Clinical Briefs With Comments from Russell H. Greenfield, MD
Clinical Briefs
With Comments from Russell H. Greenfield, MD, Dr. Greenfield is Medical Director, Carolinas Integrative Health, Carolinas HealthCare System, Charlotte, NC, and Clinical Assistant Professor, School of Medicine, University of North Carolina, Chapel Hill, NC.
Gut Reaction:Curcumin and Colorectal Cancer
Source: Wang X, et al. Curcumin inhibits neurotensin-mediated interleukin-8 production and migration of HCT116 human colon cancer cells. Clin Cancer Res 2006;12:5346-5355.
Goal: To determine the effect of neurotensin on cytokine/chemokine gene expression and cell migration in human cancer cells, and then to assess the effect of curcumin on neurotensin-mediated processes.
Study Design: In vitro cell study.
Subjects: Human colon cancer cell lines.
Methods: Cells were treated with neurotensin, with and without curcumin, then IL-8 expression and protein secretion were measured, and signaling pathways assessed. The effect of curcumin on neurotensin-mediated processes was also assessed.
Results: Neurotensin, acting through the presence of high-affinity neurotensin receptors, stimulated signaling pathways and induced IL-8 production in a dose-dependent manner. Cell migration was induced as well, likely as a result of IL-8. Curcumin, however, inhibited IL-8 induction and protein secretion. Curcumin also blocked neurotensin-induced cell migration.
Conclusion: Neurotensin selectively stimulates IL-8 gene expression in human colon cancer cells that possess high-affinity neurotensin receptors. IL-8 acts as a pro-invasive factor, increasing cell migration. Curcumin inhibits neurotensin-induced IL-8 production, as well as migration of specific human colon cancer cells.
Study strength: Use of exacting methodology.
Study weakness: Requires in vivo testing to ensure results have clinical applicability.
Of note: Cytokines and chemokines are being increasingly recognized for the roles they play locally in metastatic spread and invasion associated with a number of cancer types; chemokines (like IL-8) are chemotactic cytokines (they attract white blood cells to areas where they might be needed); IL-8 possesses inflammatory potential but also appears to affect cancer progression, leading some to call IL-8 a growth factor that correlates with the metastatic potential of certain cancers; analogous to breast and prostate cancers, certain gastrointestinal and pancreatic cancers possess receptors for gut hormones, and these gut hormones can affect tumor growth; neurotensin stimulates gut motility and secretion, as well as normal cell growth, but also stimulates proliferation of human colorectal and pancreatic cancers that possess high-affinity neurotensin receptors; neurotensin stimulates a variety of signal transduction pathways, resulting in the activation of various transcription factors that can alter expression of tumor-promoting genes.
We knew that: Curcumin is isolated from the plant turmeric (Curcuma longa); neurotensin is a gut hormone primarily found in the small intestine and released in association with fat ingestion; high-affinity neurotensin receptors are found in most colorectal and pancreatic cancers and in some prostate cancers.
Comments: This is a tough article to get through, but the results are compelling, albeit in vitro data. Not only do the researchers show how a gut hormone might impact tumorigenesis and spread, they were also able to show how a natural spice might curb those same effects. Curcumin might be beneficial in both treatment and prevention of colon cancer making curry dishes all the more attractive. Lost in the analysis might be the fact that a gut hormone (neurotensin) released in response to fat ingestion might increase tumor growth and spread through production of specific chemokines. Although curcumin, or its parent plant turmeric, may have preventive or therapeutic benefits in the setting of colon cancer, the Western-style diet clearly plays a role in development of the disease.
What to do with this article: Keep a hard copy in your file cabinet.
Popeye Was Right! Olive Oil (Oyl?) and the Heart
Source: Covas MI, et al. The effect of polyphenols in olive oil on heart disease risk factors: A randomized trial. Ann Intern Med 2006;145:333-341.
Goal: To determine whether heart health benefits ascribed to olive oil (OO) are due in part to polyphenol content, above and beyond monounsaturated fat content, by assessing the impact of sustained daily administration of OO.
Study design: Randomized, crossover, controlled clinical trial.
Subjects: Two hundred healthy male volunteers (aged 20-60 years) from six research centers in five European countries.
Methods: Volunteers were recruited via local advertisements and screened for physiologic or laboratory abnormalities (only those with results within normal reference ranges were accepted). Subjects were randomly assigned to one of three sequences (three weeks duration preceded by a two-week washout period) of 25 mL daily OO administration using high-, medium- or low-polyphenol content OO products. Subjects were asked to maintain three-day dietary records at baseline and after each intervention period. Urinary phenol content was measured before and after each intervention period. Lipid levels, glucose, and biomarkers of antioxidant status (endogenous and exogenous) and oxidative damage were also determined at baseline, and before and after each intervention.
