Soy and Breast Cancer: Harmful or Helpful?
Soy and Breast Cancer: Harmful or Helpful?
By David Kiefer, MD
The food and supplement known as soy, or soybean (Glycine max, Family Fabaceae), has quite the reputation in lay and scientific circles for many health conditions, including cancer prevention, bone health, cardiovascular disease prevention, and, most notably, treatment of menopausal symptoms. The primary mechanism of action of soy is thought to be mostly due to the phytoestrogenic isoflavone compounds genistein and daidzein, and less so biochanin A and formononetin; red clover (Trifolium pretense, Family Fabaceae), on the other hand, is a menopausal herb with the reverse proportion of these compounds, containing primarily biochanin A and formononetin.1,2,3
The presence of “phytoestrogens” in soy raises questions about its safety in women with breast cancer, with a history of breast cancer, or at high risk of breast cancer; at the same time, there is some research supporting soy’s anticancer effects. It can be difficult for a clinician to know how to counsel patients about this topic. And, the need for such counsel is not rare; one study found that soy food and supplement intake is common in women recently diagnosed with breast cancer.4 An extensive literature already exists examining the clinical use of soy, and in most of those individual studies some comment was made about adverse effects in the treatment groups. This review will instead focus on some of the recent trials specifically looking at the safety of soy in breast cancer.
Mechanism of Action
Some insight into the possible effects of soy in people at risk for hormone-sensitive cancers comes with a more detailed look at the mechanism of action of the isoflavone compounds. Soy isoflavones are diphenolic compounds with a structure similar to estrogen; these compounds bind to the estrogen receptors ER α and ER β, and may either have agonist or antagonist activity, depending on the isoflavone concentration and the tissue involved.2,3,5,6 At the same time that anticarcinogenic effects have surfaced in research results, soy isoflavones seem to be “weak estrogens” and, in animal trials, promote the proliferation of breast tissue.3,6 Hence, there is some contradiction in the in vitro scientific literature.
Figure 1. Genistein and Estrogen
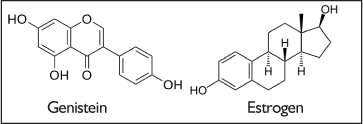
Clinical Trials
There are many factors to consider in clinical trials about soy and breast cancer, and the details about this inter-relationship have not been fully worked out.3 The length of the trial, the dose and source of soy, and the demographic being studied are some of the important variables that have been found to be significant in the published literature. For example, with respect to women’s demographic, the treatment of Asian Americans as either part of a “Western” cohort or an Asian cohort may be a crucial decision that has probably affected meta-analyses in the past.2 Although many interesting individual clinical trials exist on this topic,7 this review will focus on meta-analyses and scientific review articles.
One review on the epidemiology and biochemistry of soy and soy isoflavones sheds some light on soy risks and benefits.5 Researchers analyzed studies on soy consumption and breast cancer recurrence rates and mortality, finding, at an intake level approximating the typical Asian diet, no evidence of increased breast cancer recurrence risk. In fact, many studies have shown a decrease in risk, although there are nuances. For example, it may be that HER-2 negative patients and women at increased risk of breast cancer because of genetic polymorphisms will respond more favorably to soy intake. In addition, soy isoflavone intake greater than 225 mg daily may lead to increase breast epithelial cell proliferation in high-risk, premenopausal women. The information for these subset groups is based on low numbers of research subjects and needs to be replicated, but such detail is clearly important clinically and warrants further attention.
A meta-analysis of prospective trials aimed to improve on other reviews that emphasized case-control studies.6 This meta-analysis included 18 studies that investigated the dietary consumption of soy isoflavones (from 0 to 33.9 mg daily) as it related to breast cancer incidence or recurrence. There were 14 studies that analyzed breast cancer incidence; the researchers found a 11% decrease (relative risk [RR], 0.89; 95% confidence interval [CI], 0.79-0.99) when the highest isoflavone intake was compared to the lowest isoflavone intake, although there was a lot of heterogeneity in this part of the analysis which could have compromised the results. There were four studies of breast cancer recurrence; a 16% reduction was noted in the highest vs lowest isoflavones (RR, 0.84; 95% CI, 0.70-0.99, no significant heterogeneity). When these data were stratified, the results were only significant for Asian and postmenopausal women, showing a lack of statistically significant differences from highest to lowest isolfavone intake for Western populations and premenopausal women. It is possible that the lack of findings in Western populations is merely due to dietary soy intake, given that the highest Western intake is below the lowest Asian intake, although the authors also hypothesize that, in line with other research results, the protective effect of early soy intake may play an important role. However, there is some controversy about these benefits for Asian populations but not for Western populations. For example, one meta-analysis of Chinese vs U.S. cohorts of breast cancer survivors found that an intake of at least 10 mg of isoflavones daily led to improvements in all-cause and breast cancer mortality in both groups.8 Methodology, as well as demographics (breast cancer prevention, as opposed to prevention of breast cancer recurrence), might account for these divergent results.
Research has also been undertaken to determine the effect of genistein, and sometimes whole soy, in breast cancer survivors, finding either no increased risk or a decreased risk of recurrence.2 More research is needed to clarify the effects of isolated isoflavones as compared to whole soy foods (Western soy products and traditional Asian foods) or supplements.
