ECG Review: A ‘Sited’ Tachycardia
ECG Review: A Sited’ Tachycardia
By Ken Grauer, MD
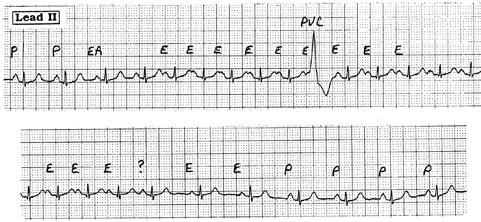 |
Figure. Telemetry rhythm strips showing
the onset and resolution
of this patient’s tachycardia.
Clinical Scenario: The tachycardia shown in the Figure was obtained from an older woman who presented with shortness of breath and a recent history of "irregular heart beat" episodes. The top strip shows the onset of one such episode, and the bottom strip shows its resolution. What is the probable mechanism of this patient’s arrhythmia? Is the premature ventricular contraction (PVC) seen in the top strip supportive of this diagnosis? How might you treat this patient’s rhythm disorder?
Interpretation: The underlying rhythm is sinus, as suggested by the two normal beats that initiate the top tracing. P wave morphology changes with the third beat, which most likely arises from an ectopic atrial site (EA). Acceleration of the rhythm follows, with development of a tachycardia that manifests an upright but different (ectopic) appearing P wave (E) compared to the sinus-conducted beats. The rate of the tachycardia is approximately 135 beats/minute, and the occurrence of the PVC does nothing to terminate the episode. Gradual slowing is seen in the bottom strip, with conversion of P wave morphology back to the sinus-initiated (P) focus.
The features described and illustrated in the above tracings are characteristic of an ectopic atrial tachycardia (gradual onset and offset of the rhythm with ectopic P wave morphology). Unlike the overwhelming majority of supraventricular tachycardia (SVT) rhythms in adults that are AV-nodal "dependent," ectopic atrial tachycardia arises from an ectopic atrial site that gradually accelerates and is independent of the AV node for its continuation. As a result, neither PVCs nor vagal maneuvers are likely to terminate the rhythm. Treatment consists of correcting the underlying cause (most likely heart failure, pulmonary disease, electrolyte disturbance, or digitalis toxicity); AV nodal-blocking drugs (for rate control); and occasionally, antiarrhythmic agents (to suppress the ectopic atrial site), though the response to such treatment is highly variable.
Dr. Grauer, Professor and Assistant Director, Family Practice Residency Program, University of Florida, ACLS Affiliate Faculty for Florida, Gainesville, FL, is on the Editorial Board of Emergency Medicine Alert.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