Results: Urinary phenol content increased in a dose-dependent manner with the phenol content of the various OOs ingested. All three interventions increased HDL levels, and lowered both the TC:HDL ratio and triglyceride levels. Intake of both medium- and high-polyphenol OO decreased the LDL:HDL ratio. Indeed, HDL levels increased and TC:HDL ratios decreased linearly with increasing polyphenol content of OO ingested. A linear decrease was also noted for oxidative markers in association with increasing phenolic content of OOs. Circulating oxidized LDL decreased after ingestion of the high-polyphenol content OO. Daily consumption of OO did not impact function of endogenous antioxidant enzymes, something noted in some prior studies.
Conclusion: Daily intake of 25 mL of any one of three types of OO used in this study improved lipid profiles, enhanced antioxidant status, and decreased antioxidant damage to lipids. Benefits increased linearly with increasing polyphenol content of the OO. These results point to an independent cardiovascular health benefit from the polyphenols in OO. Thus, OO is more than simply a source of monounsaturated fatty acids.
Study strengths: Good adherence to protocol (as reflected by changes in urinary phenol content); only a 9% dropout rate; crossover design.
Study weaknesses: Results not easily generalizable (only healthy European males involved); self-reporting of dietary intake; cannot exclude impact of other unreported dietary factors; short duration.
Of note: Women were excluded from the trial due to possible interference from estrogens (potential antioxidants); subjects were asked to avoid high intake of foods high in antioxidant potential during the trial; virgin OOs produced by centrifugation or direct-press methods possess significantly higher phenolic content (phenolic compounds are often lost in the refinement process); OO products were specially prepared for this trial, with the only differences between products being polyphenol content; a nutritionist helped subjects replace oils commonly used in the diet with the specially prepared OOs; study participants were nonsmokers and could not be using antioxidants or aspirin; physical activity was determined at baseline and at the end of each intervention; in cohort studies, a 1 mg/dL increase in HDL has been tied to a 2-3% decrease in risk of heart disease; it is important to note that changes in biomarkers were modest at best.
We knew that: Low-carbohydrate, high-fat diets typically raise HDL levels; OO is rich in oleic acid, a mono-unsaturated fatty acid to which most of the heart health benefits of OO have previously been ascribed; polyphenols reportedly possess antioxidant and anti-inflammatory actions, and have a positive impact on endothelial dysfunction and lipid profiles; oxidation of LDL cholesterol leads to changes that promote atherosclerosis; polyphenol intake has been associated with low rates of cancer and heart disease mortality; increases in HDL have been found with significant intake of other high-poly-phenol content agents, like cocoa and green tea.
Comments: Although the effects noted were modest, the information provided by this article reinforces the potential importance of the Mediterranean-style diet in promoting cardiovascular health. Extra, Extra! The data also underscore a potential added health benefit from extra virgin OO because of its polyphenol content as compared to other high monounsaturated oils. So "mangia," and be well.
What to do with this article: Keep a hard copy in your file cabinet.
D Better It Is: D2 or D3?
Source: Houghton LA, et al. The case against ergocalciferol (vitamin D2) as a vitamin supplement. Am J Clin Nutr 2006;84:694-697.
Goal: To review the data comparing benefits of vitamin D3 (cholecalciferol) and vitamin D2 (ergocalciferol) for supplementation or fortification.
Study design: Review of biochemistry of vitamin D and research pertaining to forms of vitamin D.
Conclusion: Vitamin D3 has greater bioefficacy and should be considered superior to vitamin D2 for supplementation and fortification.
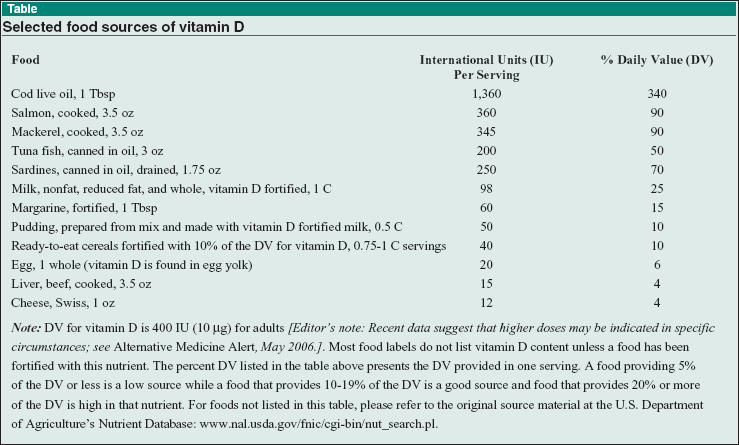
Of note: The best clinical test for assessing vitamin D status is a 25-hydroxyvitamin D level [25(OH)D], which can be used to determine response to vitamin D supplementation, but the active form of vitamin D in the body is 1,25-dihydroxyvitamin D (also called calcitriol, 1-25-dihydroxycholecalciferol, and 1,25-(OH)2D3); physicians have typically considered vitamins D2 and D3 to be bioequivalent and interchangeable; sun exposure and fish intake (see Table below for food sources) provide vitamin D in the form of D3; vitamin D2 was first produced in the 1920s and is plant-derived; researchers initially found it difficult to distinguish between the biological value of the two forms, and the World Health Organization made no distinction between them in their 1949 recommendations; in the 1950s, preparations of D3 were found to be about four times as potent as formulations of D2; interestingly, studies show that D2 is more effective in rats, while D3 is markedly more effective in monkeys and birds (species differ in the relative binding affinity of vitamin D and its metabolites to plasma vitamin D binding protein); in humans, D3 raises 25(OH)D levels almost twice as effectively as D2; as well as being less bioactive, D2 may also be less stable than D3, such that the actual content of vitamin D in a bottle may differ significantly from label claims.