These reviews are reassuring; some concerning results from earlier reviews possibly indicated adverse hormonal effects as seen by endometrial hyperplasia (but no cancer) with 150 mg of soy extract daily over 5 years.1,9 However, the story is anything but clear, and will continue to require clinicians’ vigilance in following the medical literature as new studies are published. For example, one 6-month study randomized 126 healthy women with a family history of unilateral breast cancer to soy isoflavones (150 mg genistein and 74 mg daidzein) or placebo and found (via fine needle aspiration of breast epithelium and nipple aspiration fluid) no decrease in overall cell proliferation, though there was an increase in cell proliferation for the premenopausal group.10 The authors claim that this hints at a lack of preventive effects for soy in breast cancer and possibly a risk for premenopausal women. However, a complete interpretation of these results is complicated and anything but clear; other researchers have pointed out numerous issues with this study, including the menstrual timing of the data collection that could have affected the results, and a possible failure of randomization.11
Finally, as alluded to above, the timing of soy intake may be very important; much of the protection that soy exhibits for breast cancer development seems to stem from the intake of soy during early childhood and adolescence.2,3
Dose Relevant to Breast Cancer
The safest and most effective dose of soy remains to be determined. Most clinical trials use dosages from 50-100 mg of isoflavones daily.9 Some researchers mention that 80-120 mg of isoflavones yields the “greatest effect with a positive safety profile,” noting the need for long-term data.1 As a reference, the isoflavone consumption in Southeast Asian countries approximates 20-50 mg daily, compared to less than 1 mg daily in Western countries.5
Conclusions and Challenges
Contrary to some findings in in vitro research and animal models, the vast majority of human research, including prospective and retrospective clinical trials, shows no increased risk for women with or at risk of breast cancer. There are caveats that need to be further elucidated, including the genetic contribution to soy risk and benefit and demographic differences (especially Asian vs Western living or born). It is becoming more and more clear that early and continued exposure to soy, as with the typical Asian diet, may explain a significant portion of the cancer protective effects of soy. Furthermore, menopausal status is important with some of the intervention studies, showing that soy intake may be most useful during the postmenopausal years rather than premenopausal age groups. Nonetheless, there are numerous challenges to interpreting the medical literature about soy; in addition to the many types of soy foods, there are numerous products and formulations, which are not always labeled with respect to isoflavone content,9 making it difficult to firmly establish cause-effect for soy intake. In addition, carcinogenesis is not an overnight phenomenon; cancer takes years to develop and, in most research, the trials are short-term enough to compromise the formation of definitive hypotheses about soy’s adverse effects.
Recommendations
Based on the current state of science regarding soy and cancer, only a few basic clinical recommendations can be made. There are too many variables that remain to be fully explored to make generally applicable statements about soy. The research points to benefits for an early introduction of soy foods (the best data are for soy foods found in traditional Asian cuisine), and regular soy intake throughout life. Does this hold for all women, even those at high-risk of breast cancer (such as a strong family history)? Possibly, though it seems prudent to wait and receive irrefutable proof of benefit in that demographic. The medical community should be wary of recommending concentrated soy supplements in “high doses,” the specifics of which are starting to accumulate, and favor, instead, isoflavone doses in line with traditional consumption patterns. This is a very exciting area; the realm of diet and cancer proves to continue to provide clinicians with important areas of intervention for patients. With respect to soy, many of these details are coming together.
References
1. Geller SE, Studee L. Soy and red clover for mid-life and aging. Climacteric 2006;9:245-263.
2. Hilakivi-Clarke L, et al. Is soy consumption good or bad for the breast? J Nutr 2010;140:2326S-2334S.
3. Andres S, et al. Risks and benefits of dietary isoflavones for cancer. Crit Rev Toxicol 2011;41:463-506.
4. Boucher BA, et al. Intake of phytoestrogen foods and supplements among women recently diagnosed with breast cancer in Ontario, Canada. Nutr Cancer 2012;64:695-703.
5. Magee PJ, Rowland I. Soy products in the management of breast cancer. Curr Opin Clin Nutr Metab Care 2012;15:586-591.
6. Dong JY, Qin LQ. Soy isoflavones consumption and risk of breast cancer incidence or recurrence: A meta-analysis of prospective studies. Breast Cancer Res Treat 2011;125:315-323.
7. Kang HB, et al. Study on soy isoflavone consumption and risk of breast cancer and survival. Asian Pac J Cancer Prev 2012;13: 995-998.
8. Nechuta SJ, et al. Soy food intake after diagnosis of breast cancer and survival: An in-depth analysis of combined evidence from cohort studies of US and Chinese women. Am J Clin Nutr 2012;96:123-132.
9. Low Dog T. Menopause: A review of botanical dietary supplements. Am J Med 2005;118 (Suppl 12B):98-108.
10. Khan SA, et al. Soy isoflavone supplementation for breast cancer risk reduction: A randomized phase II trial. Cancer Prev Res 2012;5:309-319.
11. Wu AH, et al. Soy isoflavones for breast cancer risk reduction. Cancer Prev Res (Phila) 2012;5:984-985.
The food and supplement known as soy, or soybean (Glycine max, Family Fabaceae), has quite the reputation in lay and scientific circles for many health conditions, including cancer prevention, bone health, cardiovascular disease prevention, and, most notably, treatment of menopausal symptoms.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
