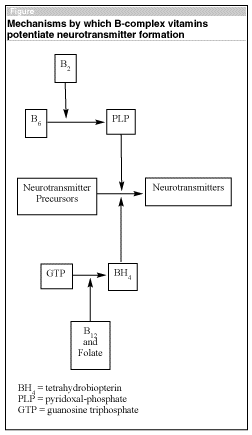
Riboflavin is essential for the biochemical conversion of pyridoxine to pyridoxal-phosphate (PLP) (see Figure). PLP in turn is a co-enzyme for several decarboxylases needed for neurotransmitter synthesis. Cobalamin and folate are required for the formation of tetrahydrobiopterin (BH4), which is a hydroxylase cofactor necessary for serotonin synthesis. Thiamin has less of a clear link to depression, although it plays a role in the formation of another neurotransmitter, acetylcholine.
Pharmacokinetics
All of the B-complex vitamins are water-soluble. They are easily absorbed from the gastrointestinal tract and are metabolized in the liver.
Efficacy Data
Several studies in the 1980s found that up to 30% of patients with depression have vitamin deficiencies, mostly vitamin B12 and folate.2 Studies which used a more accurate test for folate deficiency,3 red blood cell (RBC) folate concentration, have reported lower rates (10-15%).4 Whether the vitamin deficiency is primary or secondary to the depression is open to question; however, depressed patients often have poor nutritional intake.
There has been only one randomized placebo-controlled study of a B vitamin for depression. Godfrey et al randomized 24 patients with major depression and RBC folate levels below 200 mcg/L to 15 mg/d of methylfolate (a precursor to folate) or placebo.5 All patients received standard antidepressants. At six months, there was a significant improvement in the methylfolate patients on a 4-point clinical outcome scale (P < 0.01). There were no significant differences in Hamilton Depression Scale score between the groups, although there was a trend in favor of the methylfolate group.
In a trial of patients with unipolar or bipolar mania being treated with lithium, Coppen randomized patients to 200 mcg of folate per day or to placebo.6 At one year, the patients with unipolar mania who took folate had significantly lower depression scores than those who did not; the patients with bipolar mania who took folate actually had a trend toward worsened depression. The authors did not report aggregate data of the two groups.
Adverse Effects
Even at very high doses, most of the B-complex vitamins that play a role in depression appear to be safe. Reports of neurotoxicity from pyridoxine have involved doses of 1-6 g/d over several weeks,7 although doses as low as 200 mg/d may cause such symptoms as well.8 At very high doses, folate has been reported to cause altered sleep patterns, irritability, nausea, and pruritus.
Drug Interactions
Anticonvulsants and oral contraceptives may lower folate levels.9 Pyridoxine can interfere with levodopa’s anti-Parkinsonian effects.
Formulation
B-complex vitamins are available in virtually all multivitamins in doses that are calibrated to meet 100% of the recommended daily intake. In addition, formulations containing B-complex vitamins alone are available.
Folic acid is available in many different tablet dosages: 0.1, 0.2, 0.4, 0.8, and 1.0 mg. The best dietary sources of folic acid are vegetables, especially green leafy vegetables, potatoes, cereal products, fruits, and organ meats (e.g., liver, kidney). Methylfolate is not commercially available in the United States.
Dosage
Given the lack of clinical trial data, no clear dosing recommendations can be made for B-complex vitamins for depression beyond the recommended daily intakes listed in Table 1.
Conclusion
Although there are theoretical reasons to think that B-complex deficiency may play a role in depression, the evidence supporting the efficacy of vitamin supplementation in the treatment of depression is lacking. There is no evidence to suggest that supplementation within the range of recommended daily intakes is harmful; however, there are at least theoretical reasons to believe that it may be helpful.
Recommendation
Given that vitamins are safe, reliably regulated in the United States, and relatively inexpensive, it is reasonable to advise patients with depression to take one or two multivitamins per day that include B-complexes. However, patients should be advised that this should be adjunctive treatment only, and should not be the sole therapy they get for their depression.
Providers should consider checking B12 and RBC folate levels in patients who are depressed and have poor diets and then treat any specific deficiencies that are found. Advise patients to steer clear of expensive, mega-dose formulations of vitamins for the treatment of depression; there is no evidence to suggest that such therapies are effective.
References
1. Petrie WM, Ban TA. Vitamins in psychiatry. Do they have a role? Drugs 1985;30:58-65.
2. Alpert JE, Fava M. Nutrition and depression: The role of folate. Nutr Rev 1997;55:145-149.
3. Abou-Saleh MT, Coppen A. Serum and red blood cell folate in depression. Acta Psychiatr Scand 1989;80: 78-82.
4. Bottiglieri T. Folate, vitamin B12, and neuropsychiatric disorders. Nutr Rev 1996;54:382-390.
5. Godfrey PS, et al. Enhancement of recovery from psychiatric illness by methylfolate. Lancet 1990;336: 392-395.
6. Coppen A, et al. Folic acid enhances lithium prophylaxis. J Affect Disord 1986;10:9-13.
7. Clinician Fact Sheet: The B vitamins, Part III. Altern Med Alert 2001:4(4):S1-2.
8. Parry GJ, Bredesen DE. Sensory neuropathy with low-dose pyridoxine. Neurology 1985;35:1466-1468.
9. Schumann K. Interactions between drugs and vitamins at advanced age. Int J Vitam Nutr Res 1999;69: 173-178.
October 2001; Volume 4; 112-114
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.