Special Feature: Knee Extensor Mechanism Disruptions
Knee Extensor Mechanism Disruptions
By William J. Brady, MD
|
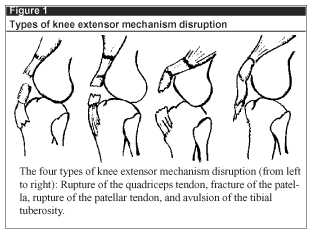
The extensor mechanism disruptions include rupture of the quadriceps tendon, patellar fracture, patellar tendon rupture, and tendon avulsion at the tibial tubercle;1-4 the most commonly encountered form of disruption involves rupture of the patellar tendon. (See Figure 1.) Extensor mechanism disruption generally occurs as the result of the quadriceps muscle suddenly contracting forcefully against a slightly flexed knee; in fact, biomechanical study has shown that when the knee is slightly flexed the forces across the patellar tendon are maximal. Direct trauma to either the patella or the proximal tibia also may result in extensor mechanism disruption, usually involving a patellar fracture or avulsion of the patellar tendon. Misdiagnosis by the primary care provider has been reported to be as high as 40%. Accurate early diagnosis is essential to ensure the best outcome with early surgical repair and intensive physical therapy.
 |
Quadriceps tendon rupture is more common in patients with systemic disease, such as chronic renal failure, gout, hyperparathyroidism, diabetes mellitus, and obesity; also, patients with degenerative arthritic changes in the knee are susceptible. Patellar tendon injuries in these patient groups are less common; in general, these patients tend to be younger and less likely to have degenerative disease or systemic illness. Bilateral patellar tendon rupture has been reported and is associated with systemic lupus erythematosus and rheumatoid arthritis.2 Extensor mechanism disruption has been reported as an unusual complication of Paget’s disease; the patellar tendon usually is avulsed from the tibial tubercle in the region of pagetic bone. In other instances, rupture of the tendon often occurs through a pathologic area of the tendon; in fact, several studies have implicated steroid injections and microscopic damage to the tendon’s vascular supply as a cause of failure.5 Ongoing or recent treatment with fluoroquinolone antibiotics also has been associated with tendinopathy and tendon rupture, including the quadriceps tendon.6
Clinical Presentation and Diagnostic Approach
The clinical presentation of an extensor mechanism disruption generally includes the complaint of acute onset of knee pain with loss of function. The history includes either stumbling or jumping followed by sudden buckling of the knee and extreme pain. The patient usually describes a history with the common theme of forceful axial loading on a partially flexed knee; the inability to extend the knee results in the loss of function. Further, a careful medical history is essential to alert the examiner to associated systemic illnesses. Physical examination may reveal a palpable defect in the quadriceps or patellar tendon. The position of the patella should be assessed. Quadriceps tendon ruptures will present with inferior displacement of the patella (patella baja), proximal ecchymosis, and swelling. Proximal patellar displacement (patella alta), inferior pole tenderness, and swelling indicate patellar tendon rupture. Evaluation of range of motion will reveal markedly depressed active extension at the knee, inability to maintain passive extension against gravity, or complete loss of knee extension. Patients with partial ruptures may have active extension, but it will be markedly weakened.3,4 Hematoma or hemarthrosis may mask the clinical signs discussed above. In most cases, the diagnosis is made with the inability to extend the knee in the setting of the appropriate mechanism.
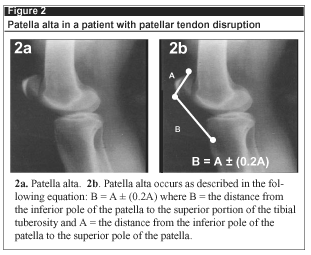
Radiographic findings in patients with quadriceps tendon rupture include inferior patellar displacement (patella baja), superior pole boney avulsion fragment, and degenerative spurring of the patella seen on the tangential view (tooth sign). Complete disruption of the patellar tendon will be indicated by superior displacement of the patella and inferior boney avulsion fragment. (See Figure 2.) Comparison views may be necessary to diagnose subtle patellar displacement. In cases involving bony injury, either patellar fracture or avulsed bone fragment will be seen on the radiograph. In many cases, the radiograph may be entirely normal; such a finding should not dissuade the clinician from the correct diagnosis.
 |
Additional radiographic imaging may be required, usually after referral to the orthopedic surgeon. The quadriceps and patellar tendons are easily visualized using magnetic resonance imaging. Partial tears and tendinosis may be difficult to diagnosis, but complete tears are easily visualized. Patellar fractures, bone bruises, and avulsion of the tibial tubercle are revealed as changes in marrow signal intensity. MR imaging also is extremely useful in identifying associated meniscal tears and chondromalacia patella. Ultrasound and computed tomography (CT) also have been used to evaluate continuity of the extensor mechanism.5
Treatment
Accurate diagnosis of partial or complete patellar tendon ruptures, avulsion fractures of the patella or tibial tubercle, and complete quadriceps tendon tears is essential because best results are obtained with early surgical repair. The primary treatment issue for the emergency physician is accurate diagnosis and timely orthopedic referral. Orthopedic consultation should occur either at the time of injury or within 24 hours of presentation. Knee immobilization with crutch walking should be advised until orthopedic follow-up is accomplished. Ultimate repair involves surgery in most cases.7 The delay in treatment of a quadriceps tendon tear for 4-6 weeks may result in the tendon being difficult to mobilize. Patients with patellar tendon ruptures that have gone undetected for more than two or more weeks may develop significant proximal retraction of the patella with quadriceps contracture and adhesion.
Most surgical repair techniques are followed by immobilization in a long leg cast in extension for four to six weeks with partial weight bearing using crutches. Intensive physical therapy is prescribed beginning with active flexion and passive extension exercises. Strengthening exercises are advanced as knee flexion returns. Patients return to sporting activities in four to six months, when knee flexion is at least 120° with strength deficits less than 10%.7
Dr. Brady, Associate Professor of Emergency Medicine and Internal Medicine, Residency Director and Vice Chair, Emergency Medicine, University of Virginia, Charlottesville, is on the Editorial Board of Emergency Medicine Alert.
References
1. Naver L, Aalberg JR. Rupture of the quadriceps tendon following dislocation of the patella: Case report. Am J Bone Joint Surg 1985;67:324-325.
2. Nabors ED, Kremchek TE. Bilateral rupture of the extensor mechanism of the knee in healthy adults. Orthoped 1995;18: 477-479.
3. Cooper ME, Selesnick FH. Partial rupture of the distal insertion of the patellar tendon. A report of two cases in professional athletes. Am J Sports Med 2000;28:402-406.
4. Jeffery JA, Podmore M. Unusual avulsions of the patella tendon in two schoolboy athletes: Case reports and discussion with reference to the literature. Injury 1995;26:126-128.
5. Khan KM, et al. Patellar tendinosis (jumper’s knee): Findings at histopathologic examination, US, and MR imaging. Victorian Institute of Sport Tendon Study Group. Radiol 1996;200:821-827.
6. Harrell RM. Fluoroquinolone-induced tendonopathy: What do we know? South Med J 1998;92:622-625.
7. Panni AS, et al. Patellar tendinopathy in athletes. Outcome of nonoperative and operative management. Am J Sports Med 2000;28:392-397.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
