An ‘Ounce of Prevention’ May Keep Off Pounds
By Ellen Feldman, MD
Altru Health System, Grand Forks, ND
Dr. Feldman reports no financial relationships relevant to this field of study.
SYNOPSIS: Specific self-regulation techniques are shown to be effective at preventing weight gain in young adults.
SOURCE: Wing R, Tate DF, Espeland MA, et al. Innovative self-regulation strategies to reduce weight gain in young adults: The Study of Novel Approaches to Weight Gain Prevention (SNAP) randomized clinical trial. JAMA Intern Med 2016;176:755-762.
SUMMARY POINTS
- This is a longitudinal study looking at prevention of weight gain in young adults.
- The authors randomly sorted 599 participants into three groups: control; self-regulation and small daily changes in diet and exercise; and self-regulation and large, periodic changes in diet and exercise.
- Self-regulation included daily self-weighing, submission of results via email or text, and receipt of specific recommendations to change eating patterns or exercise with variation in weight.
- “Small-change” group focused on diet and exercise changes of about 100 kcal/day while “large-change” group incorporated a robust initial weight loss and a more substantial increase in activity level.
- Results after three years showed the “large-change” group had the most success in reducing mean weight gain (vs. control and vs. small-change group) and that both large- and small-change self-regulation groups were more effective at reducing mean weight gain than control.
Although unhealthy weight gain may occur throughout one’s lifespan, the greatest incidence of weight gain happens during young adulthood, with an average weight gain of 1 kg/year.1,2 The Study of Novel Approaches to Weight Gain Prevention (SNAP), funded by The National Heart, Lung, and Blood Institute, was designed to investigate the effectiveness of new approaches to weight gain prevention during this high-risk period.3 In explaining the thinking behind the study design, Wing et al noted that self-regulation has been a proven successful strategy when looking at prevention of weight regain after weight loss in adults. It was not a long stretch to hypothesize that these same techniques may help prevent primary weight gain in young adults.
Self-regulation is a core intervention in this study but not necessarily a commonly understood concept. The behavioral model of self-regulation developed in the late 1900s by Howard Leventhal and colleagues and since refined is based on a feedback loop. Components include identification of a specific goal (self-monitoring), a concrete method to measure progress or deviation from the goal (self-evaluation), and corrective responses.4
The SNAP study was designed as a randomized, clinical trial with three arms: a control group and two distinct active intervention groups with specific strategies to monitor and control weight gain. Each of the active groups employed a self-monitoring technique (weighing) but then were instructed in different self-regulation methods: one with small, daily changes known as the “small-change group” and the other with more substantial intermittent interventions known as the “large-change” group.
Adults 18-35 years of age were recruited via mass mailing and emails targeting persons who were concerned about the prospect of weight gain. Among other criteria for inclusion in the study was a body mass index (BMI) between 21-30.9 kg/m2; at baseline just over half of the participants had BMI > 25.0 kg/m2, putting them in the “overweight’ category.
Although the aim was to include at least 25% males in the study, final numbers fell a bit short (22%). Twenty-seven percent of participants self-identified as a member of a minority group. Retention was notably high in all groups, with more than 80% of all subjects completing at least two full study years.
Participants randomized into the control group attended one educational meeting regarding weight maintenance. Those in either of the other two study arms had more active interventions. Both the small- and large-change groups began with 10 in-person meetings with “interventionists,” all of whom had master’s level education in nutrition, psychology, or exercise physiology. These meetings occurred face-to-face over four months, with follow-up meetings online. Participants were introduced to the concept of self-regulation with an identified goal of keeping at or below baseline weight. All were encouraged to weigh themselves daily and submit results electronically. Monthly feedback was provided via email with either reinforcement or corrective strategies and/or an option for more personalized assistance if weight had increased above baseline.
The corrective strategies differed between the two active intervention groups. Those in the small-change group were given pedometers and asked to add about 2,000 steps each day, reduce portion sizes, cut down on sugar-filled drinks, and make small incremental changes in physical activity. If weight started to rise above baseline, they were encouraged to implement other small, daily changes.
Those randomized into the large-change group focused more on large, periodic changes. During the first four months of the study, the authors introduced a goal of creating a weight loss “buffer zone” to protect against the weight gain expected with aging. To achieve this, calorie restriction (500-1,000 kcal from baseline daily) was promoted for the first two months and was prescribed again if weight exceeded baseline later in the study. Moderate-intensity activity to 250 minutes/week was encouraged throughout the entire study.
Assessments were completed at baseline, month 4, month 12, month 24, and, for a portion of the participants (depending on timing of entrance), months 36 and 48.
The primary outcome studied was mean weight change. (See Table 1.)
Table 1: Mean Weight Changes |
||||
|
Mean weight change over mean of 3 years |
Standard error |
P value relative to control |
P value relative to small-change group |
|
|
Control |
0.26 kg |
0.22 |
||
|
Small-change |
-0.56 kg |
0.22 |
0.02 |
|
|
Large-change |
-2.37 kg |
0.22 |
< 0.001 |
< 0.001 |
Secondary outcomes were a weight gain of 0.45 kg or more and development of obesity. Although the large-change group was more successful at mean weight loss than either the control or small-change group, both the small- and large-change group participants displayed a reduced incidence of obesity of nearly 50% relative to control. (See Figure 1.)