 |
We knew that: The majority of prescription vitamin D comes in the form of D2, while an increasing number of supplements are being reformulated to contain D3; the widespread practice of adding D2 to milk essentially eliminated rickets in the United States and Europe during the 1930s; human studies assessing effectiveness of vitamin D supplementation can be complicated by differences in degree of sun exposure; D2 and D3 do not follow the same metabolic pathway, and thus lead to production of unique biologically active metabolites; D2 administration produces appreciable amounts of 25(OH)D2 which has less affinity for vitamin D binding protein, resulting in a shorter circulating half-life; some human trials using D2 have shown benefits with respect to results of dual-energy X-ray absorptiometry (DEXA) and rate of falls, while others have shown no benefit; all successful fracture prevention trials of vitamin D have used D3.
Comments: Never before has a "review of a review" made its way into the pages of Alternative Medicine Alert, but with increasing emphasis on adequate intake of vitamin D (to help prevent osteoporosis, some cancers, perhaps multiple sclerosis, and to treat pain associated with hypovitaminosis D), as well as the plethora of available supplements containing vitamin D, this article is important. Vitamins D2 and D3 are not bioequivalent as previously believed, but in high enough dosages vitamin D2 can be effective (for example, data suggest that 50,000 IU D2 is equivalent to 15,000 IU D3). Simply stated, it is inefficient to use D2 over D3, and many supplements, as well as prescriptions, contain vitamin D2. Although there appears to be no harm in using vitamin D2 (ergocalciferol), our patients are better served by our prescribing and recommending supplements containing vitamin D3 (cholecalciferol).
What to do with this article: Keep a hard copy in your file cabinet.
Pomegranates Messy? A Brief Report
Source: Sorokin AV, et al. Rhabdomyolysis associated with pomegranate juice consumption. Am J Cardiol 2006;98:705-706. Epub 2006 Jul 14.
Design: Case report.
Subject: Forty-eight-year-old male with dyslipidemia and a possible underlying myopathy.
Scenario: The gentleman in question had been using ezetimibe (Zetia®) daily and rosuvastatin (Crestor®) every other day for 17 months without significant difficulty for familial hypercholesterolemia when he began drinking 200 mL of pomegranate juice twice a week. Three weeks later he presented with significant thigh pain and brown urine, and was found to have a markedly elevated serum creatinine phosphokinase (CPK) level of 138,030 U/L (normal < 200 U/L). Kidney function was normal.
Conclusion: Pomegranate juice may increase the risk of muscle breakdown in association with the use of statin drugs.
Of note: The patient may have had an underlying myopathy (his CPK levels prior to and during treatment for dyslipidemia were moderately and consistently elevated, but below 800 U/L); previously, the patient had not been able to tolerate atorvastatin (Lipitor®) therapy (muscle pain), but was doing well on the regimen noted above; pomegranate juice can inhibit hepatic CYP 3A4 activity; intestinal CYP 3A4 inhibition may promote increased drug absorption and, thereby, higher plasma levels.
We knew that: Hepatic CYP 3A4 is a major metabolic pathway for many medications; grapefruit juice is an inhibitor of CYP 3A4 and has been associated with rhabdomyolysis during statin therapy.
Comments: In the August 2006 issue of Alternative Medicine Alert, a review of an article on pomegranate juice for the treatment of prostate cancer was offered. The data presented were exciting and remain so. We are compelled to make our readers aware of this recent case report not to dissuade anyone from employing pomegranate juice, but to emphasize the importance of individualization of therapy. The patient in question appears to have had an underlying condition that may have predisposed him to rhabdomyolysis, and even the authors themselves state they cannot definitely ascribe the complication directly to the intake of pomegranate juice. In addition, rosuvastatin appears to be metabolized through pathways other than CYP 3A4. Pomegranate juice may well prove to be of great therapeutic benefit, but an understanding of circumstances requiring cautious employ is worthwhile.
What to do with this article: Remember that you read the abstract.
Greenfield RH. Gut reaction: Curcumin and colorectal cancer. Altern Med Alert 2006;9(12):140-142. Greenfield RH. Popeye was right! Olive oil (Oyl?) and the heart. Altern Med Alert 2006;9(12):142-143. Greenfield RH. D better it is: D2 or D3? Altern Med Alert 2006;9(12):143-144. Greenfield RH. Pomegranates Mess? A brief report. Altern Med Alert 2006;9(12):144.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
