Abstract & Commentary: Detecting Airflow Obstruction in the Mechanically Ventilated Patient
Abstract & Commentary
Detecting Airflow Obstruction in the Mechanically Ventilated Patient
By David J. Pierson, MD, Editor, Professor Emeritus, Pulmonary and Critical Care Medicine, University of Washington, Seattle, is Editor for Critical Care Alert.
Synopsis: Examination of expiratory flow-volume tracings obtained from passively ventilated patients during manual compression of the abdomen showed a pattern ascribed to expiratory flow limitation in those with a history of COPD or asthma, and also in obese patients.
Source: Lemyze M, et al. Manual compression of the abdomen to assess expiratory flow limitation during mechanical ventilation. J Crit Care 2011;Jul 26. [Epub ahead of print.]
Lemyze and colleagues studied a simple bedside procedure for detecting expiratory airflow obstruction in intubated, mechanically ventilated patients. They recorded inspiratory and expiratory flow tracings on the ventilator's digital monitor screen with and without pressing manually on the patient's abdomen throughout expiration. They reasoned that expiration in patients who had no expiratory airflow limitation would be augmented throughout the expiratory phase, whereas the flow tracings in obstructed patients (as in severe chronic obstructive pulmonary disease [COPD] or asthma) would demonstrate a different pattern and not show increased flow throughout the whole exhalation. They tested this in a series of ventilated patients with and without previously known obstructive lung disease.
The patients were studied during controlled mechanical ventilation (sedated; no triggering), with simultaneous recording of expiratory waveforms and measurement of esophageal pressures via gastric balloon. Separately, the first 13 patients also had expiratory waveforms recorded with 5 cm H2O continuous negative airway pressure, using a technique for detecting airflow limitation during mechanical ventilation described by Valta et al in 1994.1 The authors studied 44 patients (28 men; mean age 56 years) in a medical ICU who had been ventilated for a mean of 4.7 days (primary causes for respiratory failure not given). Seventeen patients were diagnosed with COPD (defined according to GOLD criteria; severity of obstruction by forced expiratory volume in the first second [FEV1] not given), and three carried a diagnosis of asthma. The other patients were not known to have underlying airway disease.
Using the authors' technique, expiratory flow limitation was detected during abdominal compression in 31 of 44 patients, or 70%. This included all 20 patients with a clinical history of obstructive lung disease, plus 11 others, 10 of whom were obese and several of whom were elderly. Of the first 13 patients studied, in whom airflow limitation was assessed by both abdominal compression and negative expiratory pressure, seven demonstrated such limitation, with complete agreement by both techniques. There was good correlation between the presence of the obstruction pattern and the detection of auto-PEEP. The authors conclude that manual compression of the abdomen during exhalation, with examination of the expiratory waveform on the ventilator's monitor, "provides a simple, rapid, and safe bedside reliable maneuver to detect and quantify expiratory flow limitation during mechanical ventilation." They hypothesize that the apparent airflow obstruction in the 25% of their patients who were not known to have airway disease may have been due to obesity (airway closure from ventilation at low lung volumes), airway edema (from excessive fluid administration), or advanced age.
Commentary
Methodologically, this study has several important shortcomings that affect the confidence with which their recommendations can be accepted. Chief among these is the lack of validation of the new technique with accepted measurements of airflow obstruction in the patients studied. The authors used a previously reported technique, the application of negative airway pressure during expiration, as their "gold standard" to confirm that obstruction was present, but used it in only 13 of the 44 patients studied. In validating the negative-pressure technique, Valta et al had correlated its results with spirometric measurements in the obstructed patients in their study.1 The absence of FEV1 data or other confirmation of the diagnosis of obstructive lung disease, as well as the apparent presence of airflow limitation in patients without known airway disease, diminishes the confidence with which the present study's conclusions can be accepted. In addition, because the patients were sedated and not interacting with the ventilator, whether this technique might be useful in spontaneously triggering patients or those on spontaneous modes such as pressure support will require further study.