Figure 1: Development of Obesity During Follow-up (%) |
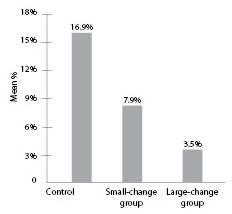 |
COMMENTARY
In a recent series of articles, The New York Times asked: Why Do Obese Patients Get Worse Care? Their answer: Many Doctors Don’t See Past the Fat.5 Although The New York Times may have a valid point, in its exploration of the medical difficulty of treatment for obesity they left out the subject of prevention. This is not a surprise, as the medical field has widely neglected this aspect of obesity treatment as well.
In 2008, the Council of the Obesity Society published a white paper regarding obesity as a disease.6 The discussion in the paper concluded: “It seems that considering obesity a disease is likely to have far more positive than negative consequences and benefit the greater good by soliciting more resources into research, prevention, and treatment of obesity; by encouraging more high-quality caring professionals to view treating the obese patient as a vocation worthy of effort and respect; and by reducing the stigma and discrimination heaped upon many obese persons.”
SNAP was designed to look primarily at how to prevent weight gain and, as such, represents a valuable contribution to our knowledge of the field of obesity treatment. Recall that just over 50% of all participants in this study had a BMI > 25 kg/m2. BMI is a screening tool that may be used to detect obesity and is determined by dividing total body weight in kilograms by height squared in meters.7 Results of BMI are placed into general categories (some of which may be further subdivided) as follow:
Underweight: < 18.5 kg/m2
Normal weight: 18.5-24.9 kg/m2
Overweight: 25-29.9 kg/m2
Obesity: ≥ 30 kg/m2
One of the valuable contributions of this study is that both normal weight and overweight participants were involved, making it truly a prevention rather than a weight loss study. Given the rising medical costs associated with treatment of the obese and growing concerns about an epidemic of obesity,8 identifying interventions to attack obesity in the arena of prevention (as we do with other chronic disorders) seems a necessary and crucial step in tackling this condition.
Self-monitoring or self-weighing to avoid weight gain is a familiar concept to most adults. Application of specific self-regulation strategies to prevent weight gain is a more nuanced concept akin to the more familiar role of self-regulation in medical disorders, such as diabetes and asthma.
Self-regulation depends on identification and internalization of a goal. In this study, all participants were recruited through mailings looking for young adults with an interest in weight control. All subjects entered the study with a shared goal. This is useful for implementation of self-regulation, but certainly may have led to selection bias. Replicating this study with a more randomized group and with more diverse recruitment tools is essential before applying any conclusions from the results to the population as a whole.
Bridging the gap from an interesting study to clinical implementation often is challenging. In this case, it is pertinent to wonder if a practitioner has enough solid evidence from this study to encourage young, healthy adults to adopt self-regulation of weight strategies; if so, what would this look like in a clinical setting? The evidence points to the efficacy of self-weighing only when linked with the rest of the feedback loop (reporting of weight and corrective action or reinforcement of success) — there is no evidence or implication from this study that self-weighing divorced from the remainder of the interventions is helpful or if any one step is critical for weight gain prevention. Clearly, this is an area for further research.
Further studies to clarify the sustainability of the interventions over time also are needed. Although a goal of keeping off pounds during young adulthood is significant, continuing this trend throughout a lifetime is the ultimate goal when looking at obesity risks and health.
Likewise, it would be useful to know if any of the participants moved from the overweight to normal weight category (as determined by BMI) during the study period. These statistics were not examined in this paper, but may be helpful to obtain in future investigations to more fully understand the effect of interventions on weight control.
For now, a practitioner is on firm ground in reminding young, healthy patients about the potential for weight gain in early adulthood. There is much to be gained and little risk in encouraging patients to adopt a habit of self-monitoring weight and to develop compensatory strategies when needed; these very well may be valuable tools in preventing obesity and may convey lifelong health benefits. Although this study suggests a role for self-regulation in prevention of weight gain, future studies looking closely at each element of intervention are necessary to give patients definitive answers and strategies to combat weight gain associated with aging.
REFERENCES
- National Heart, Lung, and Blood Institute. Preventing Weight Gain in Young Adults. Available at: https://www.nhlbi.nih.gov/research/reports/2005-weight-gain. Accessed Oct. 23,2016
- Williamson DF, Kahn HS, Remington PL, Anda RF. The 10-year incidence of overweight and major weight gain in US adults. Arch Intern Med 1990;150:665-672.
- National Heart, Lung, and Blood Institute. Study of Novel Approaches for Prevention (SNAP). Available at: http://www.nhlbi.nih.gov/research/resources/obesity/trials/snap.htm. Accessed Oct. 23, 2016
- Leventhal H, Leventhal EA, Contrada RJ. Self-regulation, health and behavior: A perceptual-cognitive approach. Psychol Health 1998;13:717-733.
- Kolata G. Why Do Obese Patients Get Worse Care? Many Doctors Don’t See Past the Fat. The New York Times Sept. 25, 2016.
- Allison DB, Downey M, Atkinson RL, et al. Obesity as a disease: A white paper on evidence and arguments commissioned by the Council of the Obesity Society. Obesity 2008;16:1161-1177.
- National Heart, Lung, and Blood Institute. Calculate Your Body Mass Index. Available at: http://www.nhlbi.nih.gov/health/educational/lose_wt/BMI/bmicalc.htm. Accessed Oct. 23, 2016.
- Cawley J, Meyerhoefer C. The medical care costs of obesity: An instrumental variables approach. J Health Econ 2012;31:219-230.
Specific self-regulation techniques are shown to be effective at preventing weight gain in young adults.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