The above cautions notwithstanding, this paper highlights a clinically important issue in the management of mechanically ventilated patients. Obstructive lung disease is very common in all adult ICU populations, and predisposes patients to potentially life-threatening complications during mechanical ventilation if not detected and appropriately managed. Patients with severe underlying COPD, especially, are particularly vulnerable to air trapping, dynamic hyperinflation, and auto-PEEP during positive-pressure ventilation, which if undetected may lead to diminished venous return, hypotension, and pulseless electrical activity, as well as to alveolar rupture and clinical barotrauma. In addition, the presence of dynamic hyperinflation exacerbates patient-ventilator asynchrony and is one of the most common reasons for unsuccessful attempts at weaning.2
Despite multiple clinical practice guidelines and the ready availability of the means of assessment, the diagnosis and staging of COPD are notoriously inaccurate.3 Cigarette smokers who are middle-aged or elderly have a high prevalence of COPD, but the proportion of them who have it is still considerably less than 50%. Only measurements of vital capacity and FEV1 can confirm the diagnosis in patients with chronic respiratory symptoms and an appropriate exposure history. However, studies have shown that the majority of patients who carry a diagnosis of COPD have never had pulmonary function tests. Conversely, studies of medical patients hospitalized for other reasons have shown that the prevalence of undiagnosed COPD in such individuals is high.3 Thus, both because of its clinical importance during mechanical ventilation and the unavailability of accurate diagnostic information in many patients, accurate detection of airflow obstruction in all ventilated patients is a problem of great practical importance.
Current ICU ventilators incorporate automated assessment of auto-PEEP, although the measurement must be initiated each time by the clinician and it cannot be carried out meaningfully if the patient is actively making either inspiratory or expiratory efforts. Although it is not a quantitative measurement, the presence of auto-PEEP can be detected at the bedside via the ventilator's graphics display.4 The figure (see below) illustrates schematically both the abdominal compression technique for detecting airflow obstruction, as used by Lemyze et al in this study, and the detection of dynamic hyperinflation utilizing the ventilator's expiratory waveform.
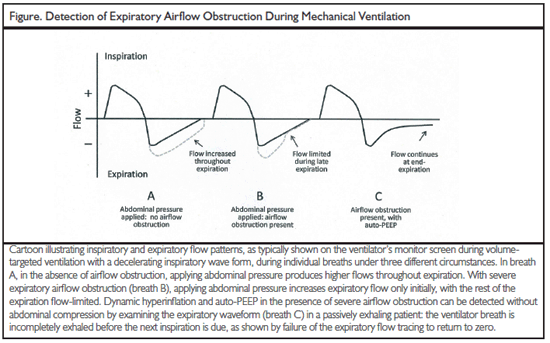
In ventilated patients with severe asthma, significant airway obstruction can often be detected during the inspiratory phase by an increased difference between peak and plateau pressures, the former reflecting decreased airway caliber and the latter the degree of air trapping. Changes in both peak-minus-plateau pressure difference and the auto-PEEP level can be used as indicators of the effectiveness of bronchodilator therapy in the management of acute severe asthma. Auto-PEEP is the most direct monitor of dynamic hyperinflation in COPD. Because airway obstruction in COPD is primarily expiratory, the inspiratory peak-minus-plateau airway pressure difference is a less useful monitor in that condition than in asthma.
References
- Valta P, et al. Detection of expiratory flow limitation during mechanical ventilation. Am J Respir Crit Care Med 1994;150:1311-1317.
- Pierson DJ. Patient-ventilator interaction: Conference summary. Respir Care 2011;56:214-228.
- Pierson DJ. Translating evidence into practice. Respir Care 2009;54:1386-1401.
- de Wit M. Monitoring of patient-ventilator interaction at the bedside. Respir Care 2011;56:61-72.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
